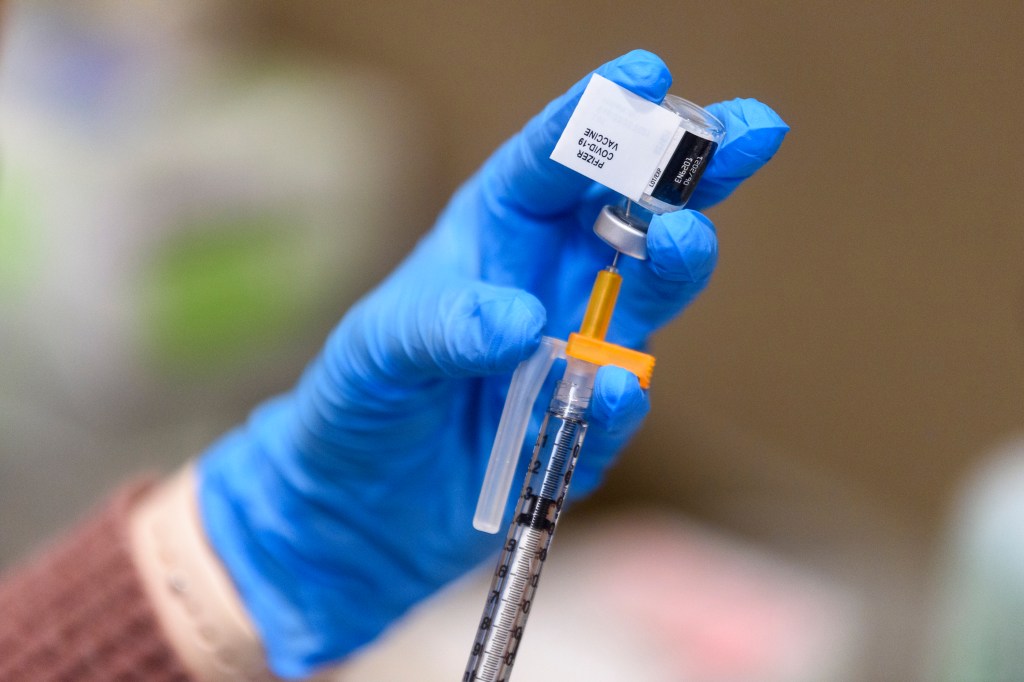
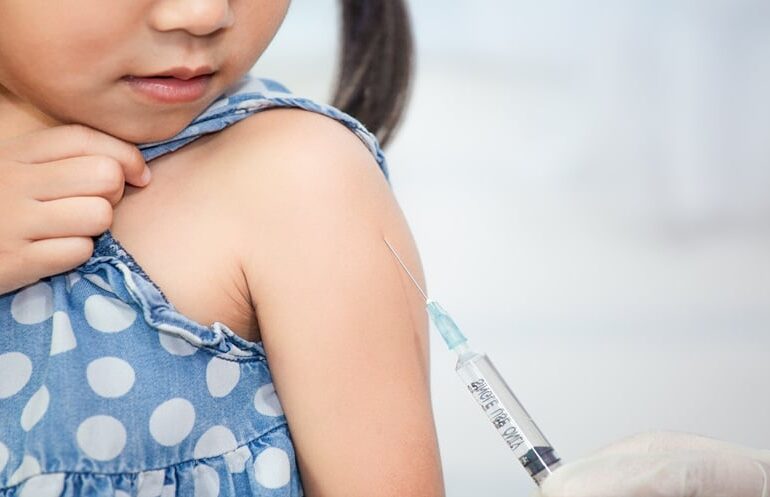
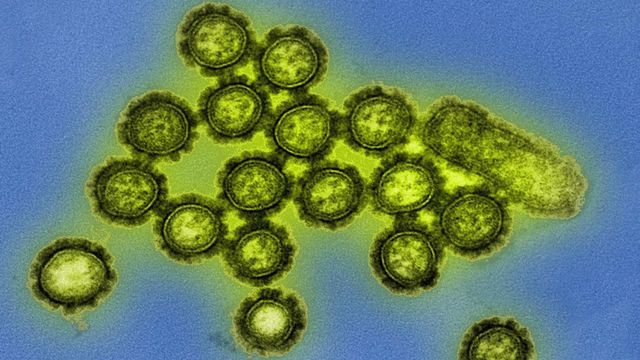
“[O]f course, we’re not going to take vaccines away from anybody. We are going to make sure that Americans have good information right now.”
