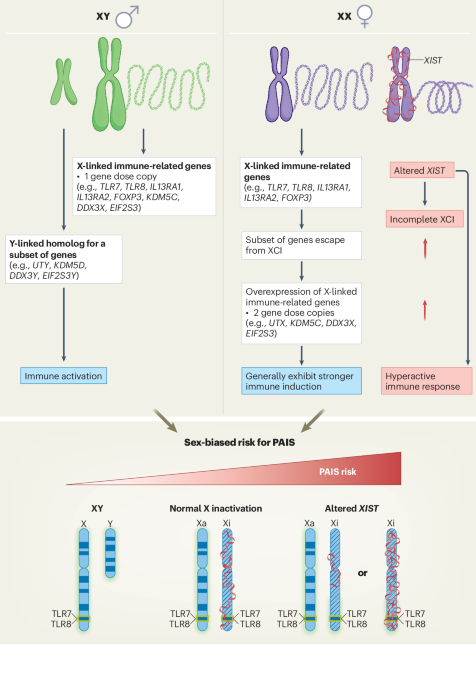
Fish, E. N. The X-files in immunity: sex-based differences predispose immune responses. Nat. Rev. Immunol. 8, 737–744 (2008). This review compiles a comprehensive table of immune-related genes on the X chromosome and synthesizes evidence from the literature showing that some of these genes escape XCI, resulting in increaed gene dosage.
Cheng, M. I. et al. The X-linked epigenetic regulator UTX controls NK cell-intrinsic sex differences. Nat. Immunol. 24, 780–791 (2023).
Cunningham, M. A., Wirth, J. R., Naga, O., Eudaly, J. & Gilkeson, G. S. Estrogen receptor α binding to ERE is required for full Tlr7- and Tlr9-induced inflammation. SOJ Immunol 2, 7 (2014).
Klein, S. L. & Flanagan, K. L. Sex differences in immune responses. Nat. Rev. Immunol. 16, 626–638 (2016). This seminal paper is often credited with defining the field of sex differences in immunity. The review examines immune responses across a range of diseases and presents evidence for the the evolutionary emergence of sex-based differences in immunity across species.
Dunn, S. E., Perry, W. A. & Klein, S. L. Mechanisms and consequences of sex differences in immune responses. Nat. Rev. Nephrol. 20, 37–55 (2024).
Libert, C., Dejager, L. & Pinheiro, I. The X chromosome in immune functions: when a chromosome makes the difference. Nat. Rev. Immunol. 10, 594–604 (2010).
Case, L. K. et al. Chromosome y regulates survival following murine coxsackievirus b3 infection. G3 2, 115–121 (2012).
Arnold, A. P. X chromosome agents of sexual differentiation. Nat. Rev. Endocrinol. 18, 574–583 (2022).
Berletch, J. B. et al. Escape from X inactivation varies in mouse tissues. PLoS Genet. 11, e1005079 (2015).
Carrel, L. & Willard, H. F. X-inactivation profile reveals extensive variability in X-linked gene expression in females. Nature 434, 400–404 (2005).
Arnold, A. P. Four core genotypes and XY* mouse models: Update on impact on SABV research. Neurosci. Biobehav. Rev. 119, 1–8 (2020).
Itoh, Y. et al. The X-linked histone demethylase Kdm6a in CD4+ T lymphocytes modulates autoimmunity. J. Clin. Invest. 129, 3852–3863 (2019). This paper clearly demonstrates how X-chromosome gene dosage influences immune cell function and shapes disease outcomes.
Hagen, S. H. et al. Heterogeneous escape from X chromosome inactivation results in sex differences in type I IFN responses at the single human pDC level. Cell Rep. 33, 108485 (2020).
Rubtsov, A. V. et al. Toll-like receptor 7 (TLR7)-driven accumulation of a novel CD11c+ B-cell population is important for the development of autoimmunity. Blood 118, 1305–1315 (2011).
Blanton, L. V. et al. Stable and robust Xi and Y transcriptomes drive cell-type-specific autosomal and Xa responses in vivo and in vitro in four human cell types. Cell Genom. 4, 100628 (2024).
Dutta, S. & Sengupta, P. Men and mice: relating their ages. Life Sci. 152, 244–248 (2016).
Potluri, T. et al. Age-associated changes in the impact of sex steroids on influenza vaccine responses in males and females. NPJ Vaccines 4, 29 (2019).
Fox, H. S., Bond, B. L. & Parslow, T. G. Estrogen regulates the IFN-γ promoter. J. Immunol. 146, 4362–4367 (1991).
Heldring, N. et al. Estrogen receptors: how do they signal and what are their targets. Physiol. Rev. 87, 905–931 (2007).
Kovats, S. Estrogen receptors regulate innate immune cells and signaling pathways. Cell. Immunol. 294, 63–69 (2015).
Hoffmann, J. P., Liu, J. A., Seddu, K. & Klein, S. L. Sex hormone signaling and regulation of immune function. Immunity 56, 2472–2491 (2023).
Thiebaut, C., Vlaeminck-Guillem, V., Trédan, O., Poulard, C. & Le Romancer, M. Non-genomic signaling of steroid receptors in cancer. Mol. Cell. Endocrinol. 538, 111453 (2021).
Lei, K. et al. Progesterone acts via the nuclear glucocorticoid receptor to suppress IL-1β-induced COX-2 expression in human term myometrial cells. PLoS ONE 7, e50167 (2012).
