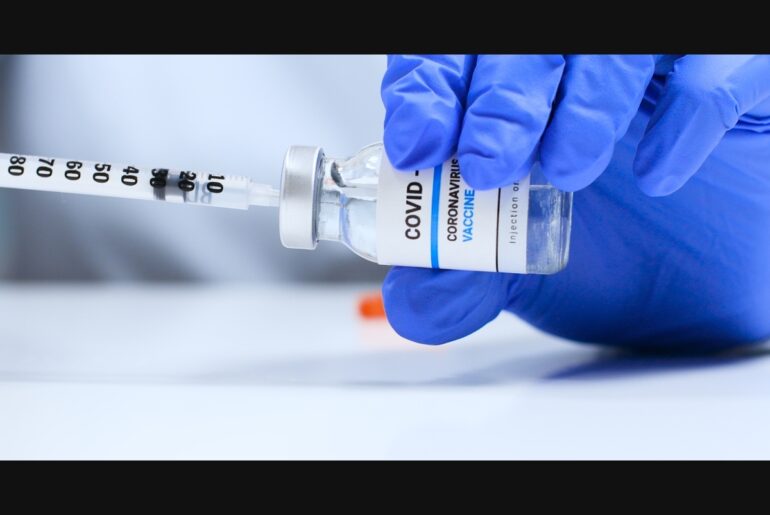
 Immunotherapy is changing the landscape of cancer care by leveraging the body’s natural defenses to combat tumors. This innovative treatment offers long-lasting benefits with reduced side effects for numerous patients; however, it may not be universally effective due to challenges like tumor evasion strategies and immune suppression. The idea sounds almost poetic. The body, designed to protect itself, turns its own defence system against cancer. For decades, this felt like a far-fetched goal. Today, it is part of real treatment plans across hospitals worldwide.Immunotherapy has changed how doctors approach cancer. It does not attack the disease directly like chemotherapy. Instead, it helps the immune system do what it was always meant to do, recognise and destroy harmful cells.But the story is not simple. Some patients see remarkable results. Others do not respond at all. That contrast raises an important question: when does this treatment work, and why does it sometimes fail?
Immunotherapy is changing the landscape of cancer care by leveraging the body’s natural defenses to combat tumors. This innovative treatment offers long-lasting benefits with reduced side effects for numerous patients; however, it may not be universally effective due to challenges like tumor evasion strategies and immune suppression. The idea sounds almost poetic. The body, designed to protect itself, turns its own defence system against cancer. For decades, this felt like a far-fetched goal. Today, it is part of real treatment plans across hospitals worldwide.Immunotherapy has changed how doctors approach cancer. It does not attack the disease directly like chemotherapy. Instead, it helps the immune system do what it was always meant to do, recognise and destroy harmful cells.But the story is not simple. Some patients see remarkable results. Others do not respond at all. That contrast raises an important question: when does this treatment work, and why does it sometimes fail?
What is immunotherapy, really?
Immunotherapy is a type of cancer treatment that strengthens or restores the body’s immune response against cancer cells.Under normal conditions, the immune system identifies abnormal cells and eliminates them. Cancer, however, is clever. It finds ways to hide or shut down this response.Immunotherapy steps in to remove those barriers.A widely used form is checkpoint inhibitors. These drugs target proteins like PD-1 or CTLA-4, which act as “brakes” on immune cells. Once these brakes are lifted, immune cells can attack cancer more effectively.According to the US National Cancer Institute (NCI), immunotherapy is now approved for several cancers, including melanoma, lung cancer, and kidney cancer.
How does it actually work inside the body?
The immune system relies heavily on T cells. These are specialised cells that detect and kill infected or abnormal cells.Cancer cells, however, can send signals that confuse these T cells. They may appear “normal” or actively suppress immune activity.Immunotherapy works in a few key ways:It helps T cells recognise cancer cellsIt boosts the strength of immune responsesIt blocks signals that prevent immune attacksThink of it as removing a disguise from cancer and handing the immune system a clearer target.Clinical research supported by the National Institutes of Health (NIH) shows that this approach can lead to long-lasting responses in certain cancers. 
