As the rising popularity of herbal supplement use trickles down from adults to children and adolescents, there is a new question that pediatric nurse practitioners (NPs) should ask their patients: “What are you taking?”
Amanda Johnson, DNP, APRN, CPNP-AC/PC, acute care program director at Rush University, presented findings on herbal supplementation in pediatrics at the National Association of Pediatric Nurse Practitioners (NAPNAP) 47th National Conference on Pediatric Health Care held March 18 to 21, 2026, in Pittsburgh, Pennsylvania.
Dr Johnson discussed the rising rates of supplement use among children and adolescents and the clinical blind spots that can accompany it.
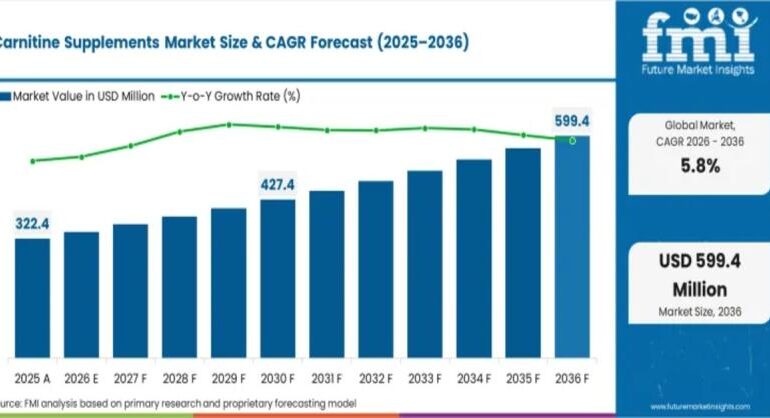
“Companies make over $90 billion selling supplements. It’s a big, mass production, and people are buying,” she said in an interview with The Clinical Advisor. “And if our adults are buying, our kids are also buying. Our adolescents and our school-aged children are seeing what their parents are buying. So, it’s an important conversation to start because they are getting exposed to it.”
Why Children Are Taking Supplements
Roughly 1 in 9 children in the United States has tried herbal supplements, Dr Johnson explained. The most common reasons why children and adolescents take supplements are for weight loss, bodybuilding, skin health, focus, gut issues, memory, or mental health support.
“They are seeing influencers describe what they’re taking, what it’s doing, how it’s improving, their ability to focus or sleep, and they glean on that,” Dr Johnson said. “And then they go to Walmart, Target, or the grocery store, and they buy the same product, hoping for the same response.”
This dynamic is compounded by marketing strategies that emphasize accessibility and the appeal of herbal supplementation. According to Dr Johnson, supplement advertising on social media online retail platforms reinforces the perception that “natural” products are inherently safe.
Many newer products, formulated as gummies, are targeted toward younger consumers, Dr Johnson noted.
Herbal Supplementation Safety in Children
Supplement-related adverse events contribute to an estimated 23,000 emergency department visits annually due to unintended consequences, according to Dr Johnson.
“Part of our job as nurse practitioners is to make sure that we’re asking those questions. Are they taking supplements? What supplements are they taking, and do we know the adverse side effects of those?” she said.
Yet clinicians may not always be equipped to answer those questions, according to Dr Johnson’s presentation. Historically, education on complementary and alternative medicine (CAM) has been limited in medical and nursing curricula. While about half of medical schools in the US now include some CAM-related coursework, the depth and consistency of training remain variable.
Under the Dietary Supplement Health and Education Act of 1994, dietary supplements are not regulated by the US Food and Drug Administration (FDA) in the same way as prescription medications. Manufacturers are responsible for ensuring product safety and accurate labeling, but they are not required to prove efficacy before marketing. In some cases, even the contents listed on labels may not precisely reflect what is in the bottle.
Part of our job as nurse practitioners is to make sure that we’re asking those questions. Are they taking supplements? What supplements are they taking, and do we know the adverse side effects of those?
There is no regulation on the amount of the plant in any given supplement, Dr Johnson explained. She added that herbal products may contain whole plants or only specific components such as roots or extracts.
Common Herbal Supplements
Echinacea is often marketed toward people who want to support their immune system. While some compounds in the plant have demonstrated anti-inflammatory and immune-modulating properties in laboratory studies, clinical evidence remains mixed, Dr Johnson said. A randomized controlled trial involving more than 700 participants found no significant difference between echinacea and placebo in treating the common cold, aside from a marginal reduction in symptom duration.
Ginkgo biloba has been studied for conditions ranging from cognitive impairment to attention-deficit/hyperactivity disorder (ADHD). While some evidence suggests it may enhance the effects of conventional ADHD medications, it has not shown efficacy as a standalone treatment. Additionally, it is linked to increased risk for bleeding, especially when used alongside anticoagulant or antiplatelet medications, Dr Johnson explained.
“Supplementation goes in and out of flavor for which one is trending. Right now, the one that’s selling the most in the states is turmeric or curcumin,” Dr Johnson said.
Despite its popularity and anti-inflammatory properties observed in preclinical studies, turmeric’s clinical benefits remain uncertain, she explained. Trials have produced inconsistent results, and its poor bioavailability limits its therapeutic potential.
While meta-analyses suggest that St John’s wort may be effective for mild to moderate depression in adults with outcomes comparable to some selective serotonin reuptake inhibitors (SSRIs), it is associated with several drug interactions, including with antidepressants, oral contraceptives, and anticoagulants, making unsupervised use potentially dangerous, Dr Johnson explained.
Topical use of arnica for pain and inflammation is common, but oral ingestion is not FDA-approved and can be toxic at high doses. Studies evaluating its effectiveness for post-surgical recovery have generally found no significant benefit, Dr Johnson stated.
Popularity of Herbal Supplements for Children
Beyond individual supplements, Dr Johnson emphasized the growing prevalence of combination products. These formulations, often marketed for “focus,” “immune health,” or “mood,” may contain multiple active ingredients in varying, sometimes unspecified, amounts, she explained.
“If you look at the supplements that are now available, they are combined supplements. They’re gummies, and they are trending towards our millennials and our adolescent populations because they have a very attractive appearance … and so those are the ones that most people are buying right now,” she said.
Especially because safety and efficacy data are particularly sparse in pediatric populations, this growing popularity raises concerns about dosing, interactions, and overall safety, Dr Johnson explained. At the same time, however, she did not recommend complete dismissal of herbal supplements for children.
Her goal, she said, is to encourage informed, shared decision-making between clinicians and patients. In addition to pediatric clinicians asking their patients about their supplement use, both higher-quality clinical trials and greater awareness of how supplements are portrayed on social media can help improve outcomes for children and adolescents who take herbal supplements, she concluded.
Visit Clinical Advisor’s conference section for more coverage of NAPNAP 2026.