Science no longer views the mind as an isolated chemical factory disconnected from the body’s internal ecology. Recent breakthroughs in nutritional psychiatry reveal a complex, bidirectional highway where your digestive health dictates your cognitive clarity. While genetics and environment set the stage, balanced nutrition supports mental wellness within your gut by serving as a primary conductor for mood regulation and stress resilience.
Clinical insights into the gut-brain axis prove that food functions as a biological signal rather than simple fuel. Short-chain fatty acids and neurotransmitter precursors, produced by specific bacterial taxa, travel directly to the brain to modulate inflammatory responses. Shifting your dietary patterns creates a measurable impact on systemic inflammation, effectively altering the biological theater where emotional processing occurs.
Assembling a psychobiotic plate provides a tangible method for supporting long-term mental wellness. You can leverage prebiotic fibers, fermented nutrients, and polyphenols to cultivate a microbiome that fosters wisdom-related traits and emotional stability. Focus remains on the intersection of data-driven nutrition and psychological health to ensure your dietary choices support a resilient, high-functioning mind.
Peer through the current data to see what the evidence truly supports, pinpoint where uncertainty remains, and learn to assemble a realistic food pattern—the psychobiotic plate. The goal is not hype. It is clarity.
 (Credit: Intelligent Living)
(Credit: Intelligent Living)
Gut Microbiome and Mental Health: Mapping the Clinical Evidence
 (Credit: Intelligent Living)
(Credit: Intelligent Living)
How Gut Microbiome Diversity and the Gut-Brain Axis Shape Wisdom and Emotional Regulation
The Science of Wisdom: Quantifying Emotional Regulation and Gut Diversity
In everyday language, wisdom sounds abstract. In research settings, it is measured.
Psychologists utilize a specialized scale to quantify wisdom-related traits, allowing researchers to measure internal capacities through a validated framework.
Specific attributes measured include:
Emotional regulation and impulse control
Compassion and altruism
Self-reflection and internal awareness
Tolerance of diverse perspectives
Pro-social behavior
While emotional regulation empowers you to pause rather than react, compassion strengthens social bonds, and self-reflection sharpens long-term decision-making. When mental illness disrupts mood stability or stress regulation, these capacities can decline.
Exploratory research has linked loneliness to gut microbial diversity in community-dwelling adults, revealing how biological markers and psychological well-being are deeply intertwined. These gut microbes shape loneliness and wisdom by influencing the neurological pathways responsible for social connection.
Study results do not prove causation, but they suggest that biological and psychological dimensions of well-being may be more interconnected than previously assumed.
The Gut-Brain Communication Layer (How Food Becomes Mental Signal)
The gut and brain communicate through multiple pathways. Bidirectional systems like the gut-brain axis rely on sweet taste receptors to signal metabolic health, alerting the brain to incoming nutrients and potential inflammatory triggers.
Short-Chain Fatty Acids and Immune Signaling
Gut bacteria ferment dietary fiber and produce short-chain fatty acids such as butyrate. These compounds influence immune cells, intestinal barrier integrity, and inflammatory signaling. Chronic low-grade inflammation has been observed in a subset of individuals with depression, and a meta-analysis on low-grade inflammation suggests that roughly a quarter of patients show elevated inflammatory markers.
Dietary Patterns and Microbial Balance
Dietary choices directly shape which bacterial taxa thrive within your system. Specific habits support gut health by protecting the delicate microbial balance from small, accumulating choices that might otherwise undermine metabolic stability. Diets rich in diverse plant fibers, legumes, nuts, seeds, and fermented foods tend to support greater microbial diversity. Diets dominated by ultra-processed products can displace fiber and introduce additives that may alter metabolic responses.
Data from large-scale psychiatric analyses reveal striking patterns across various disorders, specifically the depletion of protective butyrate-producing taxa and the surge of pro-inflammatory genera. Biological signatures detailed in clinical reviews suggest a shared gut-based framework for mental health.
Biological complexity prevents any simple claim that microbes cause mental illness. Research suggests that food influences biological signals that interact with stress response systems, immune tone, and potentially neurotransmitter pathways.
