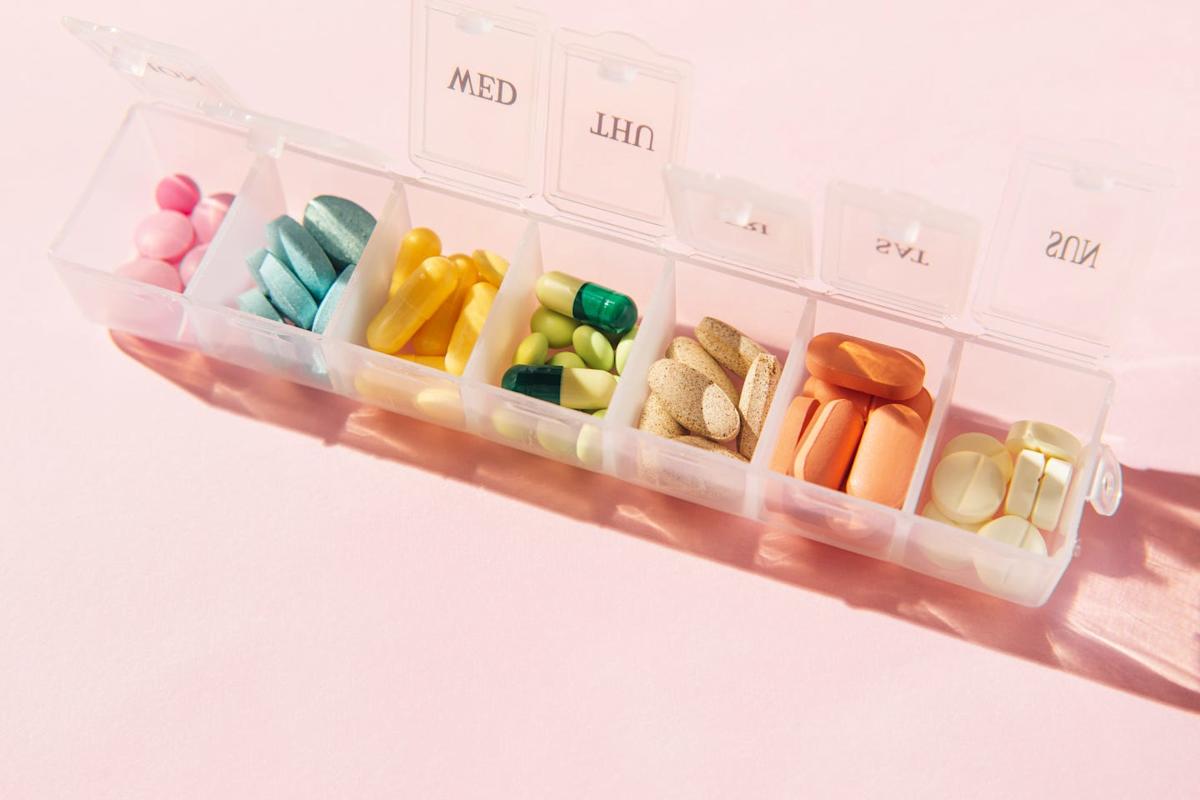
Can Supplements Help With Perimenopause?Tanja Ivanova – Getty Images
Perimenopause supplements are everywhere. Scroll social media for a few minutes, and you’ll see powders promising “hormone balance,” capsules for hot flashes, collagen drinks for skin elasticity, herbal blends for mood swings, and metabolism-boosting gummies aimed at women in midlife.
It’s easy to see the appeal. Perimenopause—the often years-long transition before menopause that typically begins in a woman’s 40s, though sometimes earlier—occurs as ovarian function begins to decline, leading to unpredictable hormone fluctuations. Periods may change or disappear, and symptoms like hot flashes, night sweats, poor sleep, mood swings, brain fog, joint pain, weight shifts, low libido, and fatigue can come and go. Many of these symptoms overlap with menopause, though they often start gradually and fluctuate more unpredictably during perimenopause.
Because many of these changes also coincide with stress or normal aging, women are often told it’s “just getting older.” In that space of confusion and dismissal, supplements can feel like taking control: accessible, over the counter, and marketed as empowering solutions for an unpredictable body. But how much do they actually help?