It has transformed treatment for several cancers, offering long-lasting results in some patients. However, it does not work for everyone due to factors like immune suppression and tumour behaviour.
Why doctors call it a ‘game changer’
Unlike traditional treatments, immunotherapy can sometimes offer durable results. That means patients continue to benefit even after treatment stops.Dr Amit Rauthan explains it clearly, “Checkpoint inhibitors are immunotherapy drugs which unblock the body’s own ‘T’ lymphocyte cells to become active and fight cancer cells. They are now utilised in the treatment of multiple cancers and they have the advantage of giving durable long responses in responding patients with very limited side effects.”This shift matters. In cancers like advanced melanoma, survival rates have improved significantly in recent years because of immunotherapy.It also tends to have fewer systemic side effects compared to chemotherapy, though that does not mean it is risk-free.
Why immunotherapy does not work for everyone
Here is where the story becomes complex.Doctors have seen cases where patients begin treatment with hope, only to see no improvement. Dr Rauthan shares one such case of a 57-year-old patient with advanced melanoma who did not respond despite receiving first-line immunotherapy.
So, what goes wrong?
There are several reasons:Immune desert: Some tumours lack enough T cells. Without these cells, there is nothing for immunotherapy to activate.Cancer camouflage: Tumour cells may stop expressing proteins that immune cells recognise.Immune suppression: Certain cells, like regulatory T cells, create an environment where immune activity is blocked.Rapid tumour growth: In some cases, cancer progresses faster than the immune system can respond.Dr Rauthan notes that failure is rarely due to a single factor. It is often a mix of tumour biology, immune response, and the patient’s overall condition.
Benefits that still make it worth considering
Despite its limits, immunotherapy remains one of the most promising tools in oncology.Key benefits include:Long-lasting responses in some patientsMore targeted action compared to chemotherapyPotential to treat advanced cancers where options were limitedThere is also growing interest in combining immunotherapy with other treatments. For example, pairing it with chemotherapy or targeted therapy can sometimes improve outcomes.The earlier-mentioned patient, after not responding, was shifted to a combination approach and showed clinical improvement. That highlights an important truth, treatment plans often evolve.
Risks, side effects, and the fine print
Immunotherapy is not a gentle cure-all.It can trigger immune-related side effects because the activated immune system may attack healthy tissues. Common issues include:Skin rashesFatigueInflammation in organs like lungs or liverIn rare cases, these reactions can become serious and require immediate medical care.Another challenge is cost and accessibility. Immunotherapy drugs are expensive and not always widely available.So, while the idea sounds simple, the decision to use it is anything but. 
While promising, it requires careful patient selection and often works best as part of a broader treatment strategy.
When is immunotherapy actually recommended?
Doctors do not prescribe immunotherapy for every patient.It is usually considered based on:Type and stage of cancerPresence of specific biomarkers (like PD-L1 expression)Patient’s overall healthPrevious treatmentsGuidelines from bodies like the National Cancer Institute and global oncology groups stress personalised care. That means no two treatment plans look the same.As Dr Rauthan puts it, immunotherapy is powerful, but not universal. Careful evaluation and timely reassessment remain central to good cancer care.
A changing future, not a final answer
Immunotherapy represents a shift in how cancer is understood. It moves the focus from destroying cancer to empowering the body.But it is not magic.The immune system is complex, and cancer continues to evolve. That ongoing battle is why research is still moving fast. New drugs, combinations, and biomarkers are being tested every year.Medical experts consultedThis article includes expert inputs shared with TOI Health by:Dr Amit Rauthan, HOD and Consultant, Medical Oncology, Immunotherapy, and Precision Medicine at Manipal Hospital, Old Airport Road, Bangalore.Inputs were used to explain how the immune system can be harnessed to fight cancer, how immunotherapy works, and why consulting a medical expert is crucial to determine when such treatments are appropriate.