 (Credit: Intelligent Living)
(Credit: Intelligent Living)
Building a Psychobiotic Diet from Clinical Trial Evidence to Everyday Plate Design
Clinical Success in Nutritional Psychiatry: Outcomes from Randomized Trials
Nutritional psychiatry is grounded in clinical trials, not just theory, and identifying how anxiety tracks with microbiome changes helps translate complex lab findings into everyday mental health strategies.
Adults with major depressive disorder enrolled in the SMILES trial received assignments to either structured dietary support or social groups. After 12 weeks, the dietary intervention group showed significantly greater improvement in symptoms. Evidence regarding gut bacteria linked to depression further suggests that these clinical changes align with parallel biological shifts in the microbiome. Trial data indicate a clinically meaningful effect size for some participants.
A 2025 meta-analysis pooling five randomized controlled trials of Mediterranean-style dietary interventions found moderate improvements in depressive symptoms overall, although researchers emphasized substantial heterogeneity and the need for larger studies.
Clinical findings emphasize that dietary shifts serve as an adjunct, rather than a replacement, for therapy or medication.
The Psychobiotic Plate (Fiber Plus Ferments Plus Polyphenols)
The term “psychobiotic” describes dietary patterns or microbes that influence mental health through the gut-brain axis.
In one randomized controlled study, participants assigned to a psychobiotic-style diet emphasizing prebiotic fibers and fermented foods reported reductions in perceived stress over four weeks. Further evidence from a fermented food intervention study shows that these diets increase microbiome diversity and reduce inflammatory proteins. These fermented nutrients support gut health by providing the specific substrates necessary for high-level microbial signaling.
Fiber intake is foundational. Many dietary guidelines recommend approximately 14 grams of fiber per 1,000 calories consumed, which translates to about 25 grams per day for women and 38 grams per day for men. A comprehensive review of fiber intake explains why grains affect blood sugar and gut health in ways that directly impact your risk for chronic psychiatric conditions.
Constructing a practical psychobiotic plate involves selecting ingredients that maximize the diversity of your gut ecology. Focus on whole, nutrient-dense options that provide the substrates necessary for bacterial fermentation and neuro-signaling.
Core Components of a Psychobiotic Diet
Optimal choices for your plate include:
Fiber-rich legumes and steel-cut oats
Polyphenol-packed berries and leafy greens
Healthy fats from nuts, seeds, and olive oil
Probiotic staples like yogurt, kefir, sauerkraut, and kimchi
Consistency remains more valuable than perfection in these selections. Regularly including a wide variety of plant foods ensures your gut receives the broad spectrum of nutrients required to sustain mood stability and mental clarity.
 (Credit: Intelligent Living)
(Credit: Intelligent Living)
From Ultra-Processed Risk to Precision Psychobiotics in Personalized Mental Health Nutrition
Ultra-Processed Foods as a Risk Multiplier (The Reduce First Move)
Ultra-processed foods are industrial formulations that often contain refined starches, added sugars, industrial fats, emulsifiers, colorings, and flavor enhancers.
Industrial formulations tend to be energy-dense and fiber-poor. An umbrella review in The BMJ found consistent associations between higher consumption of ultra-processed foods and increased risk of numerous adverse health outcomes, including common mental disorders.
Observational data cannot prove causation, but the consistency across large datasets strengthens global health concerns. This risk linked to ultra-processed foods underscores the urgent need for whole-food alternatives.
Microbiome perspectives reveal that replacing whole plant foods with ultra-processed products reduces fermentable fiber and alters nutrient density. Reducing ultra-processed intake serves as one of the most accessible first steps toward improving gut-derived signals and avoiding foods that trigger anxiety.
Precision Nutrition for the Mind (Why One-Size-Fits-All Fails)
Biological individuality ensures that responses to dietary changes vary significantly across populations. Baseline microbiome composition, medication use, sleep quality, stress exposure, metabolic health, and genetic factors all influence outcomes.