Sharon Malone, M.D., a board-certified OB/GYN, certified menopause practitioner, and author of Grown Woman Talk, says hormone replacement therapy remains the most reliable way to relieve symptoms during this transition. Hormone replacement therapy (HRT), a treatment that helps replace hormones like estrogen as they decline, may also help some women in perimenopause. However, supplements can be an alternative for those who can’t use hormone therapy due to medical history or who prefer a non-hormonal option.
So can supplements meaningfully help with perimenopause symptoms? We asked OB/GYNs and women’s health-focused registered dietitians to weigh in.
Can vitamins actually help with perimenopause?
Vitamins don’t treat perimenopause itself—they can’t stop ovarian aging or restore estrogen—but they may support specific systems affected during this transition.
Jennifer Laurence, MA, RD, a registered dietitian specializing in midlife and menopause, shares similar insights about marketing outpacing the science. “One concern is that certain dietary supplements for perimenopause either lack the research required to support their effectiveness, or the research is inconclusive. However, these are still marketed to the public,” she says.
Laurence also notes that influencers and celebrities often help amplify these products, which can be especially problematic. “Women are often overwhelmed and confused during perimenopause, which can make them vulnerable in their search for a solution,” she says.
In other words, supplements are tools. They are not hormone therapy, and they are not a substitute for medical care. Jessica Corwin, MPH, RDN, NBC-HWC, a registered dietitian who specializes in midlife nutrition, adds, “One of the biggest myths I spend time correcting is the idea that a supplement alone will solve perimenopause. If sleep, stress, meal timing, circadian rhythm, eating enough, and recovery are all off, no supplement can fully compensate.” She wants women to understand that supplements cannot replace hormone therapy or other evidence-based treatments for moderate to severe hot flashes or night sweats, and they are not immediate fixes.

Getty Images
Key nutrients that may help
Perimenopause brings a lot of changes—hormones shift, energy can dip, sleep might suffer, and you may notice changes in mood, muscle, or bone strength. Certain nutrients can help your body navigate this transition:
Calcium and vitamin D are crucial for keeping bones strong, and vitamin K2 helps your body use that calcium more effectively as estrogen levels decline.
Omega-3s are important, too; they support heart and brain health and may help ease mild inflammation that can manifest as joint stiffness or discomfort.
Magnesium can make a noticeable difference for sleep and mood, while B vitamins help keep your energy levels consistent.
Protein is key for maintaining muscle and metabolism, which naturally slows during this stage, and fiber helps manage blood sugar, supports digestion, and even assists hormone balance.
Vitamin C helps your skin, blood vessels, and immune system by supporting collagen and acting as an antioxidant.
Some women also find that phytoestrogens from foods like soy can help modestly with mild hormone-related symptoms such as hot flashes.
While supplements can be useful if you’re not meeting your needs through food, focusing on whole, nutrient-rich foods like leafy greens, fatty fish, dairy or fortified alternatives, nuts, seeds, legumes, and whole grains gives your body the combination of nutrients it can absorb and use most effectively.
Are perimenopause supplements safe?
Many perimenopause-branded supplement blends promise hormone balance, but evidence supporting these claims is often limited. Experts emphasize that supplements are not risk-free and should be used thoughtfully.
Dr. Sameena Rahman, OB/GYN, menopause specialist, and founder of GSM Collective, cautions that “natural” doesn’t automatically mean safe. Supplements can carry real risks and are most helpful when correcting a true deficiency, she says. Taking supplements without medical guidance—especially at high doses—can backfire. For individuals with a history of kidney stones, high-dose calcium supplements—especially when not taken with meals—may increase the risk of recurrence, and high doses of vitamin E have been linked to a higher risk of hemorrhagic stroke.
Rahman also notes that some popular ingredients—like turmeric and red yeast rice—may affect liver function. Biotin can also interfere with lab tests, including thyroid and cardiac markers, potentially leading to misdiagnosis. Corwin adds that untested supplements may contain contaminants or incorrect doses, and certain ingredients—such as maca, B-complex formulas, or ashwagandha—can overstimulate the nervous system or worsen histamine-related symptoms in sensitive individuals. Jerlyn Jones, RD, who specializes in perimenopause and menopause, further notes that ashwagandha may interact with thyroid medications.
