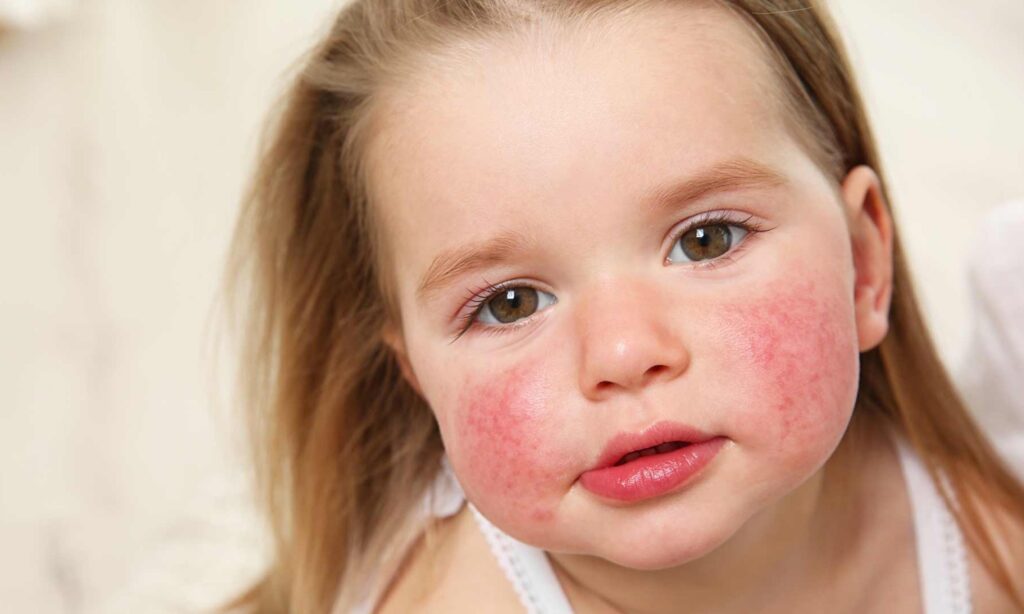
Skin immune cells in early life have been shown to mount a distinct, amplified reaction to common allergens that the same cells in adulthood do not.
That early burst of inflammation has now been linked to the timing of eczema and to the broader pattern of allergic disease that often follows it.
Working in that early-life window, Shruti Naik and colleagues at the Icahn School of Medicine documented how specific immune cells in young skin reacted with unusual intensity to those exposures.
That heightened response appeared only during a brief developmental period and faded as the animals matured.
The narrow timing of this reaction set the stage for understanding why eczema so often begins in infancy and why its origins cannot be explained by adult immune biology alone.
Dendritic cells overreact
One cell type stood out as the trigger: dendritic cells – immune sentries that activate other defense cells.
In newborn skin, these cells grabbed allergen bits and sent stronger chemical signals, so inflammation started quickly.
Adult skin carried the same cells, but their response stayed weaker after the same exposures in the same spot.
Only certain allergens triggered that response. This may explain why some children flare while others tolerate the same exposures.
Inflammation stays local
Rather than traveling deeper into the body, the early-life signal stayed in the skin and kept building.
Mapping the response, the study showed that some dendritic cells entered a peripheral immune inducer state, meaning they activated immunity on site.
Close-range activation pushed nearby cells to release inflammatory chemicals that damaged the outer skin layer.
Blocking that local pathway stopped baby mice from developing allergic skin inflammation, showing how early the process can begin.
Stress hormones and skin
Low levels of glucocorticoids, stress hormones that calm immune reactions, left newborn skin without strong control over inflammation.
During early development, the brain system that controls stress hormones had not fully matured, so baseline levels stayed low.
Giving infant mice a brief dose of corticosterone, a cortisol-like hormone in mice, dampened the overreaction within hours.
Because hormones rise with age, treatments that mimic adult levels might help, but they also carry real side effects.
Priming later allergies
For many families, eczema is more than a rash, since it can raise the odds of later allergies.
Researchers call that pattern the atopic march, when allergic disease moves from skin to airways over time.
Eczema affects nearly one in four children, and it often appears in the first months of life.
A skin flare in infancy also primed stronger lung inflammation in mice after a later allergen exposure.
Evidence from children
Skin samples from children with early eczema carried signs of the same overactive pathway seen in newborn mice.
In adult eczema samples, that signature faded, suggesting the child version of the disease may run on different rules.
Markers linked to the dendritic cell response appeared in early-onset cases, while adult skin more closely resembled the lower-response pattern seen in mature mice.
Human samples cannot prove cause on their own, but they make the mouse timeline harder to dismiss.
Time turned out to be the key factor, because the overreaction faded quickly as the newborn immune system matured.
By about 14 days after birth, mice no longer showed the same skin swelling after common allergen exposure.
Mold and a yeast trigger still sparked inflammation earlier, while several bacterial irritants failed to start that process.
Such selectivity hints that the young immune system followed a temporary set of rules, not a blanket weakness that hit every threat.
Early barrier disruption
Inflamed eczema skin often becomes dry and cracked, which lets more irritants and germs slip into the outer layers.
Once that barrier weakens, immune cells react again, and scratching can add more damage, keeping the flare going.
Early-life overreactions may start this cycle sooner, before families know which triggers to avoid or how to calm skin.
Even with good care, preventing the first immune flare could be easier than managing repeated flares once skin becomes sensitive.
Preventing early allergies
Next experiments will test ways to interrupt the early-life pathway, aiming to stop allergies before they spread beyond the skin.
Instead of treating flares after they start, future work may target the short window when immune controls are still developing.
“Children are not simply small adults when it comes to immunity,” said Naik, describing why pediatric allergy care cannot copy adult rules.
Any prevention plan will need careful testing in children, since damping inflammation too much can also weaken infection defense.
Mapping eczema origins
By tying early eczema risk to a brief immune overreaction and low stress hormones, the study gives childhood eczema a timeline.
Now, human trials must test whether guiding that window prevents later allergic disease without disrupting normal defense.
The study is published in Nature.
—–
Like what you read? Subscribe to our newsletter for engaging articles, exclusive content, and the latest updates.
Check us out on EarthSnap, a free app brought to you by Eric Ralls and Earth.com.
—–