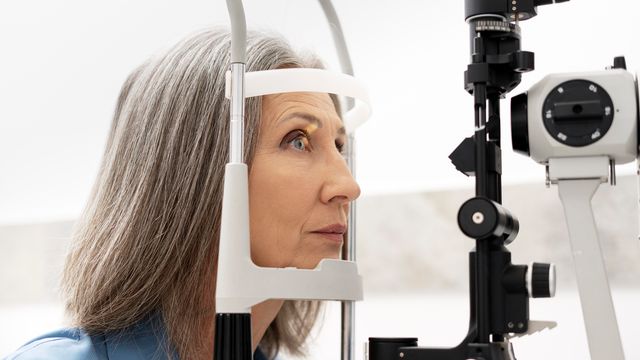
Glaucoma, a leading cause of blindness worldwide, occurs when the eye drainage system fails, leading to fluid buildup and increased pressure.
New research suggests the immune system may play a direct role in preventing that damage. In a study published in Immunity, scientists identified a specialized population of immune cells, known as resident macrophages, that help keep the eye’s drainage system functioning properly.
The study used fluorescently tagged resident macrophages in mouse eyes, finding that these cells regulate intraocular pressure (IOP) by controlling extracellular matrix turnover in the eye’s outflow tissues.
A persistent problem in glaucoma care
Current glaucoma treatments focus on lowering IOP, typically by reducing fluid production or improving its drainage, but these approaches do not always prevent disease progression.
“Despite our existing treatments, glaucoma remains a leading cause of permanent vision loss, with some patients still going blind from glaucoma,” said Dr. Katy Liu, assistant professor of ophthalmology at Duke Eye Center and lead author of the study. “New treatments that target the source of the disease are needed.”
Tracking immune cells in the eye
The researchers focused on macrophages, immune cells known for clearing debris and maintaining tissue health. While macrophages are abundant in the eye’s drainage pathway, their function in regulating pressure was unknown.
Using genetically engineered mice, the team tracked macrophage populations over time and distinguished between two types: long-lived resident macrophages, which persist in tissues, and monocyte-derived macrophages, which are continually replenished from the bloodstream.
They found that resident macrophages were concentrated in the region responsible for generating most of the eye’s outflow resistance, while monocyte-derived macrophages were more common in downstream vessels.
Removing the “cleanup crew”
To test function, the researchers selectively depleted resident macrophages. Within four days, this led to a measurable increase in IOP—from 16.9 to 18.4 mmHg—and a 59% reduction in outflow facility, a measure of how easily fluid exits the eye. They also found that extracellular matrix accumulated in the outflow tract, increasing resistance to fluid drainage.
“Resident macrophages are needed to maintain healthy intraocular pressure in the outflow tract,” Liu said. “Without them, extracellular matrix material accumulates in the outflow tract tissues and intraocular pressure increases.”
By contrast, removing monocyte-derived macrophages did not affect IOP or fluid dynamics, underscoring that not all immune cells in the tissue perform the same function. “We found that resident macrophages, but not all macrophages, work to maintain healthy IOP,” Liu said. “The function of other macrophage populations is currently unknown.”
Targeting the source of pressure dysregulation
The findings suggest that resident macrophages act to prevent buildup in the eye’s drainage pathway and preserve normal pressure. In glaucoma, dysfunction in this outflow system is a key driver of disease.
“In open-angle glaucoma, the most common form of glaucoma, the source of the disease is dysfunction in the outflow tract. Targeting resident macrophages would address the source of the pressure dysregulation, which the majority of glaucoma therapies do not currently do,” Liu explained.
While the study was conducted in mice, Liu is interested in determining whether similar mechanisms exist in humans: “Our next steps are to identify and compare resident macrophages and their functional roles in the outflow tract of healthy human eyes versus eyes with glaucoma.”
If confirmed, the findings could open the door to new treatments that go beyond lowering pressure and instead restore the normal function of the eye drainage system.
Reference: Liu KC, Grimsrud AO, Suarez MF, et al. Resident tissue macrophages maintain intraocular pressure homeostasis. Immunity. 2026. doi:10.1016/j.immuni.2026.01.025
About the interviewee:
Dr. Katy Liu is an associate professor in the Department of Ophthalmology at the Duke University Eye Center. She is a board-certified, glaucoma fellowship-trained glaucoma specialist and clinician-scientist with a PhD in Cell & Molecular Physiology, and her primary focus is to make basic science discoveries that can be translated from the bench to glaucoma patients.