A newly identified COVID-19 variant, Omicron subvariant BA.3.2, nicknamed “Cicada”, has drawn attention in global health discussions due to its unusually high number of mutations and potential to evade immunity. First detected in late 2024, the variant has since appeared across multiple continents and is being closely monitored by international health agencies. While early laboratory findings suggest increased immune escape, current evidence indicates that BA.3.2 does not cause more severe disease. However, we found that its characteristics warrant continued surveillance rather than immediate concern.
Social Media Posts
Multiple social media users shared a warning about a new COVID-19 variant, stating that the BA.3.2 subvariant, nicknamed the “Cicada” variant, has been detected in 23 countries, including the United States. The message says health authorities are closely monitoring the highly mutated strain, first identified in South Africa in late 2024, due to its unusual mutation profile and potential to partially evade immunity. It adds that symptoms remain similar to other Omicron subvariants and are generally mild in vaccinated individuals, with cough, fatigue, sore throat, runny nose, mild fever, and body aches most common.

Explainer
Virology and Lineage
BA.3.2 is an Omicron sublineage (Pango lineage B.1.1.529.3.2) that descends from BA.3, a relatively uncommon branch that appeared briefly early in the Omicron wave and then largely declined.
What makes BA.3.2 stand out is the amount of genetic change it carries. Genomic analyses suggest it has more than 70 spike-protein mutations relative to BA.3, and roughly 70 or more changes compared with earlier reference strains. Many of these changes sit in parts of the spike that help the virus attach to cells and avoid antibodies, especially the Receptor Binding Domain (RBD) and the N-Terminal Domain (NTD).
Some changes are also unusual. For example, BA.3.2 includes L452W, which is different from the more familiar L452R seen in other Omicron lineages, and it could affect the virus in different ways.
Beyond spike, BA.3.2 appears to have a large deletion of about 870 base pairs that removes the ORF7 and ORF8 genes. These genes have been linked to how earlier variants interact with the immune system, but what their absence means for BA.3.2 is still being investigated.
Phylogenetic analyses place BA.3.2 farther from other currently circulating Omicron lineages than expected, which suggests it may have evolved for a long time without being sampled. One hypothesis is that it emerged during a prolonged infection in a single host, although this has not been confirmed.
Global Epidemiology and Spread
BA.3.2 was first identified on November 22, 2024, in South Africa. It subsequently appeared in Mozambique, Europe, and other regions throughout 2025. By early 2026, it had been detected in at least 23 countries across all continents.
According to global surveillance data reported by the U.S. Centers for Disease Control and Prevention (CDC), BA.3.2 rose from approximately 0.2% of sequenced cases in mid-October 2025 to a peak of around 1.7% in early November before declining again. This suggests that while the variant spread internationally, it did not outcompete other circulating Omicron lineages.
Regional data indicate moderate presence in parts of Asia-Pacific, including Japan and South Korea, where it accounted for roughly 5–6% of sequences at certain points. However, it has not become dominant in any region.
The World Health Organization (WHO) has classified BA.3.2 as a “Variant Under Monitoring” (VUM), meaning it has genetic changes that may affect virus behavior but lacks clear evidence of increased risk.
Clinical Features and Severity
Current clinical data indicate that BA.3.2 causes symptoms similar to other Omicron variants. Reported cases include common upper respiratory symptoms such as sore throat, cough, fatigue, and fever.
Importantly, there is no evidence that BA.3.2 leads to more severe disease or higher mortality. In documented cases in the United States, including infections in older adults and a child, all patients recovered. Health authorities in Taiwan and other regions have similarly reported no increase in hospitalization or death linked to this variant.
Public health assessments from WHO and CDC consistently state that BA.3.2 does not appear to increase disease severity compared to existing Omicron strains. (Source)
Immune Escape and Vaccine Effectiveness
One of the main concerns surrounding BA.3.2 is its ability to evade immune responses. Laboratory studies show that antibodies generated from earlier infections or even recent vaccinations are less effective at neutralizing this variant.
A CDC-linked laboratory study found that sera from individuals vaccinated with updated 2025 formulations showed significantly reduced neutralization against BA.3.2 compared to other variants. Similarly, findings published in Virus Evolution indicate that BA.3.2 exhibits near-complete escape from antibodies generated before the Omicron era and partial escape even from newer vaccine-induced immunity.
Despite this, vaccines are still expected to protect against severe disease. WHO emphasizes that while breakthrough infections may increase, protection against hospitalization and death remains largely intact.