Outcomes depend on a shifting mosaic of factors that define individual health. Key determinants include:
Baseline microbiome composition and current medication use
Sleep quality and chronic stress exposure
Metabolic health and genetic predispositions
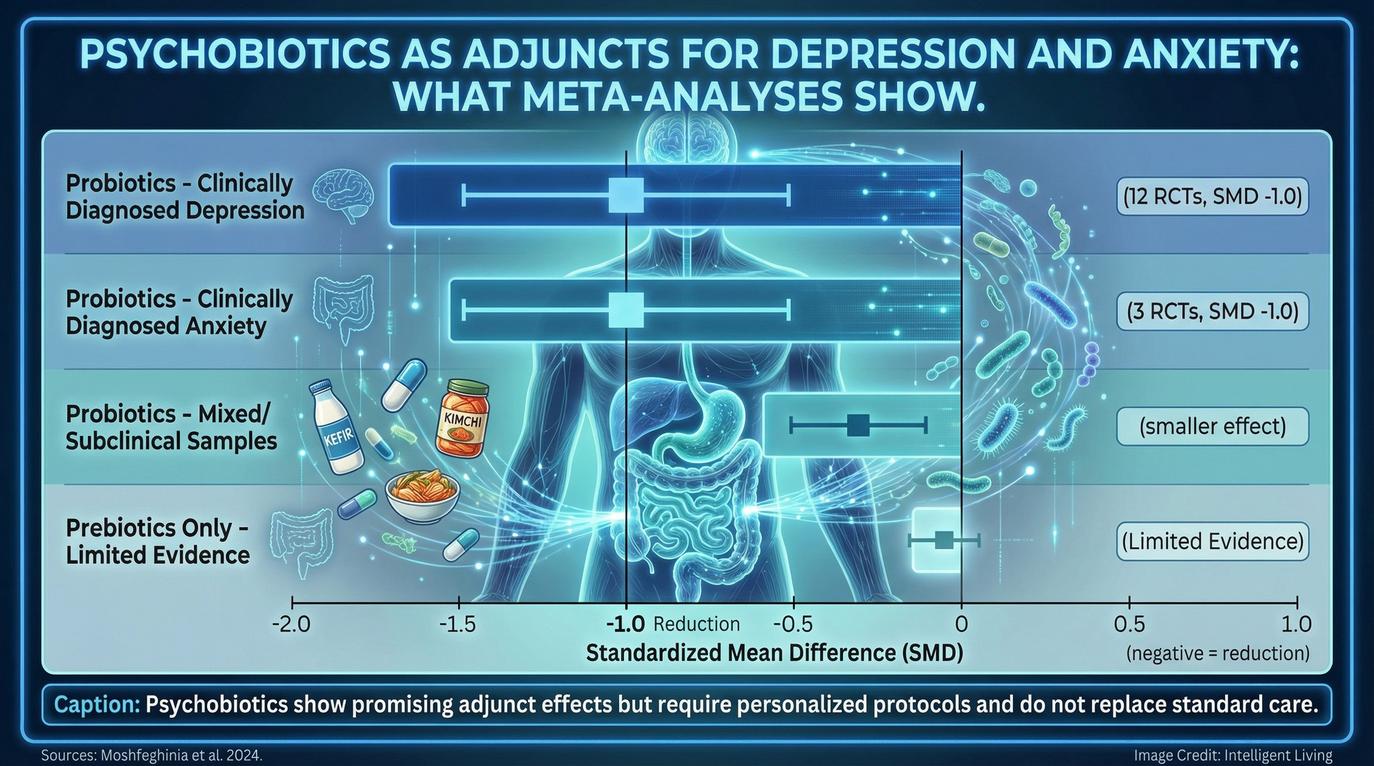
Meta-analyses examining probiotics for depressive and anxiety symptoms report modest benefits on average, but with wide variability across individuals and strains. Consistent variability underscores the critical need for data-driven nutrition science to tailor individual protocols. A psychobiotic pattern should be adapted gradually and discussed with a healthcare professional when significant symptoms or medical conditions are present.
