A new review suggests vitamin D does far more than support bones in early life, but says the strongest non-skeletal benefits still need firmer human evidence.
Key takeaways
Vitamin D is clearly important during the first 1,000 days for skeletal health, especially for preventing rickets and supporting early bone development.
The review suggests that vitamin D may also influence immune, metabolic, and selected neurodevelopmental pathways, providing biological plausibility as an early-life programming factor.
Evidence for most non-skeletal benefits in humans remains mixed, limited, and context-dependent, with stronger signals often observed in people or populations with vitamin D deficiency.
The authors argue that future research should move toward more personalized supplementation strategies, including consideration of genetics, baseline vitamin D status, and timing of exposure during pregnancy and early life.
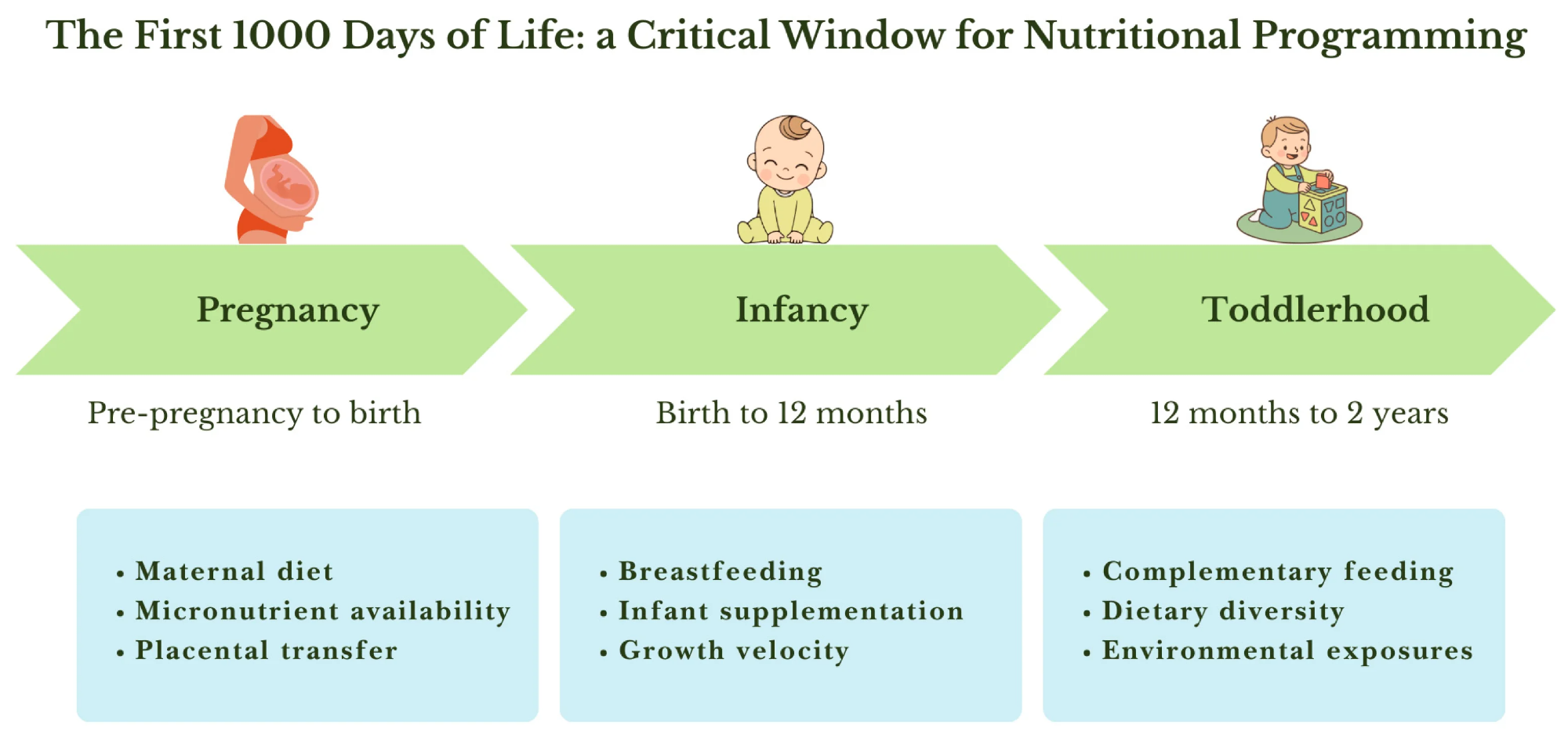
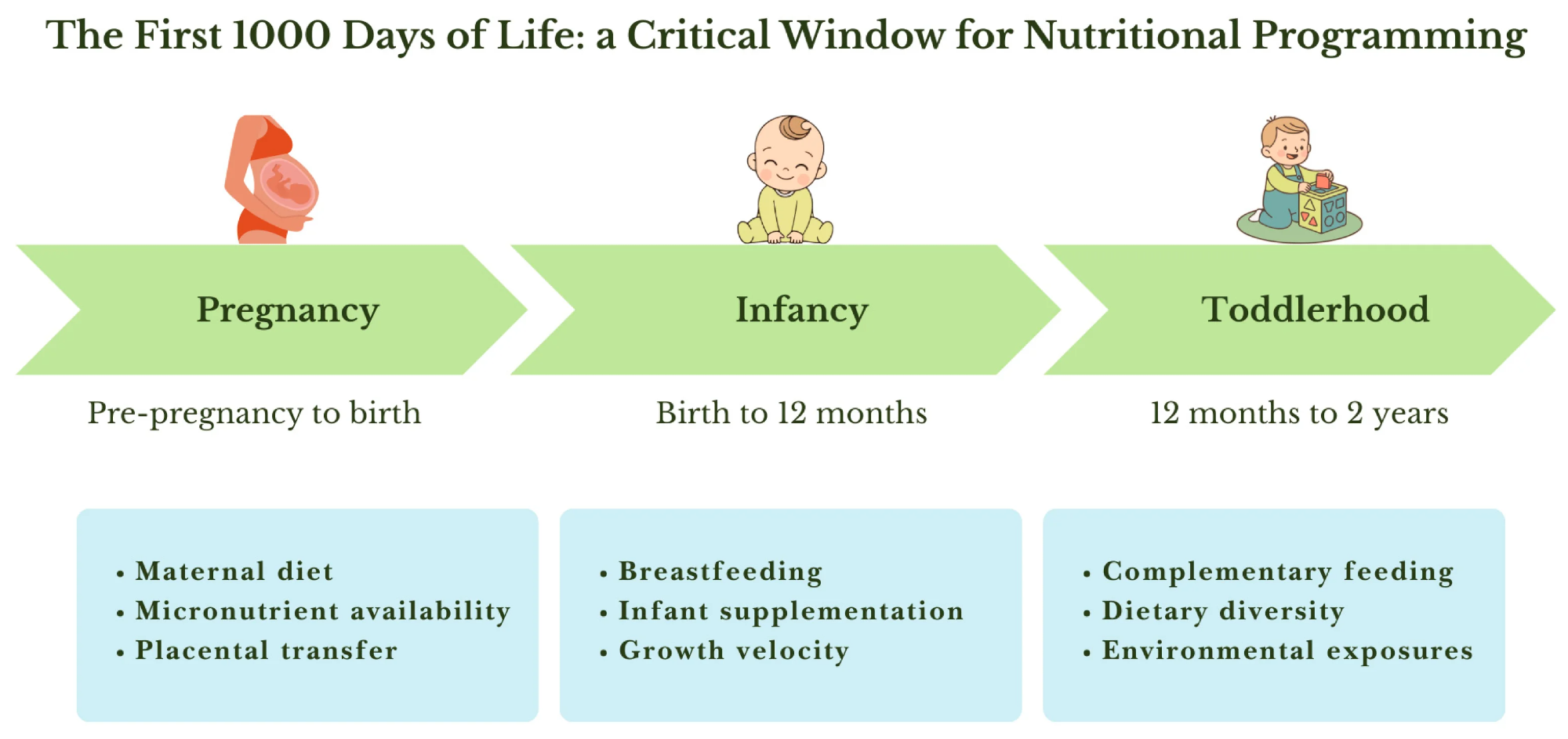
Key maternal, infant, and environmental factors influencing nutritional programming during pregnancy, infancy and toddlerhood.