Merlino, A. A. et al. Nuclear progesterone receptors in the human pregnancy myometrium: evidence that parturition involves functional progesterone withdrawal mediated by increased expression of progesterone receptor-A. J. Clin. Endocrinol. Metab. 92, 1927–1933 (2007).
Su, L. et al. Progesterone inhibits Toll-like receptor 4-mediated innate immune response in macrophages by suppressing NF-κB activation and enhancing SOCS1 expression. Immunol. Lett. 125, 151–155 (2009).
Creisher, P. S. & Klein, S. L. Pathogenesis of viral infections during pregnancy. Clin. Microbiol. Rev. 37, e0007323 (2024).
Berghofer, B. et al. TLR7 ligands induce higher IFN-α production in females. J. Immunol. 177, 2088–2096 (2006).
Meier, A. et al. Sex differences in the Toll-like receptor-mediated response of plasmacytoid dendritic cells to HIV-1. Nat. Med. 15, 955–959 (2009). This study shows sex-differential innate immune sensing of HIV-1 by pDCs, with cells from female individuals producing more IFNα in response to HIV-1-derived TLR7/TLR8 ligands than cells from male individuals, providing insights into how female individuals have a stronger overall immune response during infection.
Ziegler, S. M. et al. Human pDCs display sex-specific differences in type I interferon subtypes and interferon α/β receptor expression. Eur. J. Immunol. 47, 251–256 (2017).
Seillet, C. et al. The TLR-mediated response of plasmacytoid dendritic cells is positively regulated by estradiol in vivo through cell-intrinsic estrogen receptor alpha signaling. Blood 119, 454–464 (2012).
Wang, J. P., Zhang, L., Madera, R. F., Woda, M. & Libraty, D. H. Plasmacytoid dendritic cell interferon-α production to R-848 stimulation is decreased in male infants. BMC Immunol. 13, 35 (2012).
Webb, K. et al. Sex and pubertal differences in the type 1 interferon pathway associate with both X chromosome number and serum sex hormone concentration. Front. Immunol. 9, 3167 (2018).
Griesbeck, M. et al. Sex differences in plasmacytoid dendritic cell levels of IRF5 drive higher IFN-α production in women. J. Immunol. 195, 5327–5336 (2015).
Laffont, S. et al. X-Chromosome complement and estrogen receptor signaling independently contribute to the enhanced TLR7-mediated IFN-alpha production of plasmacytoid dendritic cells from women. J. Immunol. 193, 5444–5452 (2014).
Souyris, M. et al. TLR7 escapes X chromosome inactivation in immune cells. Sci. Immunol. 3, eaap8855 (2018). This study shows that TLR7 escapes XCI in B cells and myeloid cells from XX female individuals and individuals with Klinefelter syndrome.
Grunhagel, B. et al. Reduction of IFN-I responses by plasmacytoid dendritic cells in a longitudinal trans men cohort. iScience 26, 108209 (2023).
Lakshmikanth, T. et al. Immune system adaptation during gender-affirming testosterone treatment. Nature 633, 155–164 (2024).
Scotland, R. S., Stables, M. J., Madalli, S., Watson, P. & Gilroy, D. W. Sex differences in resident immune cell phenotype underlie more efficient acute inflammatory responses in female mice. Blood 118, 5918–5927 (2011).
Jabeen, S. et al. TLR4 sex dimorphism correlates with sex dimorphic phagocytosis in primary macrophages. J. Gend. Specif. Med. 6, 100–106 (2020).
Ter Horst, R. et al. Host and environmental factors influencing individual human cytokine responses. Cell 167, 1111–1124 (2016).
De Maeyer, R. P. H. et al. Age-associated inflammatory monocytes are increased in menopausal females and reversed by hormone replacement therapy. Aging Cell 24, e70249 (2025).
Di Florio, D. N., Sin, J., Coronado, M. J., Atwal, P. S. & Fairweather, D. Sex differences in inflammation, redox biology, mitochondria and autoimmunity. Redox Biol. 31, 101482 (2020).
Alves, T. et al. Inflammasome targeting for periodontitis prevention is sex dependent. Proc. Natl Acad. Sci. USA 122, e2507092122 (2025).
Huang, Z. et al. Effects of sex and aging on the immune cell landscape as assessed by single-cell transcriptomic analysis. Proc. Natl Acad. Sci. USA 118, e2023216118 (2021).
Zhang, M. A. et al. Antagonizing peroxisome proliferator-activated receptor alpha activity selectively enhances TH1 immunity in male mice. J. Immunol. 195, 5189–5202 (2015).
Blanquart, E., Laffont, S. & Guery, J. C. Sex hormone regulation of innate lymphoid cells. Biomed. J. 44, 144–156 (2021).
Zychlinsky Scharff, A. et al. Sex differences in IL-17 contribute to chronicity in male versus female urinary tract infection. JCI Insight 5, e122998 (2019).
Darboe, A. et al. Age-related dynamics of circulating innate lymphoid cells in an African population. Front. Immunol. 11, 594107 (2020).
Kadel, S. et al. A major population of functional KLRG1− ILC2s in female lungs contributes to a sex bias in ILC2 numbers. Immunohorizons 2, 74–86 (2018).
Cephus, J. Y. et al. Testosterone attenuates group 2 innate lymphoid cell-mediated airway inflammation. Cell Rep. 21, 2487–2499 (2017).