That is what we were told by Robert F. Kennedy Jr., head of Health and Human Services, a year ago. In the months since, the resurgence of measles and threats to vaccine access have become all too apparent. The Center for Disease Control’s Advisory Committee on Immunization Practices (ACIP) has been almost completely overhauled and replaced with vaccine skeptics. In January, HHS unilaterally announced changes to the childhood immunization schedule, dropping the number of recommended vaccines from 17 to 11 based on flawed and misleading comparisons to other countries, particularly Denmark—a process that flies in the face of internationally established guidance on evidence-based decision-making. All the while, the number of measles cases in the US has soared to over 3,500 since January 2025.
Hospitals fighting measles confront a challenge: Few doctors have seen it before
On March 5, the Public Health Committee of the Connecticut state legislature tooks steps to protect vaccine access given the changes to ACIP and national recommendations. The primary purpose of Raised Bill 450 and HB 5044 is to protect access to vaccines to those who want them by strengthening the authority of the Commissioner of the Department of Public Health to establish vaccine policy in the state rather than relying solely on the ACIP-recommended schedule.
The bills ensure that vaccines recommended by the commissioner will be available to all parents who wish to have their child vaccinated by protecting Connecticut’s ability to purchase childhood vaccines, requiring all state-regulated health insurance plans to cover the recommended vaccines, and ensuring that pharmacists will be permitted to administer vaccines. The bills also seek to preclude challenges to some mandatory immunization requirements, for instance by allowing for religious exemptions.
A public hearing on the bill drew hundreds of people in opposition. Many of the arguments put forth echo those of the “medical freedom” movement, arguing that individuals have a right to choose their preferred medical treatments without government interference. It may sound reasonable. But when it comes to vaccines, it ignores the fact that most vaccines not only protect the people receiving them from getting really sick if exposed to an infectious disease—they also reduce the chances that they spread the infection to others around them, a concept known as “herd immunity”.
Herd immunity is about more than just eliminating transmission by reaching an often unattainable threshold of population-level protection. Vaccines can reduce the chances of experiencing the most severe symptoms of a disease. And by preventing some infections, or just reducing symptoms and the infectiousness of breakthrough cases among vaccinated individuals, vaccines reduce the chances of spreading the disease to others, including those too young to be vaccinated or who are unlikely to respond to the vaccine.
Vaccines are often not as effective for those who need them the most. As we age, our immune systems don’t work as well—a phenomenon known as “immune senescence.”
Immunocompromised individuals also do not respond as well to vaccines and in some cases may not be eligible for them. Very young infants have antibodies from their mother that may interfere with their own immune response, including to measles vaccine. Therefore, it is best to minimize the chances that they are exposed to the disease by ensuring those around them are vaccinated.
It’s true that in very rare instances, vaccines can cause severe side effects, such as Guillain-Barre syndrome, a temporary form of paralysis caused by the immune system attacking nerve cells. More often, vaccines can make you feel lousy the next day. However, these conditions can also be triggered by the infections themselves. The risks of getting infected and possibly being hospitalized or dying far outweigh the risks associated with vaccines.
Vaccine requirements are not about getting every single person vaccinated. They can—and should—allow for exemptions for medical reasons. But making vaccination an “opt out” rather than “opt in” decision is often sufficient to encourage people to receive a vaccine or have their children vaccinated. By doing so, school-based vaccine requirements have been shown to decrease rates of measles, influenza, and other illnesses in the community more broadly.
Nevertheless, new legal challenges to vaccine requirements for schooling are working their way through the courts. These too will make us less safe, subjecting us to the risk of diseases that were once a scourge of the past returning to our state. We need to enhance access to and uptake of vaccines in Connecticut, not turn away from these proven public health measures.
For over a century, there has been a national consensus on this issue, where “medical freedom” has its limits. In the 1905 Supreme Court case Jacobson vs Massachusetts, the court ruled that states had the authority to require individuals to get vaccinated (or face a fine) in the midst of a smallpox epidemic, saying:
“[T]he rights of the individual in respect of his liberty may at times, under the pressure of great dangers, be subjected to such restraint, to be enforced by reasonable regulations, as the safety of the general public may demand.”
Vaccines are not just about personal medical choice. Your decision to get vaccinated—or not—has repercussions for the entire population, including the “safety of the general public” that Supreme Court Justice Harlan invokes above. For that reason, government intervention to incentivize vaccination and increase uptake is not only reasonable, but necessary. Raised Bill 450 and HB 5044 deserve our support and the support of all who care about the welfare of the residents of our state, young and old.
Virginia E. Pitzer is a professor of epidemiology at Yale School of Public Health. Her research focuses on the population-level impact of vaccines. She has served on numerous World Health Organization committees responsible for reviewing evidence to support vaccine policy recommendations.
Gregg S. Gonsalves is an associate professor of epidemiology at Yale School of Public Health and an associate professor (adjunct) at the Yale Law School. His research focuses on the impact of public policies on infectious disease control.