In a groundbreaking development that promises to reshape the landscape of cancer immunotherapy, researchers have uncovered a novel mechanism to dramatically enhance the efficacy of CAR-T cell treatments against solid tumors. This discovery centers on the deletion of the nuclear receptor NR2F6, a previously underexplored molecular checkpoint, which has been shown to revive the fatigued functionality of CAR-T cells and foster an unprecedented form of antigen-agnostic immune memory. These findings, recently published in Nature Communications, could herald a new era of cellular immunotherapies capable of overcoming the immunosuppressive microenvironments that have long hindered success in solid malignancies.
Chimeric Antigen Receptor T-cell (CAR-T) therapy has revolutionized treatment modalities for hematologic cancers, yielding remarkable remission rates in conditions such as acute lymphoblastic leukemia and certain lymphomas. Despite these successes, the extension of CAR-T therapies to solid tumors has been stymied by multiple barriers, including tumor heterogeneity, antigen escape, and an immunosuppressive tumor microenvironment that impedes T cell persistence and functionality. The study spearheaded by Humer, Klepsch, Rieder, and colleagues delineates a transformative strategy focused on NR2F6 deletion to surmount these obstacles and unleash the full therapeutic potential of CAR-T cells in solid cancer contexts.
NR2F6, a member of the nuclear receptor superfamily, functions as an intracellular immune checkpoint that negatively regulates T cell activation and effector functions. Unlike classical immune checkpoints such as PD-1 or CTLA-4 which interact at the cell surface, NR2F6 modulates transcriptional programs within T cells, fine-tuning their response thresholds. Importantly, the inherent regulatory role of NR2F6 in dampening immune responses suggested that its deletion might recalibrate T cell activation dynamics, enabling more robust and sustained antitumor activity without exacerbating autoimmunity.
The researchers employed sophisticated gene-editing techniques to excise NR2F6 specifically in engineered CAR-T cells targeting diverse solid tumor antigens. This genetic manipulation induced a phenotypic rejuvenation of exhausted CAR-T cells, characterized by enhanced proliferation, increased cytokine secretion, and resistance to the suppressive metabolic cues prevalent within the tumor microenvironment. Intriguingly, these modified cells displayed profound cytotoxicity not only in antigen-positive tumor cells but also demonstrated cross-reactive killing capacity independent of the original CAR specificity, a phenomenon described as antigen-agnostic immune memory.
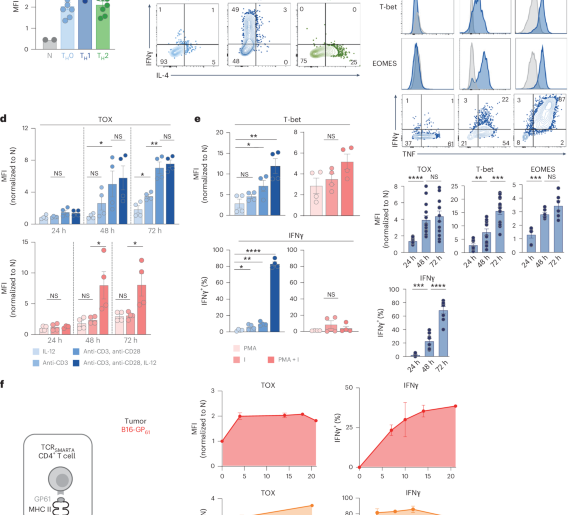
Mechanistically, NR2F6 deletion unleashed a transcriptional reprogramming within the CAR-T cells, elevating the expression of pro-inflammatory cytokines such as IFN-γ and TNF-α while suppressing inhibitory pathways linked to cellular exhaustion and metabolic dysregulation. This shift promoted a durable and self-amplifying immune response, enabling the CAR-T cells to adapt and recognize evolving tumor antigenic profiles that typically undermine single-target approaches. Such adaptability fundamentally challenges the paradigm of strict antigen dependency in CAR-T therapies and opens avenues for targeting highly mutable solid tumors notorious for antigenic heterogeneity.
Experimental in vivo models validated these insights, as NR2F6-deficient CAR-T cells achieved significant tumor regression and prolonged survival in murine models of aggressive cancers such as glioblastoma and pancreatic adenocarcinoma. Notably, treated subjects exhibited resistance to tumor rechallenge, underscoring the establishment of a long-lived, antigen-agnostic immune memory that could confer lasting protection against relapse. This discovery implicates NR2F6 as a critical modulator not only of immediate CAR-T cell functionality but also of their immunological memory potential, a feature previously elusive in engineered T cell therapies.
The safety profile of NR2F6 deletion was carefully evaluated, revealing no overt signs of systemic autoimmunity or off-target tissue damage, a crucial aspect given the amplified immune activation. The precise intracellular localization and selective expression pattern of NR2F6 likely mitigate risks associated with global immune perturbation, contrasting favorably with the potentially deleterious effects observed in broader checkpoint inhibition strategies. These findings underscore a sophisticated balance where enhanced antitumor efficacy is achieved without compromising immune homeostasis.
