The differences between men and women when it comes to disease are striking. For example, 50% of women will contract a urinary infection during their lifetime, compared with just 10 to 15% of men. Bladder cancer affects three times more men than women, but women with bladder cancer are often diagnosed at a later stage and have a worse prognosis. These disparities raise a basic question: why do immune responses and health trajectories differ depending on sex?
Molly Ingersoll’s team is seeking to elucidate this enigma by studying underexplored mucosal sites such as the bladder. The team’s theory is based on the influence of steroid hormones (estrogen, progesterone, androgens and cortisol), which act as powerful modulators of the immune system. To test their hypothesis, the scientists worked with the “Milieu Intérieur” consortium and analyzed 17 different hormones in the blood of the cohort volunteers, around 500 of whom came back to provide additional samples ten years later.
INSERER VIDEO MOLLY INGERSOLL
This longitudinal approach offers an insight into how our hormones change as we age. The results are striking.
Female hormonal contraception changes virtually the entire steroid landscape, including cortisol and cortisone, key regulators of stress and immunity. This systemic impact is as yet poorly understood, and it raises questions about long-term effects on metabolism and resistance to infection or other diseases.
The menopause is a critical turning point, with rapidly declining estrogen and progesterone levels associated with increased susceptibility to bladder infections and changes to the characteristics of bladder tumors.
In men who smoke, there was a surprising correlation between nicotine and androgens that was not found in women, revealing a link between specific levels of male hormones and environmental disruptors.
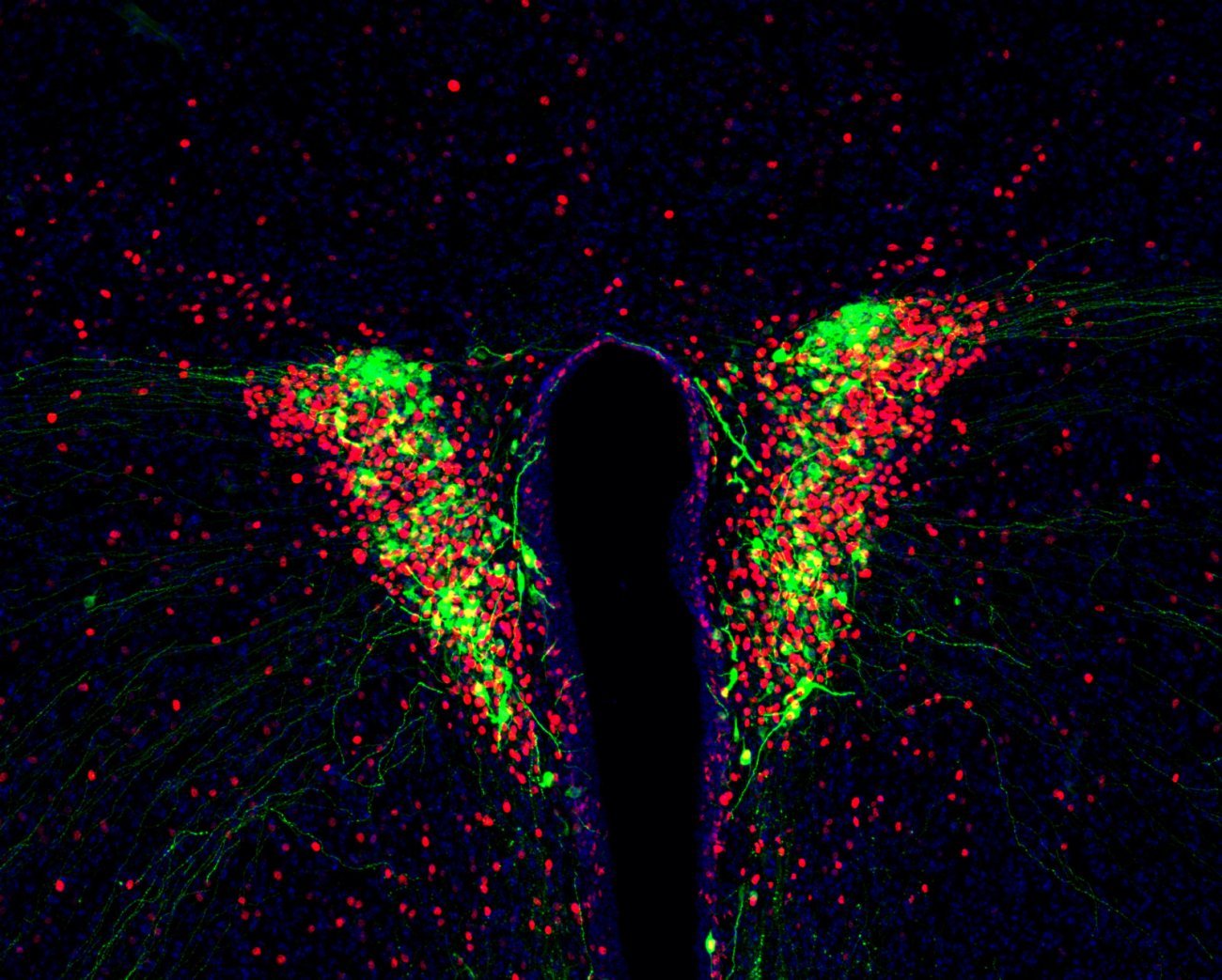
Hormone-producing neurons in the hypothalamus. In the hypothalamus, neurons producing vasopressin (green), a hormone essential for stress response and antidiuretic function, are activated by inflammation in the blood (c-Fos, red). – Copyright: Institut Pasteur/Ferdinand Jagot
Finally, monitoring the cohort over ten years showed that a significant drop in progestogens is unexpectedly linked with a higher risk of disease, but only in men.
The study has its limits – it can reveal correlations but not causality. But the quality of the data sets is unparalleled, providing scientists with rare and valuable insights.
The data will serve as a global benchmark. Future projects will focus on dissociating the effects of hormones from those of X/Y chromosomes and personalizing treatments based on sex. The challenge lies in adapting medicine to the biological reality of women and men, resulting in fairer, more effective therapies for everyone.