Add DMNews to your Google News feed. ![]()
![]()
Tension: A woman followed her neurologist’s supplement recommendations faithfully for two years, only to discover a new study suggesting her specific combination may have been undermining the very brain repair processes she was trying to support.
Noise: We’ve built a culture of cognitive self-defense around supplement stacks, but the combinatorial science is shockingly thin. Individual nutrients studied in isolation behave differently when taken together over years, and the regulatory framework doesn’t require anyone to test the combinations consumers are actually taking.
Direct Message: The daily supplement ritual is often less about chemistry than control. The traits that actually protect cognition across decades — deep engagement, resilience, sustained curiosity — can’t be swallowed with a glass of water, and the most protective thing you can cultivate may be an honest relationship with uncertainty itself.
To learn more about our editorial approach, explore The Direct Message methodology.
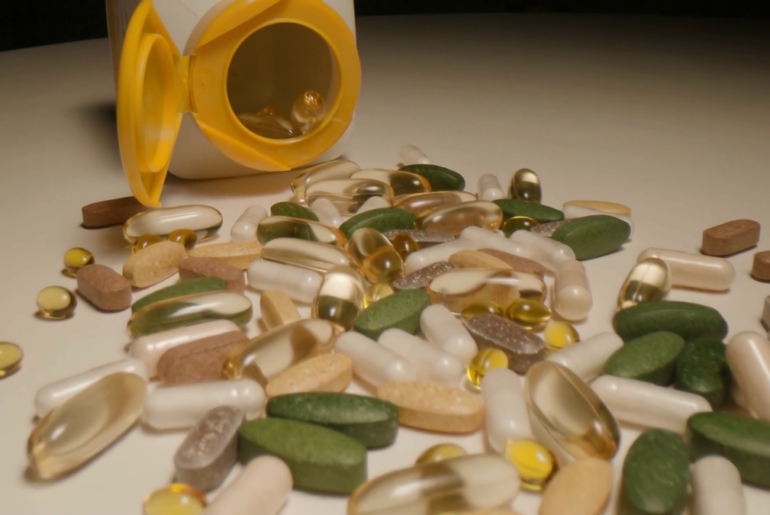
Denise, a 51-year-old speech pathologist in Portland, kept her supplements in a ceramic bowl on the kitchen counter, right next to the coffee maker. Every morning: omega-3 fish oil, vitamin E, a B-complex, curcumin, and a phosphatidylserine capsule. Her neurologist had recommended the combination after her mother’s Alzheimer’s diagnosis at 74, when Denise asked what she could do now, before anything started. The neurologist wasn’t cavalier about it. She reviewed Denise’s bloodwork, her family history, her diet. She made thoughtful, evidence-based selections. Denise felt something rare in American healthcare: the sensation of being proactive rather than reactive.
For two years, she took every capsule without missing a day. She felt sharper, slept better, noticed fewer of those mid-afternoon word-finding lapses that had started creeping in around 48. Then, in late 2023, a study published in Neurology suggested that high-dose combinations of certain antioxidants and fat-soluble vitamins may, under specific conditions, interfere with the brain’s natural cellular cleanup mechanisms rather than support them. The very combination she’d been taking faithfully may have been undermining the autophagy process her brain needed most.
Denise didn’t panic. She called her neurologist. But what she felt in that phone call was something quieter than fear. It was a specific kind of betrayal, the kind that comes when you did everything right and the ground still shifted beneath you.
I’ve been thinking about Denise a lot, because her story illuminates something uncomfortable about the way we approach cognitive decline in this country. We’ve built an entire culture around the idea that the brain is a machine you can maintain with the right inputs: the correct stack of supplements, the optimal morning routine, the precise Mediterranean diet ratio. And the people who buy into this framework most deeply aren’t reckless wellness influencers. They’re careful, science-literate people following credentialed advice.
 Photo by Anna Shvets on Pexels
Photo by Anna Shvets on Pexels
Marcus, 63, a retired civil engineer in Tucson, described a similar experience. His cardiologist had green-lit a regimen of CoQ10, alpha-lipoic acid, and high-dose vitamin E after a mild cardiac event in 2021. Marcus did his own research on top of it, reading abstracts, cross-referencing dosages. He felt confident. Then his wife forwarded him a piece about supplements working against each other, and he started asking questions he hadn’t considered before. Could the alpha-lipoic acid be recycling the vitamin E into a pro-oxidant form at those doses? Was the CoQ10 altering his mitochondrial membrane dynamics in ways that compounded rather than complemented?