High-dose minerals also warrant caution, especially for women with underlying conditions or those already meeting their needs through diet. Sayuri Barritt, RD, CD, a registered dietitian who supports women in midlife, adds that supplements tend to work gradually; hormonal balance and symptom relief often take time rather than happening immediately. Even simple supplements can have complex effects, and lasting improvements typically require a combination of lifestyle changes, nutrition, and medical guidance—not just pills.
Should you get tested first?
Before starting supplements, bloodwork can help identify nutrient deficiencies, such as vitamin D, iron, or B12, which are most likely to respond meaningfully to supplementation. Corwin says supplements usually offer modest improvements rather than complete symptom relief, with the greatest benefits seen when a true deficiency is corrected. Ultimately, decisions about supplementation should consider medical history, current medications, and symptom patterns.
The bigger picture
Supporting health during perimenopause and menopause is most effective with balanced nutrition, strength training, quality sleep, stress management, and regular medical care. As Barritt explains, macro- and micronutrients are best obtained from whole foods, which the body is designed to digest and absorb through complex processes. Whole foods also deliver nutrients in combinations that supplements can’t replicate, and individual symptoms may shift nutrient needs. If using supplements, Jones recommends choosing reputable, third-party–tested brands, such as those certified by USP, NSF International, or Informed Choice, to ensure safety and quality.
Perimenopause varies widely from person to person, but it can be managed. Rahman notes that many women normalize discomfort or delay seeking care, even when symptoms may reflect broader health concerns. While supplements can offer targeted support—for muscle, bone, blood sugar, and digestion—they’re not a cure-all. The most effective approach pairs consistent lifestyle habits with thoughtful supplement use and realistic expectations.
“Perimenopause is an opportunity for prevention and early intervention, not something women should simply ‘push through,’” says Rahman.
Why trust Good Housekeeping?
Valerie Agyeman is a registered dietitian specializing in women’s health with over 10 years of experience in clinical nutrition, corporate wellness, and nutrition communications. She contributes to food and supplement testing at the Good Housekeeping Institute Nutrition & Fitness Lab and has covered topics including gut health, vitamin D, and skin health.
Stefani Sassos is the director of the Good Housekeeping Institute Nutrition Lab where she oversees all nutrition-related content, product testing, and evaluation. She runs and oversees supplement testing and analysis for Good Housekeeping and has covered other supplements in the past including multivitamins, vitamin D, and joint supplements.
For this piece, we consulted experts in women’s health to provide trusted, practical guidance:
Dr. Sameena Rahman is a board-certified OB/GYN and certified Menopause Practitioner with over a decade of experience in midlife care, sexual medicine, and concierge gynecology. She founded The GSM Collective in Chicago to provide personalized, patient-first women’s healthcare and serves as Clinical Assistant Professor of OB/GYN at Northwestern Feinberg School of Medicine.
Jessica Corwin is a registered dietitian nutritionist, a National Board Certified Health and Wellness Coach, and holds a Master’s in Public Health, with 20 years of experience spanning community health, culinary nutrition, and lifestyle medicine. She specializes in midlife nutrition, translating evidence-based research into practical guidance for women navigating perimenopause and menopause through her practice, Eat. Grow. Live.
Jennifer Laurence is a registered dietitian and licensed nutritionist with a master’s in Nutrition Education, specializing in integrative and functional medical nutrition therapy for women in midlife. She helps women navigate unwanted weight gain, fatigue, and other metabolic changes during perimenopause and menopause through personalized, sustainable nutrition and lifestyle strategies.
Jerlyn Jones is a registered dietitian, nutrition consultant, and owner of The Lifestyle Dietitian LLC, specializing in perimenopause and menopause. She brings extensive experience helping individuals manage symptoms such as bloating, fatigue, and digestive changes through evidence-based, practical nutrition strategies.
Sayuri Barritt, RD, CD, is the owner of Forty Love Nutrition LLC in Seattle, WA, specializing in supporting women in midlife to improve metabolic health, hormone balance, and gut function. She helps clients transform body insecurities into strength and energy through evidence-based nutrition education and personalized counseling.
You Might Also Like