Laffont, S. et al. Androgen signaling negatively controls group 2 innate lymphoid cells. J. Exp. Med. 214, 1581–1592 (2017).
Chi, L. et al. Sexual dimorphism in skin immunity is mediated by an androgen-ILC2-dendritic cell axis. Science 384, eadk6200 (2024).
Vom Steeg, L. G., Flores-Garcia, Y., Zavala, F. & Klein, S. L. Irradiated sporozoite vaccination induces sex-specific immune responses and protection against malaria in mice. Vaccine 37, 4468–4476 (2019).
Peacock, J. W. et al. Gender differences in human immunodeficiency virus type 1-specific CD8 responses in the reproductive tract and colon following nasal peptide priming and modified vaccinia virus Ankara boosting. J. Virol. 78, 13163–13172 (2004).
Amadori, A. et al. Genetic control of the CD4/CD8 T-cell ratio in humans. Nat. Med. 1, 1279–1283 (1995).
Breznik, J. A., Schulz, C., Ma, J., Sloboda, D. M. & Bowdish, D. M. E. Biological sex, not reproductive cycle, influences peripheral blood immune cell prevalence in mice. J. Physiol. 599, 2169–2195 (2021).
Gui, J., Mustachio, L. M., Su, D. M. & Craig, R. W. Thymus size and age-related thymic involution: early programming, sexual dimorphism, progenitors and stroma. Aging Dis. 3, 280–290 (2012).
Olsen, N. J., Olson, G., Viselli, S. M., Gu, X. & Kovacs, W. J. Androgen receptors in thymic epithelium modulate thymus size and thymocyte development. Endocrinology 142, 1278–1283 (2001).
Cua, D. J., Hinton, D. R. & Stohlman, S. A. Self-antigen-induced Th2 responses in experimental allergic encephalomyelitis (EAE)-resistant mice. Th2-mediated suppression of autoimmune disease. J. Immunol. 155, 4052–4059 (1995).
Dunn, S. E. et al. Peroxisome proliferator-activated receptor (PPAR)α expression in T cells mediates gender differences in development of T cell-mediated autoimmunity. J. Exp. Med. 204, 321–330 (2007).
Zhang, M. A. et al. Peroxisome proliferator-activated receptor (PPAR)α and -γ regulate IFNγ and IL-17A production by human T cells in a sex-specific way. Proc. Natl Acad. Sci. USA 109, 9505–9510 (2012).
Hewagama, A., Patel, D., Yarlagadda, S., Strickland, F. M. & Richardson, B. C. Stronger inflammatory/cytotoxic T-cell response in women identified by microarray analysis. Genes Immun. 10, 509–516 (2009).
Crotty, S. T. Follicular helper cell biology: a decade of discovery and diseases. Immunity 50, 1132–1148 (2019).
Park, H. J., Park, H. S., Lee, J. U., Bothwell, A. L. & Choi, J. M. Gender-specific differences in PPARγ regulation of follicular helper T cell responses with estrogen. Sci. Rep. 6, 28495 (2016).
Kim, S. J., Zou, Y. R., Goldstein, J., Reizis, B. & Diamond, B. Tolerogenic function of Blimp-1 in dendritic cells. J. Exp. Med. 208, 2193–2199 (2011).
Vignali, D. A., Collison, L. W. & Workman, C. J. How regulatory T cells work. Nat. Rev. Immunol. 8, 523–532 (2008).
Robinson, G. A. et al. Investigating sex differences in T regulatory cells from cisgender and transgender healthy individuals and patients with autoimmune inflammatory disease: a cross-sectional study. Lancet Rheumatol. 4, e710–e724 (2022).
Afshan, G., Afzal, N. & Qureshi, S. CD4+CD25hi regulatory T cells in healthy males and females mediate gender difference in the prevalence of autoimmune diseases. Clin. Lab. 58, 567–571 (2012).
Kondo, H. et al. Markers of memory CD8 T cells depicting the effect of the BNT162b2 mRNA COVID-19 vaccine in Japan. Front. Immunol. 13, 836923 (2022).
Yee Mon, K. J. et al. Differential sensitivity to IL-12 drives sex-specific differences in the CD8+ T cell response to infection. Immunohorizons 3, 121–132 (2019).
Rukavina, D. et al. Age-related decline of perforin expression in human cytotoxic T lymphocytes and natural killer cells. Blood 92, 2410–2420 (1998).
Guan, X. et al. Androgen receptor activity in T cells limits checkpoint blockade efficacy. Nature 606, 791–796 (2022).
Yang, C. et al. Androgen receptor-mediated CD8+ T cell stemness programs drive sex differences in antitumor immunity. Immunity 55, 1268–1283 (2022).
Kwon, H. et al. Androgen conspires with the CD8+ T cell exhaustion program and contributes to sex bias in cancer. Sci. Immunol. 7, eabq2630 (2022).
Surman, S. L. et al. How estrogen, testosterone, and sex differences influence serum immunoglobulin isotype patterns in mice and humans. Viruses 15, 482 (2023).
Peckham, H. et al. Estrogen influences class-switched memory B cell frequency only in humans with two X chromosomes. J. Exp. Med. 222, e20241253 (2025).
Fink, A. L. & Klein, S. L. The evolution of greater humoral immunity in females than males: implications for vaccine efficacy. Curr. Opin. Physiol. 6, 16–20 (2018).
