As measles and pertussis cases surge across multiple states, researchers argue that the real vulnerability lies not only in individual choice but in the policies that allow immunity gaps to widen and outbreaks to take hold.
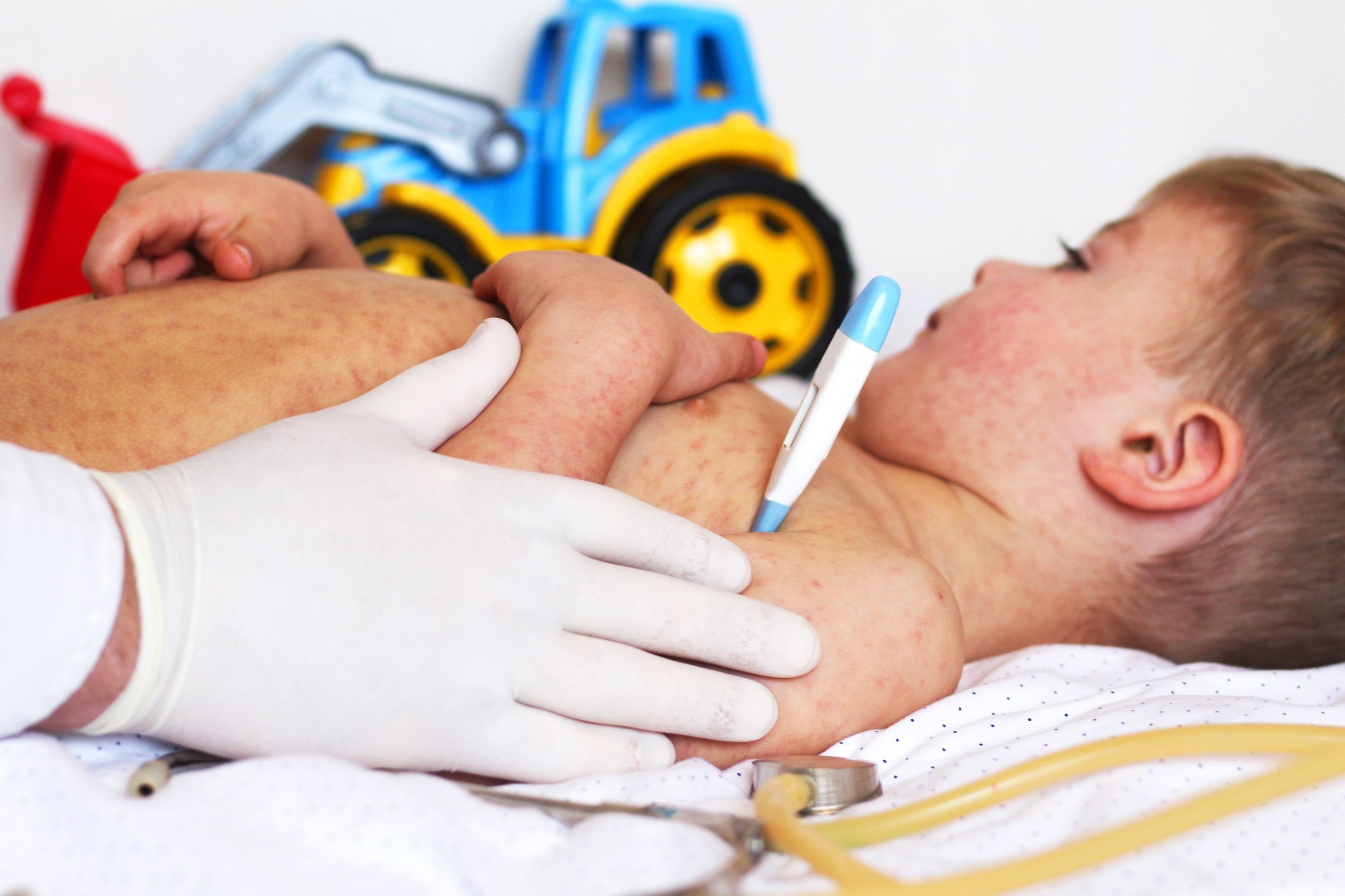
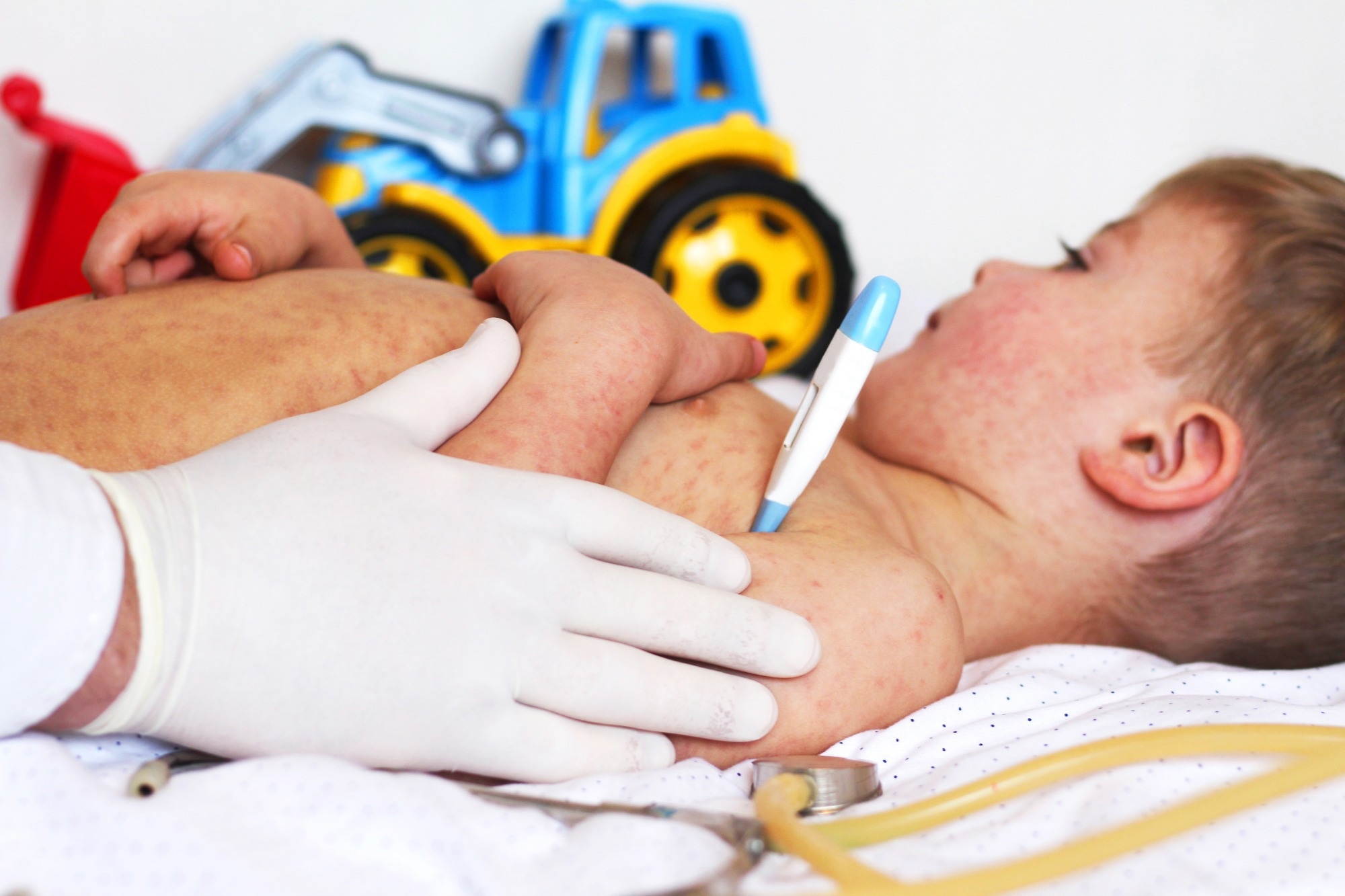
Commentary: Policy Failure, Not “Hesitancy”: Lessons From Recent Measles and Pertussis Outbreaks in the United States. Image Credit: fotohay / Shutterstock
In a recent commentary published in The Journal of Pediatric Pharmacology and Therapeutics, authors argue that recent outbreaks of vaccine-preventable diseases, such as pertussis (whooping cough) and measles, in the United States (US) have largely been framed as a crisis of vaccine hesitancy. However, they contend that these outbreaks are better explained by interacting policy failures and systemic failures, while acknowledging that vaccine hesitancy alone does not fully account for outbreak dynamics. Specifically, weakening immunization policies, permissive vaccine exemption laws, and insufficient investment in public health resources have contributed to rising case counts in several regions across the US.