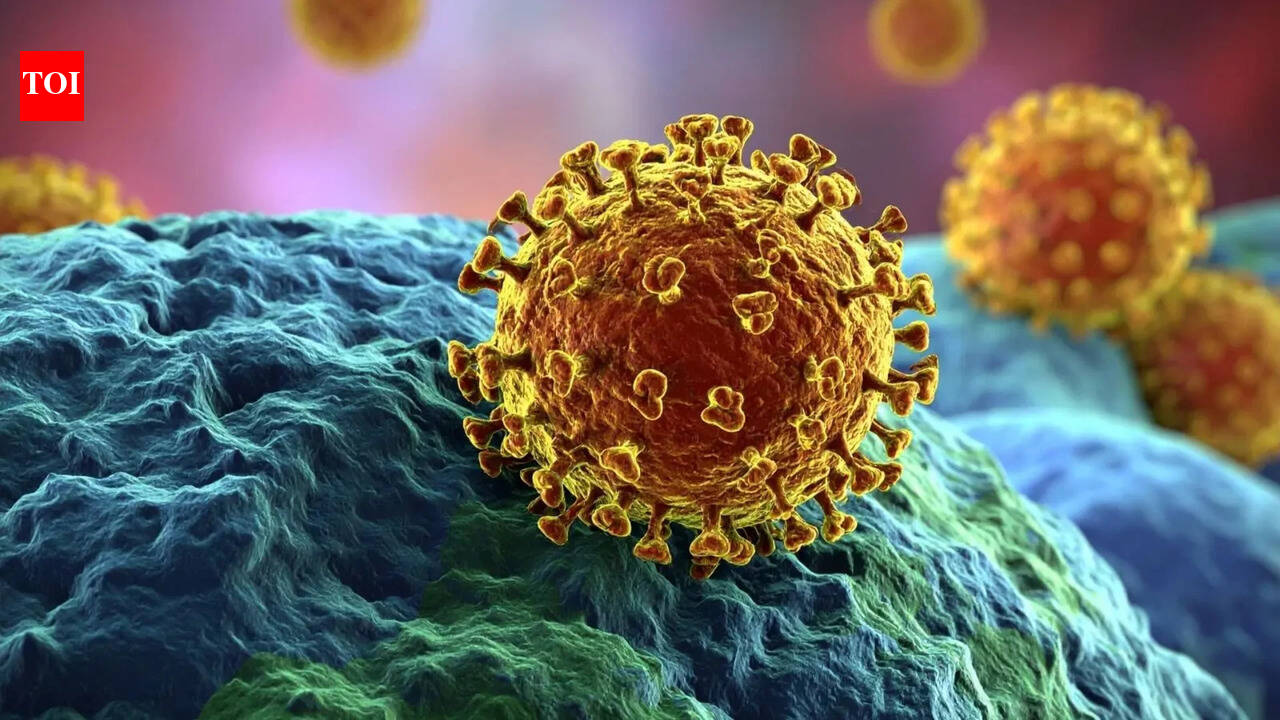

![[MBN] A Spring Herb Table to Restore Weakened Immunity A special remedy will be unveiled to tackle chronic fatigue and weakened immunity, the unwelcome guests of the changing seasons. On the program, Venerable Jeokmun, designated as Master No. 3 of Korean Buddhist temple cuisine, faces off in a spring herb cooking contest against "announcer-chef" Cho Woo-jong, who holds a licensed Western cuisine chef qualification. From spring cabbage bibimbap that has been selling out on social networking service (SNS) platforms to seasonal menus infused with the master’s secret techniques, the show presents a spring dining table that satisfies both the palate and health.](https://www.vitaminrush.com/wp-content/uploads/2026/03/20260331_01110129000004_L00-770x515.jpg)