Flanagan, K. L., Fink, A. L., Plebanski, M. & Klein, S. L. Sex and gender differences in the outcomes of vaccination over the life course. Annu. Rev. Cell Dev. Biol. 33, 577–599 (2017).
Mohanram, V. et al. B cell responses associated with vaccine-induced delayed SIVmac251 acquisition in female rhesus macaques. J. Immunol. 197, 2316–2324 (2016).
Tuero, I. et al. Mucosal B cells are associated with delayed SIV acquisition in vaccinated female but not male rhesus macaques following SIVmac251 rectal challenge. PLoS Pathog. 11, e1005101 (2015).
Fink, A. L., Engle, K., Ursin, R. L., Tang, W. Y. & Klein, S. L. Biological sex affects vaccine efficacy and protection against influenza in mice. Proc. Natl Acad. Sci. USA 115, 12477–12482 (2018).
Farzadegan, H. et al. Sex differences in HIV-1 viral load and progression to AIDS. Lancet 352, 1510–1514 (1998). This study is among the first to provide large-scale clinical evidence that female individuals have lower HIV-1 viral loads than male individuals at comparable stages of infection, yet experience faster progression to AIDS.
Scully, E. P. et al. Sex-based differences in human immunodeficiency virus type 1 reservoir activity and residual immune activation. J. Infect. Dis. 219, 1084–1094 (2019).
Das, B. et al. Estrogen receptor-1 is a key regulator of HIV-1 latency that imparts gender-specific restrictions on the latent reservoir. Proc. Natl Acad. Sci. USA 115, E7795–E7804 (2018).
Rubin, L. H. et al. Sex differences in neurocognitive function in adults with HIV: patterns, predictors, and mechanisms. Curr. Psychiatry Rep. 21, 94 (2019).
Szotek, E. L., Narasipura, S. D. & Al-Harthi, L. 17β-estradiol inhibits HIV-1 by inducing a complex formation between β-catenin and estrogen receptor α on the HIV promoter to suppress HIV transcription. Virology 443, 375–383 (2013).
Chang, J. J. et al. Higher expression of several interferon-stimulated genes in HIV-1-infected females after adjusting for the level of viral replication. J. Infect. Dis. 208, 830–838 (2013).
Ziegler, S. & Altfeld, M. Sex differences in HIV-1-mediated immunopathology. Curr. Opin. HIV AIDS 11, 209–215 (2016).
Prodger, J. L. et al. Reduced HIV-1 latent reservoir outgrowth and distinct immune correlates among women in Rakai, Uganda. JCI Insight 5, e139287 (2020).
Yu, M. W. et al. Androgen-receptor gene CAG repeats, plasma testosterone levels, and risk of hepatitis B-related hepatocellular carcinoma. J. Natl Cancer Inst. 92, 2023–2028 (2000).
Brown, R., Goulder, P. & Matthews, P. C. Sexual Dimorphism in chronic hepatitis B virus (HBV) infection: evidence to inform elimination efforts. Wellcome Open Res. 7, 32 (2022).
Ruggieri, A., Gagliardi, M. C. & Anticoli, S. Sex-Dependent outcome of hepatitis B and C viruses infections: synergy of sex hormones and immune responses? Front. Immunol. 9, 2302 (2018).
Chan, W. K., Klock, G. & Bernard, H. U. Progesterone and glucocorticoid response elements occur in the long control regions of several human papillomaviruses involved in anogenital neoplasia. J. Virol. 63, 3261–3269 (1989).
Grebely, J. et al. The effects of female sex, viral genotype, and IL28B genotype on spontaneous clearance of acute hepatitis C virus infection. Hepatology 59, 109–120 (2014).
Breidbart, S., Burk, R. D. & Saenger, P. Hormonal regulation of hepatitis B virus gene expression: influence of androgen receptor. Pediat. Res. 34, 300–302 (1993).
Farza, H. et al. Hepatitis B surface antigen gene expression is regulated by sex steroids and glucocorticoids in transgenic mice. Proc. Natl Acad. Sci. USA 84, 1187–1191 (1987).
Tsay, P. K. et al. Impact of gender, viral transmission and aging in the prevalence of hepatitis B surface antigen. Chang Gung Med. J. 32, 155–164 (2009).
Wang, S. H. et al. Estrogen receptor α represses transcription of HBV genes via interaction with hepatocyte nuclear factor 4α. Gastroenterology 142, 989–998 (2012).
Wu, M. H. et al. Androgen receptor promotes hepatitis B virus-induced hepatocarcinogenesis through modulation of hepatitis B virus RNA transcription. Sci. Transl. Med. 2, 32ra35 (2010).
Naugler, W. E. et al. Gender disparity in liver cancer due to sex differences in MyD88-dependent IL-6 production. Science 317, 121–124 (2007).
Xu, C. et al. Sex differences in genomic features of hepatitis B–associated hepatocellular carcinoma with distinct antitumor immunity. Cell. Mol. Gastroenterol. Hepatol. 15, 327–354 (2023).
Klein, S. L, Pekosz, A, Passaretti, C, Anker, M & Olukoya, P. Sex, Gender and Influenza (World Health Organization: 2010).
Quandelacy, T. M., Viboud, C., Charu, V., Lipsitch, M. & Goldstein, E. Age- and sex-related risk factors for influenza-associated mortality in the United States between 1997–2007. Am. J. Epidemiol. 179, 156–167 (2014).
