A small, but growing number of parents in the US are declining the routine vitamin K injection for their newborns.
Preliminary findings from a new review suggest that although the US refusal rate is still less than 1%, investigators report that it is trending upward in the US and globally.
“Vitamin K refusal, though uncommon, is rising and poses disproportionate neurologic risk, including intracranial hemorrhage, death, and long-term disability,” study investigator Beatriz De Faria Sousa, a medical student and researcher at Florida International University Herbert Wertheim College of Medicine, Miami, told Medscape Medical News.
The increasing rate of refusing the vitamin K shot appears to reflect broader healthcare hesitancy among parents, she added.
The study will be presented at the 2026 American Academy of Neurology (AAN) Annual Meeting in April.
A Vital Nutrient
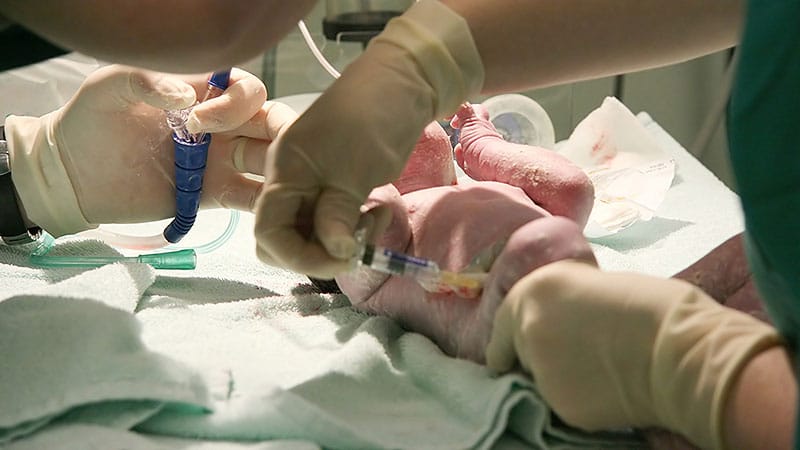
Vitamin K is a vital nutrient needed for normal blood clotting. Newborns are born with very low levels of the vitamin and receive only limited amounts through breast milk.
When a newborn has insufficient vitamin K, they may develop vitamin K deficiency bleeding (VKDB). Infants with VKDB can present with intracranial hemorrhage (ICH), which carries a significant risk for mortality and long-term neurologic disability, said De Faria Sousa.
Research shows that a single intramuscular (IM) injection of vitamin K at birth effectively protects against VKDB. The shot has been routinely administered since the American Academy of Pediatrics first recommended it in 1961, with other organizations — including the Canadian Paediatric Society — subsequently adopting similar guidance.
However, despite proven safety, the investigators noted that refusal of IM vitamin K is rising worldwide, paralleling vaccine hesitancy. The goal of the study was to review recent trends in vitamin K refusal and assess resulting neurologic consequences.
The analysis included 25 peer-reviewed studies identified through a systematic literature review covering 2005-2025. These comprised retrospective cohort studies, surveys, qualitative studies, case series, national surveillance reports, and reviews and were conducted in several countries, including the US, Canada, New Zealand, Australia, and Scotland.
Researchers extracted information on refusal prevalence and trends over time, VKDB incidence, ICH rates, mortality, neurologic outcomes, parental reasons for refusal,and possible links to vaccine refusal.
A Growing Global Trend
The results showed that refusal rates in the US remain low — below 1% in most hospitals — but pointed to upward trends in some states. In Minnesota, for example, the rate rose from 0.9% in 2015 to 1.6% in 2019. In California, Connecticut, and Iowa, refusal rates ranged from 0.2% to 1.3% in 2018-2019.
Internationally, refusal rates were higher, ranging from 1% to 3% in Canada, New Zealand, and Scotland.
Birthing centers and home birth settings had some of the highest refusal rates. In Tennessee, for example, refusal rates at birthing centers ranged from 28% to 31%.
Births attended by a midwife were also associated with higher refusal rates, as were parental beliefs aligned with “natural” philosophies. Such perspectives generally reflect a preference for reduced medical intervention during childbirth, said De Faria Sousa.
Several studies in the review also reported healthcare providers’ perceptions of vitamin K refusal rates. “Over half of providers perceive an increase,” said De Faria Sousa.
Evidence from the reviewed studies indicated that infants who did not receive IM vitamin K prophylaxis are 81 times more likely to develop VKDB. Among affected infants, about 63% present with ICH, 14% die, and 40% of survivors sustain neurologic disability.
Several studies in the review showed a strong association between vitamin K refusal and subsequent refusal of other newborn preventive services. For example, parents who declined vitamin K in Canada were 14.6 times more likely, and those in New Zealand 14.1 times more likely, to have a child who remained unimmunized at 15 months.
The investigators also found that in the US, those who refused IM Vitamin K were approximately 90 times more likely to refuse the hepatitis B vaccine and ocular prophylaxis for their infant.
Parents cited several reasons for refusal, including concerns about injection-related pain, preservatives in the formulation, and the perceived necessity of vitamin K, said De Faria Sousa. One persistent misconception is a purported link between vitamin K administration and leukemia.
Several reports noted increased use of oral vitamin K as an alternative to IM prophylaxis, with some clinicians recommending the oral formulation when parents declined the IM injection.
However, the data did not allow researchers to distinguish fear of injections from broader concerns about vitamin K itself as reasons for refusal, said De Faria Sousa. She added that countering the upward trend in vitamin K refusal will likely require prenatal counseling and targeted messaging.
“For neurologists, this trend signals growing burdens of avoidable developmental disorders. Universal uptake requires prenatal counseling, targeted messaging, and policy safeguards to reduce preventable neurodevelopmental disability,” the investigators noted in their abstract.
The study’s limitations included the fact that it was a review of previously published research and not a prospective study.
Addressing Parental Hesitancy
Reached for comment, Eugene Ng, MD, a neonatologist at Sunnybrook Health Sciences Centre in Toronto, Canada, who coauthored an updated position statement on vitamin K in newborns for the Canadian Paediatric Society, said he is not surprised that vitamin K refusal rates are increasing and said he has observed the trend in his own practice.
In some cases, Ng said he has been able to persuade parents who are hesitant about the IM injection to accept oral vitamin K instead. However, the oral regimen is less effective and requires multiple doses in addition to the initial dose given shortly after birth.
However, he added, some parents remain unconvinced about the importance of vitamin K, even when physicians explain the risk for ICH and its potentially severe consequences.
Ng said such refusals appear to reflect the broader environment of health misinformation and mistrust that has also affected attitudes toward childhood vaccinations. He also noted that the vitamin K injection is not a vaccine.
Such refusals, he added, can be frustrating for physicians, particularly given the potential consequences for the infant if vitamin K deficiency bleeding occurs. He noted that he and his colleagues have discussed whether refusal of vitamin K prophylaxis could, in some circumstances, raise child protection concerns.
At his institution, parents who decline the vitamin K injection are asked to sign a document acknowledging that the issue has been discussed with their provider and that they understand the potential risks to their infant and are declining the intervention against medical advice.
He added that more efforts are needed to disseminate accurate information about the vitamin K injection. This could include more effective use of social media and earlier prenatal education, including in prenatal classes.