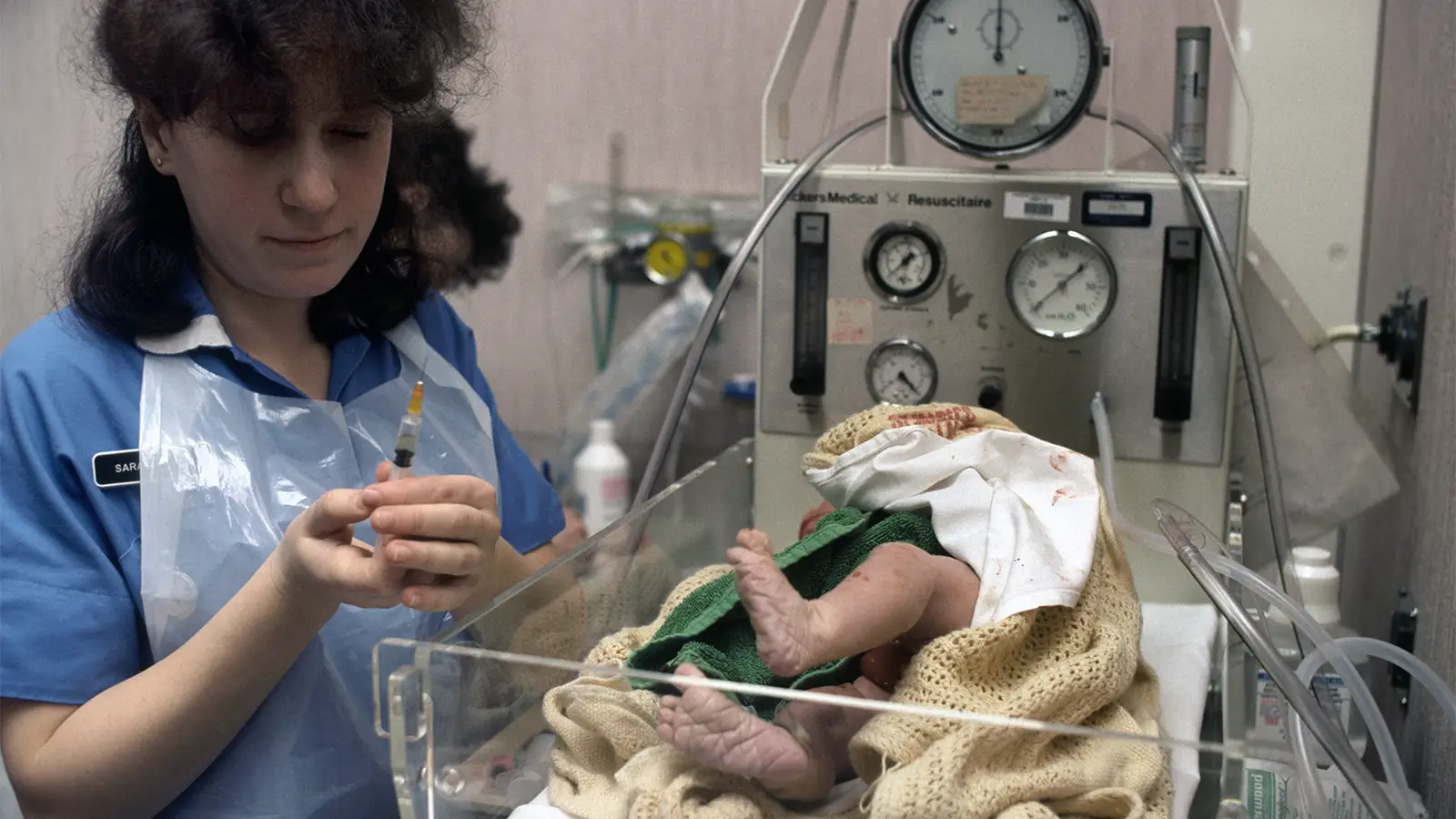
More parents refused to let newborn children have vitamin K shots, which may lead to vitamin K deficiency bleeding and future brain complications, a systematic literature review showed.
Refusal in the U.S. remained low but upward trends were evident, reported Kate Semidey, MD, of Florida International University in Miami, and co-authors in an abstract released ahead of the American Academy of Neurology annual meeting.
“Vitamin K at birth is safe and effective, and while refusal is still uncommon with rates in the United States remaining under 1% in most hospitals, our review found in recent years, there have been increases in parents refusing this supplement for their newborns,” Semidey said in a statement.
“This trend is concerning because our review also found that babies who do not get the vitamin K injection are 81 times more likely to develop vitamin K deficiency bleeding,” she added.
Vitamin K injections at birth prevent vitamin K deficiency bleeding, a rare but severe condition. The American Academy of Pediatrics has recommended the vitamin K shot since 1961. Routine newborn prophylaxis since then has nearly eliminated vitamin K deficiency bleeding in the U.S.
Late vitamin K deficiency bleeding occurs 1 week to 6 months after birth and often presents with intracranial hemorrhage, carrying 15% to 20% mortality and up to 50% long-term neurological disability, Semidey and colleagues said. “Despite proven safety, refusal of intramuscular vitamin K is rising worldwide, paralleling vaccine hesitancy,” they noted.
The review comes on the heels of research recently published in JAMA led by Kristan Scott, MD, of the Children’s Hospital of Philadelphia. Based on Epic electronic health records from 403 U.S. hospitals, Scott and colleagues showed that the percentage of infants not receiving intramuscular vitamin K rose from 2.92% in 2017 to 5.18% in 2024.
“We know unequivocally that infants who do not receive vitamin K are at significantly higher risk of serious bleeding,” Scott told MedPage Today.
“This could look like bleeding into their skin, their [gastrointestinal] tract, and even their brain, which could lead to significant complications, including death,” she said. “If this trend continues, more and more babies will be at risk for serious bleeding that is truly preventable.”
Semidey and co-authors conducted a systematic review of literature from 2005 to 2025, analyzing data from 25 peer-reviewed studies that met their inclusion criteria.
Refusal rates rose from 0.9% in 2015 to 1.6% in 2019 in Minnesota, they found. In California, Connecticut, and Iowa, refusal ranged from 0.2% to 1.3% in 2018 and 2019, with more than half of healthcare professionals perceiving increases.
In other countries, refusal rates ranged from 1% to 3% in Canada, New Zealand, and Scotland, and was over 30% in some birthing centers, Semidey and colleagues said.
Infants without intramuscular vitamin K prophylaxis were 81 times more likely to develop late vitamin K deficiency bleeding, they reported. Case series of vitamin K deficiency bleeding in infants showed that approximately 63% had intracranial hemorrhage, 40% had sustained neurological disabilities, and 14% died.
In the U.S., parents who refused vitamin K were 90 times more likely to reject both the hepatitis B vaccine and ocular prophylaxis to protect against potentially blinding infections. In Canada, those who refused vitamin K were 14.6 times more likely to not have their child vaccinated by age 15 months; in New Zealand, they were 14.1 times more likely.
Risk factors included home birth, midwife care, and “natural” philosophies, the researchers said. Parental concerns included pain, preservatives, and misinformation, they added.
“Vitamin K refusal, though uncommon, is rising and poses disproportionate neurological risk, leading to preventable infant death and lifelong disability. It also marks broader healthcare hesitancy,” Semidey and co-authors wrote.
“For neurologists, this trend signals growing burdens of avoidable developmental disorders,” they pointed out. “Universal uptake requires prenatal counseling, targeted messaging, and policy safeguards to reduce preventable neurodevelopmental disability.”