Robinson, D. P., Lorenzo, M. E., Jian, W. & Klein, S. L. Elevated 17β-estradiol protects females from influenza a virus pathogenesis by suppressing inflammatory responses. PLoS Pathog. 7, e1002149 (2011).
Lorenzo, M. E. et al. Antibody responses and cross protection against lethal influenza A viruses differ between the sexes in C57BL/6 mice. Vaccine 29, 9246–9255 (2011).
Creisher, P. S., Seddu, K., Mueller, A. L. & Klein, S. L. in Sex and Gender Differences in Infection and Treatments for Infectious Diseases (eds. Klein, S. L. et al.) 111–137 (Springer International, 2023).
Vermillion, M. S. et al. Production of amphiregulin and recovery from influenza is greater in males than females. Biol. Sex Differ. 9, 24 (2018).
Larcombe, A. N. et al. Sexual dimorphism in lung function responses to acute influenza A infection. Influenza Other Respir. Viruses 5, 334–342 (2011).
Robinson, D. P., Hall, O. J., Nilles, T. L., Bream, J. H. & Klein, S. L. 17β-estradiol protects females against influenza by recruiting neutrophils and increasing virus-specific CD8 T cell responses in the lungs. J. Virol. 88, 4711–4720 (2014).
Hall, O. J. et al. Progesterone-based therapy protects against influenza by promoting lung repair and recovery in females. PLoS Pathog. 12, e1005840 (2016).
Creisher, P. S. et al. Suppression of progesterone by influenza A virus mediates adverse maternal and fetal outcomes in mice. mBio 15, e03065-03023 (2024).
vom Steeg, L. G. et al. Androgen receptor signaling in the lungs mitigates inflammation and improves the outcome of influenza in mice. PLoS Pathog. 16, e1008506 (2020).
Huckestein, B. R. et al. Sex-based differences in persistent lung inflammation following influenza infection of juvenile outbred mice. Am. J. Physiol. Lung Cell. Mol. Physiol. 327, L189–L202 (2024).
Wang, C. et al. Sex disparities in influenza: a multiscale network analysis. iScience 25, 104192 (2022).
Fernandez-de-Las-Penas, C. et al. Symptoms experienced at the acute phase of SARS-CoV-2 infection as risk factor of long-term post-COVID symptoms: the LONG-COVID-EXP-CM multicenter study. Int. J. Infect. Dis. 116, 241–244 (2022).
Dhakal, S. et al. Sex differences in lung imaging and SARS-CoV-2 antibody responses in a COVID-19 golden Syrian hamster model. mBio 12, e0097421 (2021).
Ruiz-Bedoya, C. A. et al. 124I-Iodo-DPA-713 positron emission tomography in a hamster model of SARS-CoV-2 infection. Mol. Imaging Biol. 24, 135–143 (2022).
Takahashi, T. et al. Sex differences in immune responses that underlie COVID-19 disease outcomes. Nature 588, 315–320 (2020). This study provides one of the first detailed analyses of sex differences in the immune profile of individuals with COVID-19, demonstrating how immunological differences between the sexes correlate with distinct acute disease outcomes.
Montaño Mendoza, V. M. et al. Biological sex and age-related differences shape the antiviral response to SARS-CoV-2 infection. Heliyon 9, e13045 (2023).
Qin, L. et al. Gendered effects on inflammation reaction and outcome of COVID-19 patients in Wuhan. J. Med. Virol. 92, 2684–2692 (2020).
Scully, E. P. et al. Sex and gender differences in testing, hospital admission, clinical presentation, and drivers of severe outcomes from COVID-19. Open Forum Infect. Dis. 8, ofab448 (2021).
Qu, H. Q., Glessner, J. T., Kao, C. & Hakonarson, H. Data-informed insights into sex differences in peripheral blood mononuclear cells from single-cell transcriptomics. Genes Dis. 12, 101525 (2025).
Sauerwald, N. et al. Pre-infection antiviral innate immunity contributes to sex differences in SARS-CoV-2 infection. Cell Syst. 13, 924–931 (2022).
Agrawal, S., Salazar, J., Tran, T. M. & Agrawal, A. Sex-related differences in innate and adaptive immune responses to SARS-CoV-2. Front. Immunol. 12, 739757 (2021).
Masters, E. A. et al. Dissecting sex-specific pathology in K18-hACE2 transgenic mice infected with different SARS-CoV-2 variants. J. Med. Virol. 97, e70506 (2025).
Gupta, M., Srikrishna, G., Klein, S. L. & Bishai, W. R. Genetic and hormonal mechanisms underlying sex-specific immune responses in tuberculosis. Trends Immunol. 43, 640–656 (2022).
Bini, E. I. et al. The influence of sex steroid hormones in the immunopathology of experimental pulmonary tuberculosis. PLoS ONE 9, e93831 (2014).
Dibbern, J., Eggers, L. & Schneider, B. E. Sex differences in the C57BL/6 model of Mycobacterium tuberculosis infection. Sci. Rep. 7, 10957 (2017).
Hertz, D. et al. Turning the tables: loss of adaptive immunity reverses sex differences in tuberculosis. Immuno 5, 4 (2025).
