Provided by Getty Images Bank
‘Placebo’ is a Latin word meaning “I shall please.” Today, it refers to the phenomenon where a patient’s condition improves after taking a fake drug, believing it to be real—a case of positive belief leading to actual therapeutic effects.
During the height of World War II in the 1940s, a shortage of painkillers led military doctors to administer saline solutions to wounded soldiers. Although saline has no pain-relieving properties, it was intended to provide psychological comfort. The soldiers, however, reported feeling actual pain relief. This is a classic example of the placebo effect.
Is the placebo effect real or just an illusion? Recent medical studies are focusing on placebos not as a coincidence but as a new therapeutic method.
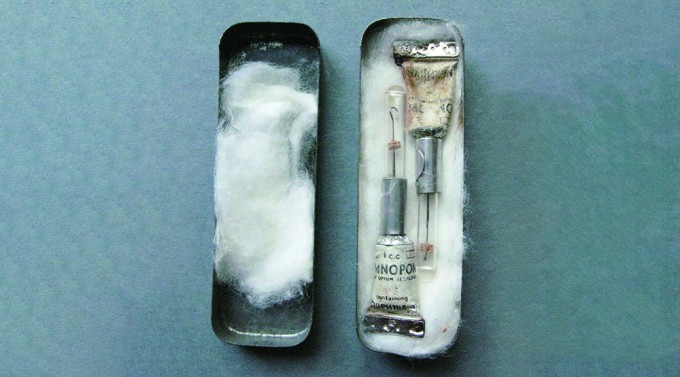
A morphine syrette issued to US troops during World War II. Morphine acts on endorphin receptors to stop the processing of pain, producing a powerful analgesic effect. Provided by the National Museum of the Royal New Zealand Navy
The first records of the placebo effect date back 300 years. In 18th-century Europe, a new treatment proposed by German physician Franz Anton Mesmer gained attention. He claimed that illnesses could be cured by controlling the fluid flowing through the human body with magnetic forces.
Mesmer’s treatment became popular, but the medical communities in Vienna and Paris, where he was active, criticized his theory. In 1784, figures like Benjamin Franklin and Antoine Lavoisier from the French Academy of Sciences launched an investigation using a blind test.
They blindfolded patients and had them drink what they were told was magnetized water, then pretended to manipulate their bodily fluids with magnets. The patients reported feeling therapeutic effects. This revealed that Mesmer’s magnetic therapy was nothing more than inducing self-suggestion in patients. Although Mesmer was discredited, the French Academy of Sciences’ report noted that “Mesmer’s treatment makes patients feel good.”
The placebo effect became a serious research topic about 170 years later. In 1955, Henry Beecher, a professor of anesthesiology at Harvard Medical School, published a paper after analyzing 15 clinical studies. He reported that patients with various diseases showed improved symptoms even after taking fake medicine. (doi: 10.1001/jama.1955.02960340022006)
Following Beecher’s research, which focused on the psychological factors behind the effectiveness of fake drugs, 21st-century science is now demonstrating how the placebo effect works through the brain.
● Pain Reduction by Placebo Verified Through Endorphin Secretion
In 2005, it was first proven that the placebo effect is a biochemical reaction in the brain. A research team led by Professor Jon-Kar Zubieta of the Department of Psychiatry at the University of Michigan confirmed that the placebo effect triggers the endogenous opioid system.
The endogenous opioid system is the brain’s self-made pain-relief system. “Natural painkillers” like endorphins and enkephalins bind to μ-opioid receptors in the brain, weakening pain signals and reducing the unpleasantness of pain.
The research team induced pain in 14 healthy young men by injecting saline into their jaws and then gave them both fake and real drugs while observing their brains using positron emission tomography (PET). PET imaging is used to track the process of specific neurotransmitters binding to receptors. As a result, the team confirmed that the placebo effect actually causes the secretion of endorphins. (doi: 10.1523/JNEUROSCI.3458-05.2005)
It was also confirmed that the placebo effect works by reducing factors that worsen pain while enhancing factors that help alleviate it. Two years later, in 2007, Tor Wager, then a professor of psychiatry at Columbia University who participated in this study, provided further evidence that placebos regulate the opioid system in different ways before pain and at the moment pain is inflicted. (doi: 10.1073pnas.0702413104)
When anticipating pain, placebos reduced the preparatory response of the pain-relief system, and when pain was present, they activated the opioid system. This means the placebo effect not only activates the pain-relief system when pain is present but also prepares for pain by reducing tension in the brain beforehand.
Provided by Getty Images Bank
● Placebo Effect Enhances Vaccine Immune Response
So, can the placebo effect be used strategically rather than relying on chance? In January 2026, an international collaborative research team including members from Tel Aviv University in Israel, Yale University in the U.S., and Princeton University in the U.K. published a study that could offer a hint. They confirmed that intentionally activating the mesolimbic pathway, a brain region associated with the placebo effect, can increase the vaccine immune response. (doi: 10.1038/s41591-025-04140-5)
The mesolimbic pathway is a circuit that becomes active when we receive a reward or expect to receive one. It is also linked to the placebo effect, which is based on expectation and belief.
