One of the most advanced cancer treatments available today may soon get a major upgrade. CAR-T therapy has already saved lives, but it remains complex, expensive, and difficult to access.
Now, researchers at the University of California, San Francisco (UCSF) have developed a new approach that could bypass many of those challenges.
The technology works by reprogramming immune cells directly inside the body, opening the door to faster, simpler cancer treatment delivered with a single injection.
This method could remove the long waiting time and high costs linked to current CAR-T cell therapy. It may also make treatment available to more patients around the world.
Reprogramming immune cells to fight cancer
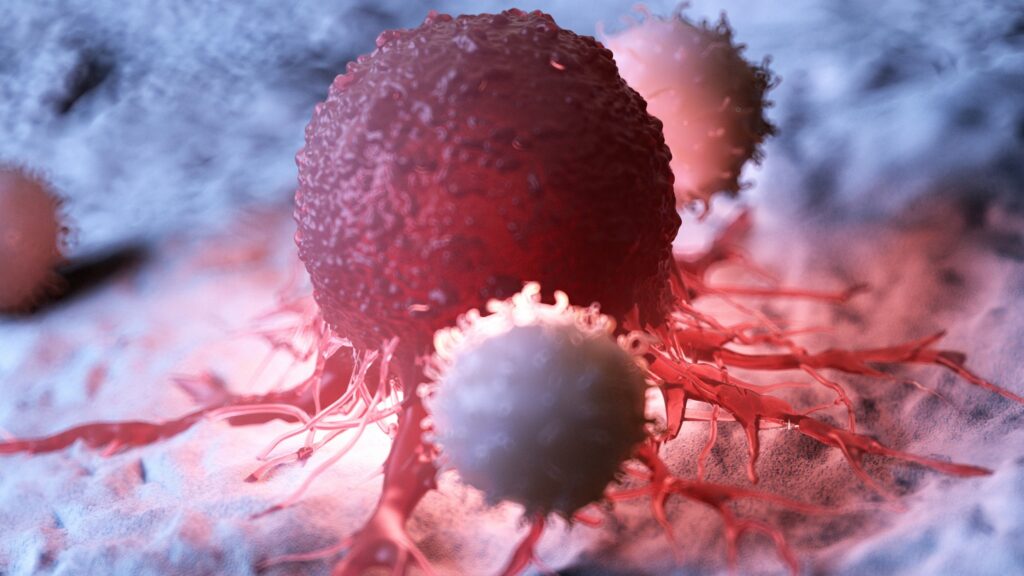
CAR-T cell therapy uses the body’s own immune system to fight cancer. Doctors collect T cells and give them new instructions in a lab.
These instructions help the cells recognize and attack cancer. The added structure, called a CAR, works like an antenna that detects cancer cells.
This therapy has already changed cancer treatment. The U.S. Food and Drug Administration has approved several CAR-T therapies for blood cancers.
Scientists are also exploring its use for infections and autoimmune diseases. However, the current process is slow and expensive, which limits access.
Challenges of CAR-T therapy
The standard method requires removing cells, modifying them, and sending them back to the patient. This process takes weeks and costs a lot of money. Not every hospital can provide this treatment.
Another issue is how the new genes are added. Traditional methods use viruses that insert DNA randomly. This can lead to uneven results because not all cells behave the same way. Some cells may work well, while others may not.
“It’s become a global access issue; many patients who would benefit from CAR-T cells either can’t afford them or can’t get them fast enough,” said Dr. Justin Eyquem, a corresponding author of the study and a UCSF professor of medicine.
“There has been a big push in the field to try to move to directly producing these cells in the body.”
Editing immune cells inside the body
Scientists at UCSF, along with the Gladstone Institutes, Duke University, and Innovative Genomics Institute, created a new solution. This method edits T cells directly inside the body, which is called in vivo engineering.
The system uses two delivery tools. One carries CRISPR-Cas9, a gene-editing tool that works like molecular scissors. The second carries the new DNA needed to create cancer-fighting cells.
This new DNA is placed at a specific location in the T cell genome called the TRAC site. This site acts like a natural control switch that turns on the CAR only in T cells, making the process more accurate and safer than random insertion.
Injection improves cancer targeting
Placing the CAR gene in the correct location makes a big difference. Every edited T cell produces the CAR in a controlled and consistent way. This helps the cells work better and last longer in the body.
Random insertion, used in older methods, can lead to uneven CAR levels. Some cells may not produce enough CAR to fight cancer effectively. The new method avoids this issue by using precise gene placement.
“When you manufacture these cells outside the body, you can do a lot of quality control to make sure you only end up with re-engineered T cells,” said Dr. Eyquem.
“Inside the body, we can’t do that post-manufacturing quality control, so we really needed to optimize the approach upfront to avoid altering any other cells.”
Strong cancer control in early studies
Scientists tested this method in mice with human-like immune systems. A single treatment produced strong results. Many mice showed complete removal of cancer within a short time.
In one study, most mice with aggressive leukemia showed full recovery after one injection.
The modified T cells grew quickly and spread through the body. In some cases, up to 40 percent of immune cells became cancer-fighting cells.
The method also worked for multiple myeloma and even solid tumors. Solid tumors are usually harder to treat, so this result is very important.
Injection boosts cancer response
The study also showed that these cells expand quickly after treatment. The immune response started earlier and became stronger compared to older methods.
In some cases, the number of cancer-fighting cells increased many times faster than with traditional approaches.
Another key finding is that these cells can remember cancer. When scientists reintroduced cancer in treated mice, the immune system responded again and controlled it, showing long-term protection.
“What was especially remarkable was that the cells we’re generating in vivo actually look better than what we make in the lab,” Dr. Eyquem said.
“We think that when cells are taken out of the body and grown in the lab, they lose some of their ‘stemness’ and proliferative capacity, and that doesn’t happen here.”
Safer and more accessible CAR-T
The researchers improved how the therapy reaches T cells, targeting only these cells while avoiding others. This precision reduces the risk of unwanted genetic changes.
They also designed carriers that resist attacks from the immune system, helping the therapy work more effectively inside the body. Early tests showed no major harmful immune reactions.
Beyond safety, the approach could simplify treatment by removing the need for complex lab procedures. This may lower costs, speed up care, and allow smaller hospitals – not just major cancer centers – to offer CAR-T therapy.
“I think this is just the beginning of a big wave of new therapies that will be truly transformational and save a lot of lives,” said Dr. Eyquem.
“If we can translate this to humans, we could dramatically reduce costs, eliminate waiting times, and potentially allow community hospitals – not just major cancer centers – to offer these life-saving therapies,” he said. “That would truly democratize access to CAR-T cell therapy.”
Together, the findings point to a future where a single injection could help the body fight cancer on its own.
The study is published in the journal Nature.
—–
Like what you read? Subscribe to our newsletter for engaging articles, exclusive content, and the latest updates.
Check us out on EarthSnap, a free app brought to you by Eric Ralls and Earth.com.
—–