Psychobiotics is Frontier Science
Testing causal relationships between gut microbiome composition and severe psychiatric disorders now involves advanced genetic methods like Mendelian randomization. One recent study on the microbiome and schizophrenia integrated large-scale genetic datasets and identified small but statistically significant associations for specific taxa.
Preliminary findings do not constitute treatment guidance. Genetic research illustrates how the field is moving from correlation toward causal testing.
 (Credit: Intelligent Living)
(Credit: Intelligent Living)
Systemic Inflammation and Brain Aging: The Sociobiome Connection
Brain Aging and Cognitive Clarity
Long-term dietary patterns also intersect with cognitive aging. In the PREDIMED trial, older adults assigned to Mediterranean diet patterns supplemented with extra virgin olive oil or nuts showed improved cognitive scores compared to controls over several years. Similar findings show how a prebiotic fiber supplement boosted memory in older adults by supporting gut-brain signaling.
A more recent trial of prebiotic supplementation and cognition in healthy older twins reported that targeted prebiotics improved certain cognitive measures compared to a placebo.
The Sociobiome: When Environment Becomes Biology
Diet does not exist in isolation. Sociobiome perspectives reframe mental health as both personal and structural, recognizing that food choices matter alongside food systems and social conditions.
Microbiome composition reflects a complex interplay of environmental and social stressors. Key contributors to this “sociobiome” include:
Socioeconomic status and regional food security
Chronic stress levels and environmental exposures
Neighborhood-level food access and community design
Recent research on socioeconomic status and the microbiome has identified associations between these neighborhood-level factors and gut microbial diversity.
Inflammation as the Shared Currency
Low-grade systemic inflammation functions as a primary biological currency linking diet, microbiome health, and mental well-being. Structural views offer a measurable biological lens for tracking change and explaining how inflammation blunts dopamine and reduces internal motivation.
Researchers track this state using C-reactive protein (CRP) markers:
Low Risk: Below 1 milligram per liter
Moderate Risk: 1 to 3 milligrams per liter
High Risk: Above 3 milligrams per liter
Understanding inflammation as a shared currency does not simplify mental illness into a single pathway, but it does offer a robust metric for clinical observation.
 (Credit: Intelligent Living)
(Credit: Intelligent Living)
Building a Gut-Healthy Diet for Mental Clarity and Emotional Resilience
Your microbiome isn’t destiny—it is a dynamic layer within a vast network of behavior, environment, and medical care.
Emotional well-being involves a complex interplay of therapy, social support, restorative sleep, and intentional movement. Nutrition is one lever among many, and specific steps to support gut health help translate this science into daily habits.
Robust clinical evidence indicates that improving diet quality, increasing plant fiber diversity, and incorporating fermented foods directly support healthier gut microbiome patterns. Evolutionary shifts in eating habits help maintain a healthy weight while reducing depressive symptoms for some individuals when used alongside standard care.
Nutrition actively shapes the biological theater where your thoughts, emotions, and decisions take center stage. Adaptive habits work alongside lifestyle changes that improve clarity to foster long-term resilience.
Psychobiotic Foundations: Frequently Asked Questions
1. How Does Nutritional Psychiatry Impact Daily Mood?
Targeted dietary shifts influence the production of neurotransmitters and anti-inflammatory compounds in the gut, providing a biological boost to emotional regulation.
2. Which Foods Best Support the Gut-Brain Axis?
Prioritize prebiotic fibers like oats and legumes alongside fermented staples like kefir and kimchi to maximize microbial diversity and signaling.
3. Can a Psychobiotic Diet Reduce Systemic Inflammation?
Consistent intake of polyphenols and high-fiber plants lowers inflammatory markers like C-reactive protein, which are often elevated in psychiatric conditions.
4. How Quickly Does the Microbiome Respond to Diet Changes?
Microbial shifts begin within days of introducing new plant fibers, though clinical improvements in mood typically manifest over four to twelve weeks.
5. Why Is Reducing Ultra-Processed Food Essential for Mental Clarity?
Industrial additives and refined sugars trigger pro-inflammatory pathways that disrupt gut-brain communication and may exacerbate symptoms of anxiety or depression.