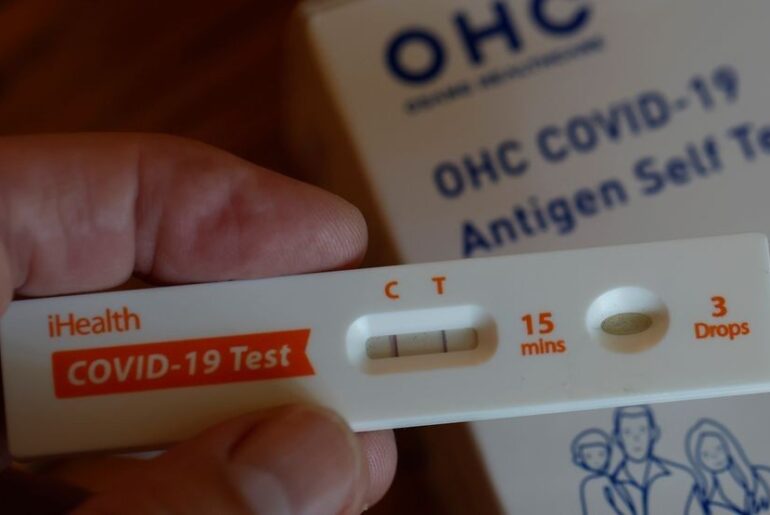
Diagnostics and Detection
BA.3.2 does not appear to compromise the performance of standard COVID-19 diagnostic tests. Current evidence indicates that commonly used multi-target PCR assays remain effective in detecting SARS-CoV-2 infections caused by this variant.
However, unlike the assumption that it cannot be flagged through PCR patterns, available genomic data suggest that BA.3.2 carries deletions in the spike protein, including the Δ69–70 deletion that has previously been associated with S-gene target failure (SGTF). This means that, in some PCR assays that include the S gene as a target, BA.3.2 may produce an SGTF pattern similar to earlier variants such as Alpha and Omicron BA.1.
That said, SGTF is not specific to a single variant and cannot be used to definitively identify BA.3.2. As with other emerging SARS-CoV-2 lineages, confirmation relies on genomic sequencing rather than PCR patterns alone. Public health agencies therefore continue to depend on sequencing and integrated surveillance systems, including wastewater monitoring, to accurately track the spread of BA.3.2.
Public Health Implications
At present, BA.3.2 has not triggered major policy changes. Health authorities, including WHO and CDC, have not recommended travel restrictions or new intervention measures specifically for this variant.
Instead, guidance remains consistent with existing COVID-19 strategies. Vaccination, especially booster doses for high-risk groups such as older adults and immunocompromised individuals, continues to be the primary defense. Surveillance systems are also being strengthened to monitor emerging variants more effectively.
WHO has stated that current vaccine formulations remain appropriate and that there is not yet sufficient evidence to justify updating vaccine composition specifically for BA.3.2.
Asia-Pacific Situation
In the Asia-Pacific region, BA.3.2 has been detected at low levels but has not become a dominant strain. Countries with strong genomic surveillance systems have reported sporadic detections, while overall COVID-19 trends remain stable.
Available reports indicate that governments in the region have not implemented BA.3.2-specific travel restrictions. Air travel and public health policies continue to follow standard COVID-19 protocols, reflecting the current assessment that the variant does not pose a significantly higher risk than other circulating Omicron lineages.
Health authorities in the region have instead emphasized continued monitoring, vaccination of high-risk populations, and maintaining existing preparedness systems rather than introducing new control measures.
Key Uncertainties
Despite increasing data, several uncertainties remain. The transmissibility of BA.3.2 is not yet fully understood, as it has not demonstrated a clear growth advantage over other circulating variants. Similarly, real-world vaccine effectiveness data, particularly against infection, remain limited, with most current evidence derived from laboratory studies rather than population-level observations.
The evolutionary pathway of BA.3.2 also remains uncertain. Its high number of mutations suggests it may have emerged through an atypical process, such as prolonged infection in a single host, although this hypothesis has not been conclusively confirmed.
Conclusion
BA.3.2 (“Cicada”) is a highly mutated Omicron subvariant that has spread internationally but remains a minority lineage. Current evidence indicates that it does not cause more severe disease and has not displaced other circulating variants. While immune escape may increase the likelihood of breakthrough infections, existing vaccines continue to provide protection against severe outcomes. Overall, BA.3.2 is being closely monitored, but it is currently assessed as posing a low additional public health risk rather than an immediate global concern.
Sources:
Evolution and Viral Properties of the SARS-CoV-2 BA.3.2 Subvariant
WHO TAG-VE Risk Evaluation for SARS-CoV-2 Variant Under Monitoring: BA.3.2
CDC reports COVID-19 variant case
New Covid Variant 2026: Cicada BA.3.2 Detected – What Travelers Need to Know

Title: BA.3.2 “Cicada” variant: detected internationally, some immune escape, no evidence of higher severity
Fact Check By: Pranpreeya
Result: Insight