 Nasal vaccine. Credit: Wikimedia Commons
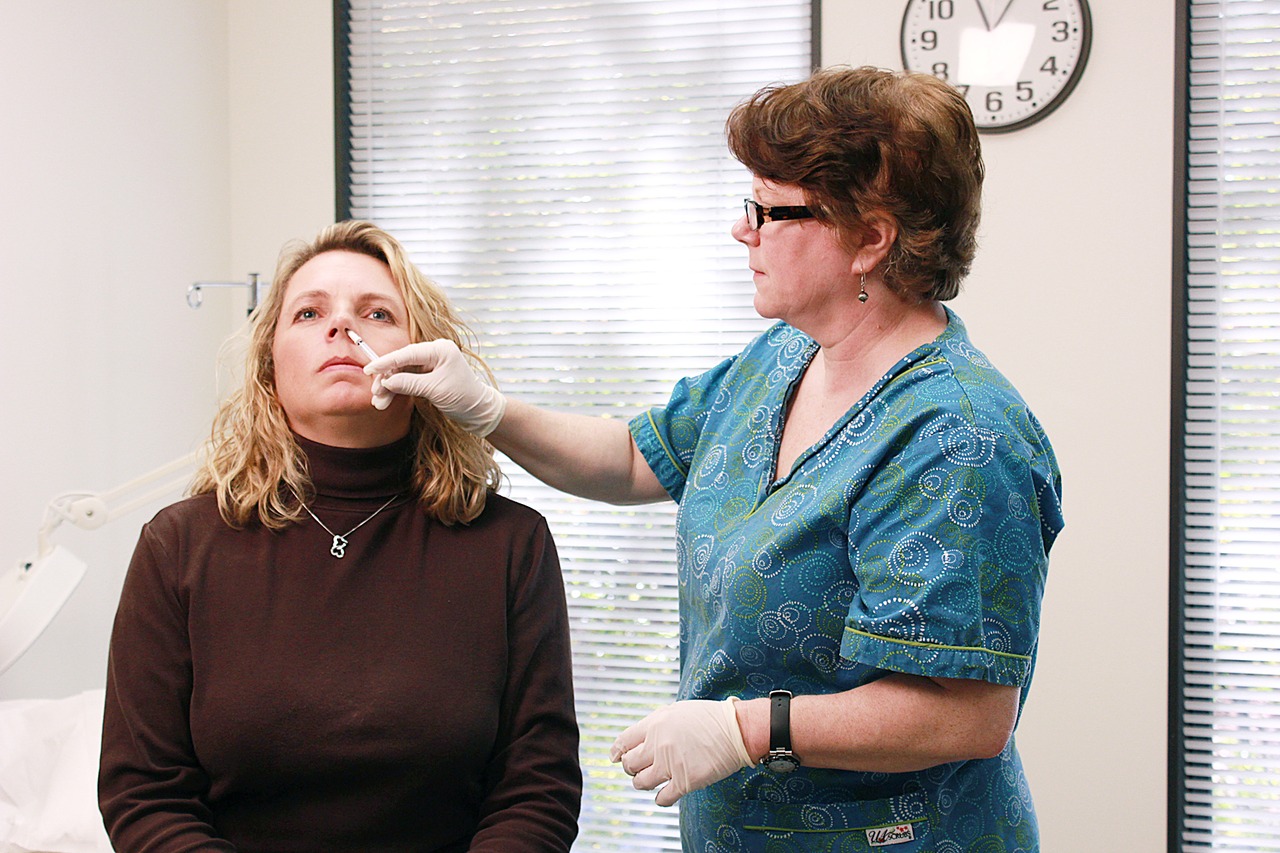
Nasal vaccine. Credit: Wikimedia Commons
Stanford University researchers are testing a bold new idea: instead of teaching the body to recognize one specific virus, why not prepare the lungs to react to almost anything? In early experiments, a new nasal vaccine candidate protected mice against a wide array of respiratory threats, from COVID-19 to bacterial infections.
Reporting in the journal Science, the team found the approach provided broad, durable protection for at least three months. It wasn’t just effective against SARS-CoV-2; it also held the line against Staphylococcus aureus (a common cause of pneumonia) and even lab-simulated allergens.
Lung Firewall
Most vaccines work like a “wanted” poster. They show the immune system a specific feature of a microbe so it can recognize the real thing later. That strategy has saved millions of lives, but it has a glaring weakness: if the virus mutates—or a totally new one emerges—the immune system is caught off guard.
Bali Pulendran, an immunologist at Stanford University and senior author of the study, told GEN that the new work is “conceptually, a very different approach” from the one-bug-at-a-time method that has guided vaccinology for over a century.
In the new study, researchers tried to mimic the signals the body produces during infection. Instead of focusing on a single target, the researchers used tiny lipid particles to deliver compounds that trigger the immune system’s early warning sensors. They also included a harmless egg protein called ovalbumin to help generate specialized immune cells that stay resident in the lungs.
The results were striking. The vaccine essentially “reprogrammed” macrophages—the white blood cells that patrol the tiny air sacs in our lungs. Once reprogrammed, these cells became far more efficient at spotting invaders and launching a rapid antiviral response.
“What makes this study stand out,” says Prof. Daniela Ferreira, a vaccinologist at the University of Oxford, “is that a nasal vaccine was able to rapidly generate T cells that reprogrammed the lungs to protect against a broad range of infections—even germs the body hadn’t seen before.”
Still a Way To Go
Scientists have long tried to build vaccines that protect against more than a single virus. Most “universal vaccine” efforts still focus on one family (such as influenza or coronaviruses) by aiming at parts of the virus that rarely change. The new study takes a different approach. Instead of targeting one pathogen, it tries to keep the lungs in a ready state so they can respond quickly to multiple threats.
×
Thank you! One more thing…
Please check your inbox and confirm your subscription.
But while the “lung firewall” concept is promising, we aren’t there just yet.
The first step is ensuring it works in humans; the second is ensuring it doesn’t cause major side effects.
“We have to ensure that keeping the body on ‘high alert’ doesn’t lead to friendly fire,” warns Prof. Jonathan Ball of the Liverpool School of Tropical Medicine. The risk is that a hyper-ready immune system could accidentally trigger chronic inflammation or other side effects.
There are practical hurdles as well. In the study, mice received drops of the vaccine in their noses. Delivering a similar treatment deep into human lungs may prove more difficult, and it is not yet clear how long protection might last.
For now, the results show what might be possible. If the approach works in people, vaccines might someday act more like a standing guard in the lungs—ready for whatever shows up next.