Add DMNews to your Google News feed. ![]()
![]()
Tension: Millions of health-conscious adults stack popular supplements every morning believing they’re protecting their brains — but neurologists are finding that three common combinations may actually be accelerating cognitive decline.
Noise: The supplement industry positions its products as gentle, natural, and risk-free, while the cultural ritual of daily supplementation has become more about managing the fear of aging than addressing actual nutritional deficiencies.
Direct Message: The most protective thing you can do for your brain often isn’t adding another pill — it’s recognizing that the daily supplement ritual may be treating your anxiety about decline, not preventing it.
To learn more about our editorial approach, explore The Direct Message methodology.
Last March, Denise Kowalski — a 61-year-old retired school librarian in Raleigh, North Carolina — pulled out her phone to show her neurologist something she was proud of. It was a photo of her daily supplement lineup, arranged neatly on her kitchen counter like little soldiers of prevention: fish oil, a B-complex vitamin, calcium with vitamin D, magnesium, and a turmeric-curcumin capsule. Seven pills every morning, washed down with green tea. She’d been doing this for four years. She called it her “brain insurance.”
Her neurologist, reviewing the results of a cognitive screening that had come back slightly worse than the year before, wasn’t impressed. He was concerned. Not about any single supplement — but about three specific combinations she was taking simultaneously, every single day, without realizing they might be working against each other inside her brain.
Denise isn’t unusual. She’s the norm. According to the Council for Responsible Nutrition’s 2023 survey, roughly 75% of American adults take dietary supplements, and most take more than one. The assumption is intuitive and almost universal: if one good thing helps, stacking several good things helps more. But a growing number of neurologists and neuropharmacologists are pushing back on that logic — hard — and what they’re finding about certain popular combinations should make anyone with a pillbox pause.