His doctor’s honest answer: “We don’t fully know yet.”
That phrase, “we don’t fully know yet,” deserves more attention than it gets. Nutritional neuroscience operates in a strange epistemological space. Individual nutrients have been studied extensively in isolation. Omega-3s show neuroprotective effects in controlled trials. Curcumin demonstrates anti-inflammatory properties in animal models. B-vitamins reduce homocysteine, a known risk marker. But the combinatorial pharmacology of taking five, six, seven supplements simultaneously? The long-term interaction effects across years? The research is astonishingly thin.
A 2023 meta-analysis in The Lancet Healthy Longevity examined 28 randomized trials of multi-supplement regimens for cognitive health and found that combinations of antioxidant supplements showed no consistent benefit for preventing dementia, and in some subgroups (particularly those already taking statins or blood thinners), certain combinations were associated with faster biomarker progression. The authors used careful language. They always do. But the implications were stark: the supplement stack millions of Americans take for brain health may, in aggregate, behave differently than the sum of its parts.
Psychologists have a term for what happens when we encounter information that contradicts a deeply held protective behavior. It’s called effort justification dissonance, the more we’ve invested in a practice, the harder it becomes to accept that the practice may have been neutral or harmful. Denise told me she kept taking her supplements for three weeks after reading the study. Not because she’d rejected the findings. Because stopping felt like surrendering to the thing she feared most.
There’s a cultural dimension here too. As recent research into proteins that may prevent brain aging has shown, the science of cognitive decline is moving fast, often faster than clinical guidelines can absorb. Your neurologist’s recommendation from 2021 might genuinely conflict with the best evidence of 2024. That’s how science works, but it creates a strange situation for patients: the advice you followed wasn’t wrong when you received it. It became complicated retroactively.
Kira, 44, a data analyst in Chicago, never took supplements based on a doctor’s advice. She built her own stack from PubMed abstracts and longevity podcasts. Lion’s mane, bacopa monnieri, a racetam compound she ordered from a European vendor, CDP-choline, and magnesium threonate. When I asked her how she decided on that combination, she described a process that sounded remarkably like building a stock portfolio: diversification across pathways, hedging neuroinflammation against synaptic plasticity against mitochondrial support. It was impressive, genuinely. And it also represented an enormous act of faith in her own ability to integrate research she’d never been trained to evaluate in combination.
Kira’s situation points to something broader. The supplement industry exists in a regulatory gray zone where individual ingredients can be studied and marketed, but nobody is required to study what happens when a consumer combines eight of them based on separate recommendation threads. We’ve essentially crowdsourced our own polypharmacy without the safeguards that exist in prescription medicine. As one family’s devastating experience showed, the consequences can unfold slowly and silently enough that you mistake deterioration for aging itself.
What strikes me about all three of these people is that none of them were acting irresponsibly. Denise followed her neurologist. Marcus consulted a cardiologist and did his own reading. Kira went directly to the primary literature. They each represent a different tier of the same hierarchy of trust, and the emerging evidence is challenging all three tiers simultaneously.
I think the discomfort here goes deeper than supplements. It touches something fundamental about how we relate to our own vulnerability. The supplement stack is, at its core, a tangible ritual of control. You open the bottles, you swallow the capsules, you do the thing. In a landscape where cognitive decline can feel like an approaching storm with no shelter, the daily ritual becomes its own form of shelter. And research on super-agers suggests the traits that actually protect cognition over decades are far less purchasable: deep social engagement, psychological resilience, sustained curiosity, the willingness to remain uncomfortable.
Denise eventually adjusted her regimen. She dropped the vitamin E and reduced the curcumin, kept the fish oil at a lower dose. Her neurologist, to her credit, initiated the conversation herself once the new data circulated. But what Denise carries now isn’t updated dosing. It’s something harder to metabolize: the recognition that care and certainty are not the same thing. That you can do everything a thoughtful, credentialed professional recommends and still find yourself on the wrong side of emerging evidence.
The supplements in the ceramic bowl are still there. Fewer of them now. She told me she sometimes pauses before reaching for them, just for a second, in a way she never used to. That pause contains something the capsules never could. An honest reckoning with the limits of what we can control, and a quiet decision to keep trying anyway, knowing the ground might shift again.
That pause might be the most neuroprotective thing she does all morning.
Feature image by Hoàng Ngọc Long on Pexels