Public Health Risks of Measles and Pertussis Resurgence
Measles remains one of the most contagious human infections and can lead to serious complications, including pneumonia, encephalitis, blindness, and death. Although effective vaccines are widely available, outbreaks continue to occur in the US. Pertussis also poses significant risks, particularly to infants and pregnant women. In these individuals, pertussis may result in apnea, pneumonia, and neurological injury.
Identifying the underlying causes of these outbreaks is essential. Determining whether recent resurgences reflect individual vaccine hesitancy or broader policy and systemic shortcomings is critical for guiding effective public health responses and strengthening immunization programs.
Commentary Argument: Policy Failures Beyond Vaccine Hesitancy
The authors argue that recent outbreaks of pertussis and measles in the US primarily reflect policy failures rather than vaccine hesitancy alone.
Outbreaks are frequently depicted as consequences of vaccination reluctance. However, the authors describe this framing as incomplete. They point to weakened immunization protections, liberal vaccine exemptions, and inadequate investment in public health systems as key contributors. In this context, policy environments determine whether localized pockets of hesitancy translate into sustained community transmission.
Epidemiological Evidence and Declining Herd Immunity
In 2024, more than 35,435 pertussis cases were recorded nationwide, a fivefold increase from 2023. Texas alone reported more than 3,500 pertussis cases by the end of October 2025, the highest number in more than a decade. Western Texas experienced its largest recorded measles outbreak in early 2025, with 762 laboratory-confirmed cases by August 2025, including severe disease and deaths. Additional outbreaks were reported across multiple US states.
In affected Texas counties, kindergarten vaccination rates fell below the 95 percent threshold typically associated with herd immunity. The authors suggest that when herd immunity declines due to policy gaps, outbreaks become more likely. Provisional school enrollment without complete vaccination documentation may allow susceptible individuals to cluster and facilitate transmission.
Policy Shifts, Exemptions, and Structural Weaknesses
The efficacy and safety of childhood vaccination have been demonstrated through decades of surveillance and research. The myth that vaccines cause autism spectrum disorder (ASD) persists despite repeated refutation in large-scale meta-analyses and cohort studies. The authors note that modern information ecosystems enable misinformation to spread rapidly, often amplified by technological systems and ideological polarization.
Liberal exemption policies, including non-medical exemptions and provisional school enrollment without adequate documentation, combined with inconsistent enforcement across districts, have created immunization gaps sufficient to permit disease transmission. Differences in vaccination coverage across Texas counties between 2023 and 2024 illustrate this pattern.
In 2025, Florida announced plans to eliminate compulsory childhood vaccine requirements for school attendance. If implemented, this policy would make Florida the first state to withdraw from conventional school vaccination mandates on the grounds of individual freedom and medical choice. Other states, including Texas, North Carolina, New Hampshire, and West Virginia, proposed legislation that could weaken school vaccination requirements, although none have fully repealed existing mandates.
Under-resourced health departments, particularly in rural areas, also contribute to delays in outbreak detection and containment due to limited surveillance and response capacity.
Recommended Policy and Public Health Interventions
The authors propose closing loopholes in provisional enrollment, re-establishing uniform enforcement of school vaccine requirements, expanding funding for mobile vaccination programs, and requiring near-real-time reporting to immunization registries.
They also recommend reevaluating liberal exemption policies that prioritize individual choice over collective safety. Strengthening maternal immunization programs through opt-out approaches integrated into routine prenatal care is another suggested strategy.
Investments in laboratory infrastructure, disease surveillance systems, and public health personnel are described as essential. Academic institutions and professional health societies are encouraged to treat vaccine misinformation as a patient safety issue. Licensing bodies should incorporate vaccine communication training into certification programs, and community-level partnerships require sustained funding and institutional support.
Policy Accountability and Future Outbreak Prevention
The commentary concludes that outbreaks are not random events but foreseeable consequences of policy shortcomings. Protecting population health is framed as a core public health responsibility. The authors caution that weakening immunization protections increases the likelihood of future outbreaks.
They emphasize that current disease resurgences reflect the interaction of structural determinants rather than a single cause. Addressing policy design, enforcement, and public health investment is therefore necessary to prevent future outbreaks and maintain community-level immunity.
Journal reference:
Kearns, G. L., Whitney, E., & Marshall, J. D. (2026). Policy Failure, not “Hesitancy”: Lessons from Recent Measles and Pertussis Outbreaks in the United States. The Journal of Pediatric Pharmacology and Therapeutics, 31(1), 115. DOI: 10.5863/JPPT-25-01224, https://pmc.ncbi.nlm.nih.gov/articles/PMC12888995/