Inside an MRI machine, the researchers had subjects view the activity of their own ventral tegmental area (VTA) in real time while recalling memories of trips, experiences of achievement, or imagining a pleasant future. This was intended to increase VTA activity. The VTA is the starting point of the mesolimbic pathway and sends dopamine signals to regulate motivation and behavior.
Afterward, the subjects were given a hepatitis B vaccine, and their antibody levels were measured after two and four weeks. The results showed that the people who consistently and effectively activated their VTA had a greater increase in antibodies that fight pathogens. Consciously generated positive expectations enhanced the vaccine’s immune response.
On January 29, Jung Min-young, a senior researcher at the Brain Development Imaging Research Center of the Korea Brain Research Institute, who reviewed the paper with us, explained, “There is prior research from animal experiments showing that activating the VTA boosts the immune system. This study intuitively demonstrates a causal relationship in the human immune system.”
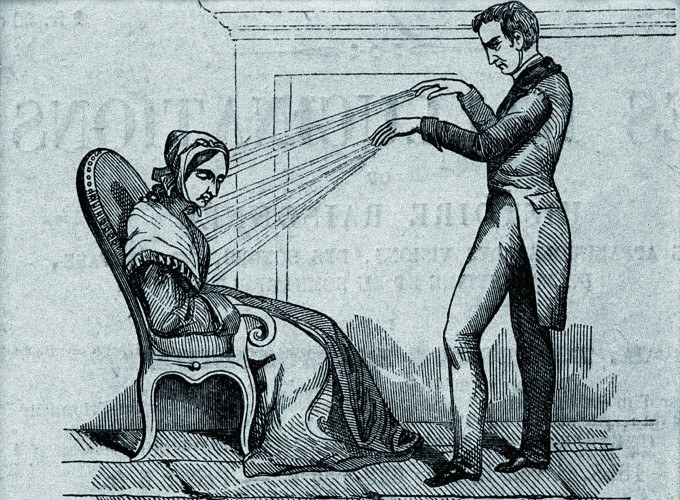
18th-century German physician Franz Anton Mesmer treats a patient using magnetism after having them ingest iron. His treatment was dismissed as a psychological factor based on suggestion, but today the placebo effect is being scientifically proven. Provided by Wellcome Collection(W)
● Will Pharmaceutical Companies Seek Out People More Susceptible to Placebos?
There are fields where the placebo effect, which can reduce pain and enhance a drug’s effectiveness through thought alone, is not so welcome. These are the medical and pharmaceutical industries, which treat patients and develop new drugs. For them, the placebo effect is considered noise to be managed and a problem to be solved. This is because when determining whether a newly developed drug is truly effective, the placebo effect should not interfere.
In 2016, a research team from Northwestern University’s Feinberg School of Medicine published a study in the international journal *PLOS Biology* revealing brain differences between people who are more and less responsive to placebos. (doi: 10.1371/journal.pbio.1002570)
It found that people with a stronger placebo effect have higher connectivity between the right middle frontal gyrus (r-MFG) and the rest of the brain.
The research team examined functional connectivity during the brain’s resting state, which is when a person has their eyes closed and is not thinking about anything in particular. They observed how connected the r-MFG was with other parts of the brain with minimal external input. It was found that individuals who experienced a stronger placebo effect showed a greater degree of connectivity activation in the r-MFG than those who did not.
The accuracy of predicting whether a person is sensitive or not to the placebo effect based on the activity of the r-MFG reached 95%. Researcher Jung explained, “The middle frontal gyrus is an area involved in visual attention. This suggests that people with a greater ability to shift their attention are more sensitive to placebos.”
Could people with high resting-state connectivity in the r-MFG be sought after by pharmaceutical companies? Researcher Jung said with a smile:
“Typically, when developing a new drug, if its effect is significant, the price is set high. If you could recruit trial participants who show a more dramatic effect than others when taking the drug, the drug’s effectiveness might appear better.”
However, current clinical trials for new drugs use the double-blind test (where neither the medical staff nor the patients know who is receiving the placebo) to minimize the placebo effect. If a person more sensitive to placebos participates in a trial and reports a better outcome after taking a placebo, such procedures would be rendered meaningless.
Researcher Jung noted that recently, placebos are being viewed as a new form of treatment. Modern medicine is moving beyond just understanding placebos to figuring out how to utilize them effectively. It remains to be seen whether the placebo will become a more sophisticated therapeutic tool.
※Related Article
Dong-A Science, April issue, Can Placebos Also Increase Vaccine Efficacy? The Science of Placebos
Copyright ⓒ DongA Science. All rights reserved.