Corica, B., Tartaglia, F., D’Amico, T., Romiti, G. F. & Cangemi, R. Sex and gender differences in community-acquired pneumonia. Intern. Emerg. Med. 17, 1575–1588 (2022).
Lopez-de-Andres, A. et al. Gender differences in incidence and in-hospital outcomes of community-acquired, ventilator-associated and nonventilator hospital-acquired pneumonia in Spain. Int. J. Clin. Pract. 75, e13762 (2021).
Kadioglu, A. et al. Sex-based differences in susceptibility to respiratory and systemic pneumococcal disease in mice. J. Infect. Dis. 204, 1971–1979 (2011).
Xiong, Y. et al. Estradiol resolves pneumonia via ERbeta in regulatory T cells. JCI Insight 6, e133251 (2021).
Yang, Z. et al. Female resistance to pneumonia identifies lung macrophage nitric oxide synthase-3 as a therapeutic target. eLife 3 (2014). This study demonstrates that estrogen drives NOS3 activation in lung macrophages, revealing a sex-specific protective pathway that underlie differential responses to pneumococcal pneumonia and highlighting NOS3 as a potential therapeutic target for treating infections.
Abid, S. et al. 17β-estradiol dysregulates innate immune responses to pseudomonas aeruginosa respiratory infection and is modulated by estrogen receptor antagonism. Infect. Immun. 85, e00422–17 (2017).
Pires, S., Peignier, A., Seto, J., Smyth, D. S. & Parker, D. Biological sex influences susceptibility to Acinetobacter baumannii pneumonia in mice. JCI Insight 5, e132223 (2020).
Linz, M. S. et al. Biological sex influences severity and outcomes in Acinetobacter baumannii pneumonia. Microbiol. Spectr. 13, e0319924 (2025).
Wang, Y., Cela, E., Gagnon, S. & Sweezey, N. B. Estrogen aggravates inflammation in Pseudomonas aeruginosa pneumonia in cystic fibrosis mice. Respir. Res. 11, 166 (2010).
Turner, J. R. Intestinal mucosal barrier function in health and disease. Nat. Rev. Immunol. 9, 799–809 (2009).
Sankaran-Walters, S. et al. Sex differences matter in the gut: effect on mucosal immune activation and inflammation. Biol. Sex Differ. 4, 10 (2013).
Goodman, W. A. et al. Impaired estrogen signaling underlies regulatory T cell loss-of-function in the chronically inflamed intestine. Proc. Natl Acad. Sci. USA 117, 17166–17176 (2020).
Homma, H. et al. The female intestine is more resistant than the male intestine to gut injury and inflammation when subjected to conditions associated with shock states. Am. J. Physiol. Gastrointest. Liver Physiol. 288, G466–G472 (2005).
Eggleston, F. C., Santoshi, B. & Singh, C. M. Typhoid perforation of the bowel experiences in 78 cases. Ann. Surg. 190, 31–35 (1979).
Ferro, A. et al. Sex differences in the prevalence of Helicobacter pylori infection: an individual participant data pooled analysis (StoP Project). Eur. J. Gastroenterol. Hepatol. 31, 593–598 (2019).
Ohtani, M. et al. 17 beta-estradiol suppresses Helicobacter pylori-induced gastric pathology in male hypergastrinemic INS-GAS mice. Carcinogenesis 32, 1244–1250 (2011).
Deltourbe, L., Lacerda Mariano, L., Hreha, T. N., Hunstad, D. A. & Ingersoll, M. A. The impact of biological sex on diseases of the urinary tract. Mucosal Immunol. 15, 857–866 (2022).
Olson, P. D., Hruska, K. A. & Hunstad, D. A. Androgens enhance male urinary tract infection severity in a new model. J. Am. Soc. Nephrol. 27, 1625–1634 (2016).
Olson, P. D. et al. Androgen exposure potentiates formation of intratubular communities and renal abscesses by Escherichia coli. Kidney Int. 94, 502–513 (2018).
Trautmann, A. Core features and inherent diversity of post-acute infection syndromes. Front. Immunol. 16, 1509131 (2025).
Johnson, D. & Jiang, W. Infectious diseases, autoantibodies, and autoimmunity. J. Autoimmun. 137, 102962 (2023).
Sylvester, S. V. et al. Sex differences in sequelae from COVID-19 infection and in long COVID syndrome: a review. Curr. Med. Res. Opin. 38, 1391–1399 (2022).
Gorenshtein, A., Leibovitch, L., Liba, T., Stern, S. & Stern, Y. Gender disparities in neurological symptoms of long COVID: a systematic review and meta-analysis. Neuroepidemiology 59, 426–440 (2025).
Moldofsky, H. & Patcai, J. Chronic widespread musculoskeletal pain, fatigue, depression and disordered sleep in chronic post-SARS syndrome; a case-controlled study. BMC Neurol. 11, 37 (2011).
Tansey, C. M. et al. One-year outcomes and health care utilization in survivors of severe acute respiratory syndrome. Arch. Intern. Med. 167, 1312–1320 (2007).
Wu, X., Dong, D. & Ma, D. Thin-section computed tomography manifestations during convalescence and long-term follow-up of patients with severe acute respiratory syndrome (SARS). Med. Sci. Monit. 22, 2793–2799 (2016).
Lee, S. H. et al. Depression as a mediator of chronic fatigue and post-traumatic stress symptoms in Middle East respiratory syndrome survivors. Psychiatry Investig. 16, 59–64 (2019).