From a translational perspective, this work charts a roadmap for next-generation CAR-T cell design, integrating gene editing to remove intrinsic inhibitory checkpoints like NR2F6 alongside antigen targeting modules. Such combinatorial engineering could elevate response rates in solid tumors, expand therapeutic windows, and potentially reduce the need for high-dose conditioning regimens or adjunctive immunosuppression. Furthermore, this antigen-agnostic immune memory could simplify treatment paradigms by mitigating the necessity for precise tumor antigen identification and circumventing the problem of antigen escape variants.
The broader implications of NR2F6 deletion extend beyond CAR-T cells, hinting at utility across diverse immunotherapeutic platforms including TCR-engineered T cells and tumor-infiltrating lymphocytes. By enhancing T cell resilience and versatility, targeting NR2F6 could synergize with checkpoint blockade antibodies, cytokine therapies, or metabolic modulators to orchestrate multifaceted anti-tumor responses. The research community is poised to rapidly explore these combinatorial strategies to harness the full promise of immune system plasticity against cancer.
Intriguingly, this discovery catalyzes a shift in the conceptual framework surrounding immune checkpoint modulation, moving beyond extracellular receptor-ligand interactions to encompass nuclear receptor-mediated transcriptional control. Such a paradigm invites a richer understanding of T cell biology and uncovers novel nodes for therapeutic intervention that may transcend oncology and benefit autoimmune disorders or infectious diseases where immune regulation is paramount.
While the preclinical data are compelling, several challenges remain before this approach can be widely adopted clinically. The scalability and precision of CRISPR-based NR2F6 deletion must be optimized to ensure robust manufacturing of CAR-T products meeting regulatory standards. Long-term safety and efficacy will require comprehensive clinical trials, particularly to evaluate potential late-onset toxicities or the impact on endogenous immune compartments. Additionally, the interplay between NR2F6 modulation and other immunosuppressive elements in the tumor milieu warrants further elucidation to fine-tune therapeutic regimens.
Nevertheless, this landmark study ignites optimism that CAR-T therapy’s Achilles heel in solid tumors is surmountable. By co-opting the nuclear receptor NR2F6’s checkpoint function, scientists have engineered CAR-T cells that not only kill with renewed vigor but also ‘remember’ the enemy in a remarkably flexible and durable manner. This breakthrough stands to expand the arsenal of immunotherapies, offering hope to patients with refractory solid malignancies that have resisted conventional treatments.
In summary, the deletion of NR2F6 within CAR-T cells represents a paradigm-shifting innovation, enhancing their functional capacity, metabolic fitness, and memory capabilities against solid tumors. This antigen-agnostic immune memory could redefine therapeutic expectations and catalyze the development of more universally applicable and enduring cellular therapies. As this research moves from bench to bedside, it may unlock unprecedented opportunities in cancer immunology and beyond.
The authors’ meticulous elucidation of NR2F6’s role provides a compelling mechanistic basis for targeted immunomodulation and sets the stage for innovative clinical interventions. Continued interdisciplinary collaboration integrating molecular biology, immunology, and bioengineering will be essential to translate these insights into tangible patient benefits. The oncology community will undoubtedly watch eagerly as this promising avenue evolves into a new frontier in cancer treatment.
As CAR-T technology matures, the modulation of intracellular checkpoints heralds a new chapter where engineered cells can autonomously overcome tumor defenses and sustain immune vigilance over the long term. This transformative approach could concurrently simplify treatment regimens and broaden patient eligibility, ultimately propelling immunotherapy toward a future where durable remission of solid tumors becomes achievable for many.
Subject of Research: Enhancement of CAR-T cell therapy efficacy in solid tumors via NR2F6 deletion leading to revived T cell function and the induction of antigen-agnostic immune memory.
Article Title: NR2F6 deletion revives CAR-T cell function and induces antigen-agnostic immune memory in solid tumors.
Article References:
Humer, D., Klepsch, V., Rieder, D. et al. NR2F6 deletion revives CAR-T cell function and induces antigen-agnostic immune memory in solid tumors. Nat Commun (2026). https://doi.org/10.1038/s41467-026-69796-0
Image Credits: AI Generated
Tags: antigen-agnostic immune memoryboosting T cell persistence in cancerCAR-T therapy for solid tumorscellular immunotherapy advancementsenhancing CAR T cell efficacymolecular checkpoints in immunotherapynovel cancer immunotherapy mechanismsNR2F6 as immunotherapy targetNR2F6 deletion in CAR-T therapyovercoming solid tumor immunosuppressionreversing CAR-T cell exhaustiontumor microenvironment and CAR T cells