In a recent review published in the journal Nutrients, researchers leveraged the Developmental Origins of Health and Disease (DOHaD) framework to evaluate the physiological role of vitamin D (vitD) during the first 1,000 days of human life.
The review revealed that early-life vitD is essential for the nutritional prevention of skeletal diseases such as rickets. More importantly, the review highlights emerging data indicating that vitamin D influences over 1,000 genes through the nuclear vitamin D receptor (VDR), with potential relevance to immune, metabolic, and selected neurodevelopmental health.
The review concludes that while vitamin D exhibits biological plausibility as a programming factor, current human clinical evidence for non-skeletal outcomes is nascent and incomplete, leading to heterogeneous, context-dependent findings.
Background
The first 1,000 days of a newborn’s life are now considered a “window of opportunity” as well as a “window of susceptibility” in pediatric practice, during which environmental stimuli significantly shape long-term health trajectories. Vitamin D, often termed the “sunshine vitamin,” has historically been studied for its role in calcium-phosphate homeostasis.
More recent research has shown that vitamin D has significant extraskeletal effects. Despite its critical role, vitamin D deficiency remains a global health concern, with estimates indicating that approximately 28% of the population is affected.
Meta-analyses of pregnant populations (n > 54,000) have found this group to be particularly vulnerable to vitamin D deficiency, with 54% demonstrating serum 25(OH)D levels below 20 ng/mL (50 nmol/L). Because neonatal stores are largely dependent on maternal transfer, maternal deficiency may predispose infants to adverse outcomes.
About the review
The present narrative review aimed to address this knowledge gap by synthesizing recent literature investigating the impacts of vitamin D across pregnancy, early life, infancy, and toddlerhood. Studies were identified from PubMed, Scopus, and Cochrane databases and included systematic reviews, meta-analyses, randomized controlled trials (RCTs), and high-quality observational studies.
The key outcomes investigated included biomarkers such as serum 25(OH)D concentrations, skeletal outcomes including bone mineral content (BMC) and bone mineral density (BMD), immune and metabolic indicators such as acute respiratory tract infections (ARTIs) and body mass index (BMI), and molecular pathways including transcriptomics and epigenetics.
The analyses also examined varying vitamin D dosing regimens, ranging from standard 400 IU/day supplementation to high-dose maternal interventions of 6,400 IU/day during lactation.
Review findings
Findings revealed that vitD is involved in several physiological functions across developmental domains.
For skeletal development, supplementation with 1,000 IU/day during pregnancy increased neonatal whole-body BMC, with some persistence into mid-childhood, although long-term clinical relevance remains uncertain.
For immune regulation, meta-analyses involving more than 48,000 participants showed a small reduction in ARTI risk with vitamin D supplementation, particularly at doses of 400-1,000 IU daily. However, effects were not significant in infants under 1 year old, indicating age-dependent responses.
For metabolic and birth outcomes, observational studies involving more than 35,000 mother-offspring pairs linked low maternal 25(OH)D levels to higher risks of small-for-gestational-age (SGA) infants and lower birth weights, although randomized trial data remain inconsistent.
For molecular programming, maternal supplementation was associated with reduced epigenetic gestational age acceleration and altered placental gene expression, though clinical implications remain uncertain.
Conclusions
The review supports vitamin D’s biological plausibility as an early-life nutritional programming factor. Its role extends beyond skeletal health to immune tolerance and possible neurodevelopmental effects, although evidence for these outcomes remains emerging and heterogeneous.
The 2024 Endocrine Society guidelines suggest empiric supplementation during pregnancy at approximately 2,500 IU/day, while emphasizing that non-skeletal benefits are not yet definitive.
Future research should adopt precision nutrition approaches that consider genetic variation, including polymorphisms in the vitamin D-binding protein (DBP), which may influence individual responses to supplementation.