Spetz, M., Natt Och Dag, Y., Li, H., Nyberg, F. & Rosvall, M. Covid-19 and cardiovascular disease in a total population-study of long-term effects, social factors and Covid-19-vaccination. Nat. Commun. 16, 10115 (2025).
Hamlin, R. E. et al. Sex differences and immune correlates of Long Covid development, symptom persistence, and resolution. Sci. Transl. Med. 16, eadr1032 (2024). The authors characterize sex-specific immune dysregulation using multi-omics profiling of immune cells from SARS-CoV-2-infected patients that either recover or develop long COVID. They identify sex differences in acute and persistent immune transcriptional responses and sex chromosome gene expression that may contribute to the higher risk of long COVID in female individuals.
Fulton, C. D., Beasley, D. W., Bente, D. A. & Dineley, K. T. Long-term, West Nile virus-induced neurological changes: a comparison of patients and rodent models. Brain Behav. Immun. Health 7, 100105 (2020).
Hoffman, K. W. et al. Sex differences in cytokine production following West Nile virus infection: implications for symptom manifestation. Pathog. Dis. 77, ftz016 (2019).
Lim, J. T. et al. Characterization of post-acute multi-organ sequelae following dengue infection. Clin. Microbiol. Infect. 31, 1865–1872 (2025).
García, G. et al. Long-term persistence of clinical symptoms in dengue-infected persons and its association with immunological disorders. Int. J. Infect. Dis. 15, e38–e43 (2011).
Hertanti, N. S., Nguyen, T. V. & Chuang, Y.-H. Global prevalence and risk factors of fatigue and post-infectious fatigue among patients with dengue: a systematic review and meta-analysis. EClinicalMedicine 80, 103041 (2025).
Seet, R. C., Quek, A. M. & Lim, E. C. Post-infectious fatigue syndrome in dengue infection. J. Clin. Virol. 38, 1–6 (2007).
Lazari, C. D. S. et al. Clinical markers of post-Chikungunya chronic inflammatory joint disease: a Brazilian cohort. PLoS Negl. Trop. Dis. 17, e0011037 (2023).
Ramachandran, V. et al. Impact of Chikungunya on health related quality of life Chennai, South India. PLoS ONE 7, e51519 (2012).
Bjornevik, K. et al. Longitudinal analysis reveals high prevalence of Epstein-Barr virus associated with multiple sclerosis. Science 375, 296–301 (2022).
Younis, S. et al. Epstein-Barr virus reprograms autoreactive B cells as antigen-presenting cells in systemic lupus erythematosus. Sci. Transl. Med. 17, eady0210 (2025).
Wormser, G. P. & Shapiro, E. D. Implications of gender in chronic Lyme disease. J. Womens Health 18, 831–834 (2009).
Rebman, A. W., Soloski, M. J. & Aucott, J. N. in Sex and Gender Differences in Infection and Treatments for Infectious Diseases (eds Klein, S. L. & Roberts, C. W.) 337–360 (Springer, 2015).
Johnson, L., Shapiro, M., Janicki, S., Mankoff, J. & Stricker, R. B. Does biological sex matter in Lyme disease? The need for sex-disaggregated data in persistent illness. Int. J. Gen. Med. 16, 2557–2571 (2023).
Aucott, J. N. et al. Risk of post-treatment Lyme disease in patients with ideally-treated early Lyme disease: a prospective cohort study. Int. J. Infect. Dis. 116, 230–237 (2022).
Girgis, A. A. et al. Aberrant T-cell phenotypes in a cohort of patients with post-treatment Lyme disease. Front. Immunol. 16, 1607619 (2025).
Zinck, C. B. et al. Pathogen strain and host sex influence infection prevalence and tissue spirochete load of Borrelia burgdorferi in its rodent host. Mol. Ecol. 31, 5872–5888 (2022).
Koloski, C. W. et al. Male C57BL/6J mice have higher presence and abundance of Borrelia burgdorferi in their ventral skin compared to female mice. Ticks Tick Borne Dis. 15, 102308 (2024).
Brouqui, P. et al. Chronic Q fever: ninety-two cases from France, including 27 cases without endocarditis. Arch. Intern. Med. 153, 642–648 (1993).
Textoris, J. et al. Sex-related differences in gene expression following Coxiella burnetii infection in mice: potential role of circadian rhythm. PLoS ONE 5, e12190 (2010).
Gay, L. et al. Impact of sex hormones on macrophage responses to Coxiella burnetii. Front. Immunol. 12, 705088 (2021).
Dominguez, A. et al. Seroprevalence of measles, rubella, and mumps antibodies in Catalonia, Spain: results of a cross-sectional study. Eur. J. Clin. Microbiol. Infect. Dis. 25, 310–317 (2006).
Mossong, J., O’Callaghan, C. J. & Ratnam, S. Modelling antibody response to measles vaccine and subsequent waning of immunity in a low exposure population. Vaccine 19, 523–529 (2001).
Riggenbach, M. M. et al. Mumps virus-specific immune response outcomes and sex-based differences in a cohort of healthy adolescents. Clin. Immunol. 234, 108912 (2022).
Hoes, J. et al. Comparison of antibody response between boys and girls after infant and childhood vaccinations in the Netherlands. Vaccine 37, 4504–4510 (2019).