The first combination raising alarms involves high-dose fish oil taken alongside blood-thinning supplements like vitamin E and ginkgo biloba. Individually, each has some evidence behind it. Omega-3 fatty acids support neuronal membrane integrity. Vitamin E is an antioxidant. Ginkgo has been marketed for decades as a memory booster. But together, in the doses many people self-prescribe, they create an anticoagulant effect that can reduce cerebral microcirculation in ways that paradoxically starve the brain of the steady oxygen flow it needs. Dr. Raymond Kelleher, a neurologist at Massachusetts General Hospital, told a 2023 symposium that he’s seen a noticeable uptick in patients over 55 presenting with accelerated white matter changes — a hallmark of brain aging — who were taking this exact trio. The mechanism isn’t dramatic. It’s slow. It’s the kind of thing that doesn’t show up on a blood panel but quietly erodes cognitive reserve over years.
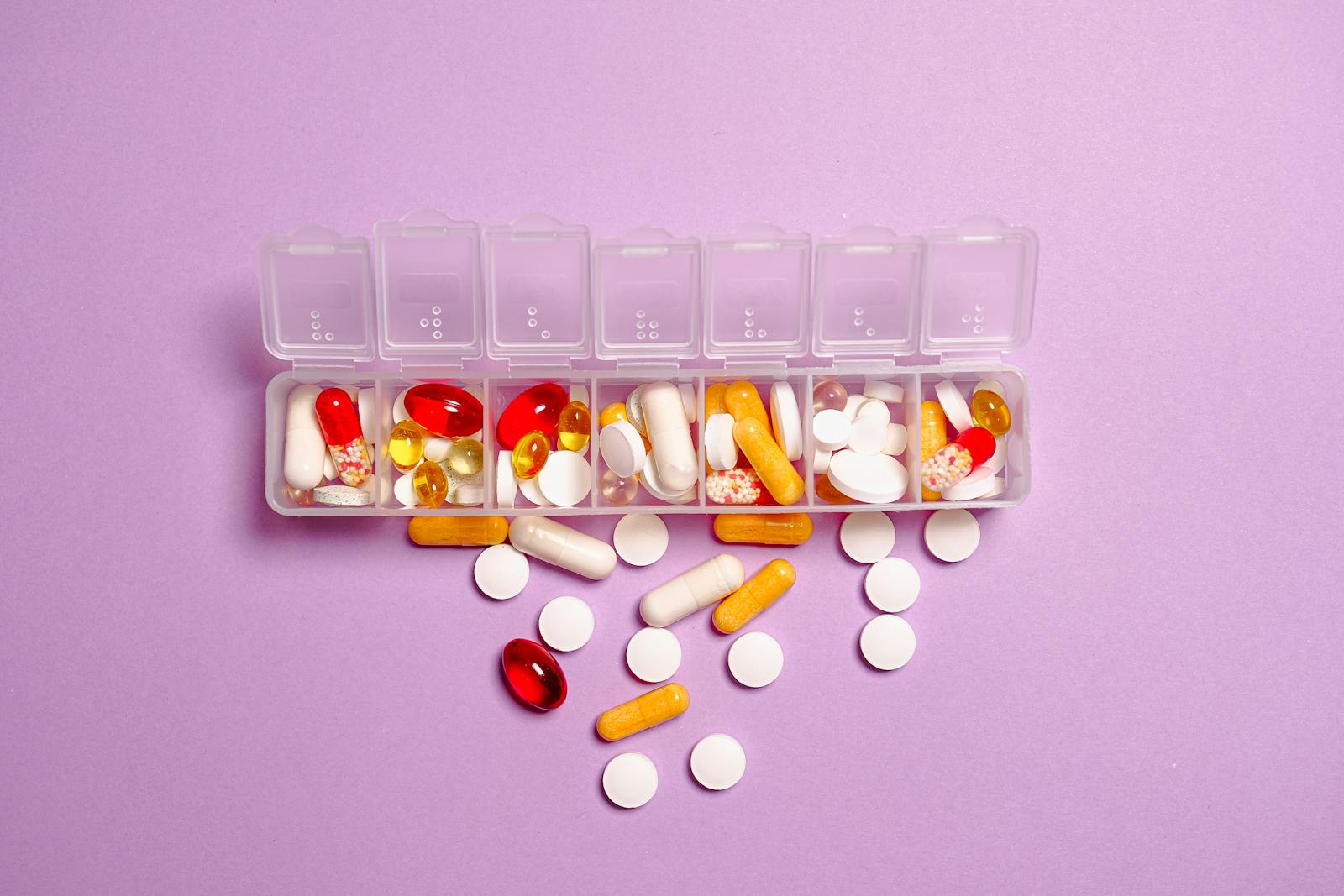
 Photo by Anna Shvets on Pexels
Photo by Anna Shvets on Pexels
The second problematic stack is one that surprises people because each component sounds so benign: calcium, vitamin D, and magnesium — often taken together, often recommended together. The issue isn’t the nutrients themselves. It’s the ratio and the dose. A 2020 study published in Neurology found that excess calcium supplementation — particularly when combined with moderate-to-high-dose vitamin D but without adequate magnesium balance — was associated with increased vascular calcification, including in the small vessels that feed the brain. Magnesium is supposed to be the balancing agent, but most over-the-counter magnesium is magnesium oxide, which has poor bioavailability. So people think they’re covered. They’re not. The calcium accumulates. The D pushes absorption higher. And the magnesium that’s supposed to prevent problems isn’t actually getting where it needs to go.
Marcus Reeves, a 54-year-old project manager in Phoenix, learned this the way most people do — accidentally. His wife had read about the importance of calcium after menopause, so they both started taking it. He added vitamin D after a blood test showed he was low. Magnesium came later, from a podcast recommendation. “I thought I was being responsible,” he said. When he mentioned persistent brain fog and difficulty concentrating to his doctor, nobody connected it to his supplement routine until a vascular screening showed early-stage calcification in his cerebral arteries. His neurologist told him something he’d never considered: the combination was likely making things worse, not better.
Stories like Marcus’s connect to something we explored in a recent piece on how popular supplement stacks may be accelerating brain aging — the pattern of well-intentioned people inadvertently engineering their own decline.