Aldakak, L., Huber, V. M., Ruhli, F. & Bender, N. Sex difference in the immunogenicity of the quadrivalent human papilloma virus vaccine: systematic review and meta-analysis. Vaccine 39, 1680–1686 (2021).
Engler, R. J. et al. Half- vs full-dose trivalent inactivated influenza vaccine (2004–2005): age, dose, and sex effects on immune responses. Arch. Intern. Med. 168, 2405–2414 (2008).
Furman, D. et al. Systems analysis of sex differences reveals an immunosuppressive role for testosterone in the response to influenza vaccination. Proc. Natl Acad. Sci. USA 111, 869–874 (2014).
Nguyen, D. C. et al. 17β-estradiol restores antibody responses to an influenza vaccine in a postmenopausal mouse model. Vaccine 29, 2515–2518 (2011).
Pauklin, S., Sernandez, I. V., Bachmann, G., Ramiro, A. R. & Petersen-Mahrt, S. K. Estrogen directly activates AID transcription and function. J. Exp. Med. 206, 99–111 (2009).
Demonbreun, A. R. et al. COVID-19 mRNA vaccination generates greater IgG levels in women compared to men. J. Infect. Dis. 224, 793–797 (2021).
Visci, G. et al. Serological response after SARS-CoV-2 vaccination in healthcare workers: a multicenter study. Med. Lav. 113, e2022022 (2022).
Kageyama, T. et al. Antibody responses to BNT162b2 mRNA COVID-19 vaccine and their predictors among healthcare workers in a tertiary referral hospital in Japan. Clin. Microbiol. Infect. 27, 1861–1865 (2021).
Shapiro, J. R. et al. Association of frailty, age, and biological sex with SARS-CoV-2 mRNA vaccine-induced immunity in older adults. Clin. Infect. Dis. 75, S61–S71 (2022).
Lustig, Y. et al. BNT162b2 COVID-19 vaccine and correlates of humoral immune responses and dynamics: a prospective, single-centre, longitudinal cohort study in health-care workers. Lancet Respir. Med. 9, 999–1009 (2021).
Notarte, K. I. et al. Effects of age, sex, serostatus, and underlying comorbidities on humoral response post-SARS-CoV-2 Pfizer-BioNTech mRNA vaccination: a systematic review. Crit. Rev. Clin. Lab. Sci. 59, 373–390 (2022).
Tong, S. et al. COVID-19 mRNA or viral vector vaccine type and subject sex influence the SARS-CoV-2 T-cell response. Vaccine 61, 127420 (2025).
Levin, E. G. et al. Waning immune humoral response to BNT162b2 COVID-19 vaccine over 6 months. N. Engl. J. Med. 385, e84 (2021).
Oyebanji, O. A. et al. COVID-19 booster doses reduce sex disparities in antibody responses among nursing home residents. Clin. Exp. Res. 37, 73 (2025).
Chaulagain, S. et al. COVID-19 vaccine (NVX-CoV2373 and NVX-CoV2540) doses and virus strain match impact sex- and age-specific immunity and protection in mice. Vaccine 61, 127409 (2025).
Sparks, R. et al. Influenza vaccination reveals sex dimorphic imprints of prior mild COVID-19. Nature 614, 752–761 (2023).
Taquet, M., Dercon, Q., Todd, J. A. & Harrison, P. J. The recombinant shingles vaccine is associated with lower risk of dementia. Nat. Med. 30, 2777–2781 (2024).
St Clair, L. A., Chaulagain, S., Klein, S. L., Benn, C. S. & Flanagan, K. L. Sex-differential and non-specific effects of vaccines over the life course. Curr. Top Microbiol. Immunol. 441, 225–251 (2023).
Roth, A. et al. Tuberculin reaction, BCG scar, and lower female mortality. Epidemiology 17, 562–568 (2006).
Harikumar Parvathy, G. et al. Sex differences in vaccine-induced immunity and protection against Mycobacterium tuberculosis. J. Infect. Dis. 232, 1187–1197 (2025).
Nieuwenhuizen, N. E. et al. Weaker protection against tuberculosis in BCG-vaccinated male 129 S2 mice compared to females. Vaccine 39, 7253–7264 (2021).
Cook, I. F. Sexual dimorphism of humoral immunity with human vaccines. Vaccine 26, 3551–3555 (2008).
Chiarella, S. E., Jenkins, S. M., Park, M. A., Abraham, R. S. & Joshi, A. Y. Sex differences in antibody responses to the 23-valent pneumococcal polysaccharide vaccination. Ann. Allergy Asthma Immunol. 127, 509–510 (2021).
Ravichandran, S. et al. Distinct baseline immune characteristics associated with responses to conjugated and unconjugated pneumococcal polysaccharide vaccines in older adults. Nat. Immunol. 25, 316–329 (2024). This study examines how preexisting immune landscapes in older men and wmomen influence responses to two FDA-approved pneumococcal vaccines, providing a foundation for precision vaccination strategies in aging populations.
Tchalla, E. Y. I., Betadpur, A., Khalil, A. Y., Bhalla, M. & Bou Ghanem, E. N. Sex-based difference in immune responses and efficacy of the pneumococcal conjugate vaccine. J. Leukoc. Biol. 117, qiae177 (2024).
Scully, E. P., Morgan, R. & Klein, S. L. Precision vaccinology: making vaccines work better for women and men. J. Infect. Dis. 232, 756–759 (2025).