The third combination is perhaps the most culturally embedded: B-complex vitamins taken alongside iron and a stimulant like caffeine or guarana-based “energy” supplements. The B vitamins — particularly B6 and B12 — are essential for nervous system function. No argument there. But high-dose B6, when taken daily over extended periods, doesn’t just support nerves — it can become neurotoxic. The threshold is lower than most people assume. The FDA’s tolerable upper intake for B6 is 100mg per day, but many B-complex supplements contain 50-100mg, and people often combine them with fortified foods, energy drinks, and other sources without realizing they’re stacking doses. Add iron — which many women take routinely — and you introduce a potent pro-oxidant into the mix. Iron, in excess, doesn’t protect brain cells. It generates free radicals that accelerate neuronal damage, particularly in the hippocampus.
Sonia Achebe, a 47-year-old nurse practitioner in Atlanta, noticed tingling in her hands and intermittent word-finding difficulty that she initially attributed to stress. Her neurologist ordered a B6 level. It was nearly three times the upper limit. She’d been taking a B-complex, a multivitamin with additional B6, and drinking a fortified protein shake every morning — all with an iron supplement she’d been on since her twenties. “I’m a healthcare provider,” she said, “and I didn’t catch it in myself.”
 Photo by Tima Miroshnichenko on Pexels
Photo by Tima Miroshnichenko on Pexels
What makes these situations so insidious is the cultural framework around supplements. We’ve built an entire identity around being “proactive” about health. The supplement industry — now worth over $60 billion annually in the U.S. alone — has masterfully positioned its products as the opposite of pharmaceutical risk: natural, gentle, empowering. And there’s a psychological dimension to this that goes deeper than marketing. As psychologists have noted about brand attachment patterns, the things we reach for habitually often say more about our emotional needs than our physical ones. That daily supplement ritual isn’t just about nutrition. It’s about control — the feeling that we’re doing something in the face of aging, cognitive decline, and the terrifying randomness of neurodegeneration.
Neurologist Dr. Aparna Srinivasan, who practices in San Francisco, puts it bluntly: “The patients who come in with the most supplements are almost always the most anxious about cognitive decline. The supplements aren’t treating a deficiency — they’re treating a fear.” She’s noticed that these patients are also the hardest to counsel, because suggesting they stop taking something feels, to them, like being told to stop caring about their brain. Research on what actually accelerates aging suggests the protective factors that matter most — curiosity, social engagement, novel experience — can’t be swallowed in capsule form.
There’s also something worth noting about motivation and the brain’s capacity to protect itself. As recent neuroscience research on GLP-1 drugs has revealed, the brain has sophisticated internal systems for self-repair and motivation that we’re only beginning to understand — systems that often respond better to behavioral change than to biochemical supplementation.
A 2022 JAMA meta-analysis looking at supplement use and cognitive outcomes in adults over 60 found no significant benefit for any common supplement in preventing cognitive decline — and found signals of potential harm in several high-dose and multi-supplement scenarios. The authors were careful in their language, as researchers are. But the data was clear enough that several neurological societies have since updated their patient guidance.
Denise Kowalski, back in Raleigh, eventually worked with her neurologist to strip her routine down to a single, low-dose vitamin D supplement — the only one her blood work actually justified. She was surprised by how difficult it was to stop taking the rest. Not physically. Emotionally. “It felt like giving up on myself,” she said. It took weeks before she stopped reaching for the pill organizer out of habit.
That feeling — that stopping the ritual means abandoning the effort — is exactly where the real problem lives. It was never about the supplements. It was about the story we told ourselves while taking them: that vigilance equals protection, that more inputs mean more safety, that the daily act of swallowing seven pills was a form of love for our future selves. And sometimes the most protective thing we can do for our brains isn’t adding another capsule to the lineup. It’s having the clarity — and the courage — to put the bottle down and ask whether the thing we’ve been doing every morning is actually the thing that’s been quietly working against us all along.
Feature image by Supplements On Demand on Pexels







