(© syahrir – stock.adobe.com)
In A Nutshell
A Framingham study found that people with higher vitamin D levels around age 39 had lower tau buildup on brain scans about 16 years later.
It was an observational study, so it cannot prove that vitamin D caused the difference.
The link showed up for tau, an Alzheimer’s-related protein, but not for amyloid in this group.
The study followed adults who were dementia-free when they were scanned, which makes the finding interesting for early prevention research.
A blood test taken around age 40 might reveal clues about what’s happening inside the brain 16 years later, and vitamin D may be a vital part of the picture.
New research from the Framingham Heart Study has found that people with higher vitamin D levels in early midlife had less buildup of tau, a protein closely tied to Alzheimer’s disease, in their brains roughly a decade and a half later. The participants showed no signs of dementia when they were scanned. This isn’t about people who are already sick. It’s about seemingly healthy adults in their 30s and 40s whose vitamin D levels appear to be quietly linked to one of the earliest biological red flags for brain disease.
Most research connecting vitamin D to brain health has focused on older adults, typically people in their 60s and 70s already showing signs of cognitive trouble. This study took the opposite approach, looking at a much younger group and using advanced brain imaging to detect invisible changes long before symptoms ever appear. If the results hold up, they point to a wide window, spanning decades, during which something as accessible as vitamin D could help protect the brain.
How the Study Tracked Vitamin D and Brain Health
Researchers drew from the Framingham Heart Study’s third-generation group, a long-running project that tracks the health of families in the Framingham, Massachusetts area across multiple generations. The study included 793 participants, 53% women, who had their blood drawn between 2002 and 2005, when they were around 39 years old on average. Those blood samples were tested for levels of 25-hydroxyvitamin D, the standard measure doctors use to assess vitamin D status.
Between 2016 and 2019, a subset of these same participants came back for specialized brain scans. A total of 369 people received scans that detect tau protein buildup in the brain, and 424 received scans that detect amyloid plaques, another hallmark of Alzheimer’s disease. Both tau and amyloid are considered biological signatures of Alzheimer’s, though they develop at different stages. Tau tends to show up earlier, particularly in memory-related brain regions, while amyloid accumulates later across broader areas.
None of the participants had dementia, stroke, or other known neurological conditions at the time of their brain scans. The average gap between the initial blood draw and the brain imaging was about 16 years.

Your vitamin D levels in midlife may predict your cognitive health years later.(© jarun011 – stock.adobe.com)
What Vitamin D Levels Revealed About Alzheimer’s-Linked Proteins
After adjusting for a long list of factors that could muddy the results, including age, sex, blood pressure, smoking, diabetes, body mass index, depression, heart disease, and even the season when blood was drawn (since vitamin D levels fluctuate with sunlight exposure), the researchers found a clear pattern. Higher vitamin D levels at baseline were linked to lower tau buildup across the entire brain surface. The association also held when researchers looked specifically at the brain regions hit earliest by Alzheimer’s disease, including areas involved in memory and spatial awareness.
The connection survived multiple rounds of statistical adjustments and held up in additional analyses that excluded the small number of participants taking vitamin D supplements. When researchers also accounted for amyloid levels in the brain, the link between vitamin D and lower tau still remained.
However, vitamin D levels showed no connection to amyloid buildup. The researchers noted that tau tends to accumulate earlier than amyloid in the disease process, so in a younger group like this one, associations with tau might simply be easier to detect. The amyloid connection, if it exists, might only become apparent later in life.
About one-third of the participants, 146 people, had vitamin D levels below 30 nanograms per milliliter, a threshold that some experts consider the boundary of insufficiency. The average vitamin D level in the full group was 38 nanograms per milliliter. Only 22 participants were taking vitamin D supplements at baseline, likely reflecting their relatively young age.
When researchers divided participants into groups based on whether their levels fell above or below that 30-nanogram cutoff, the results were less clear-cut. The association between vitamin D and tau was strongest when vitamin D was treated as a sliding scale rather than a simple yes-or-no threshold. Exploratory analyses hinted at a dose-response pattern, with the highest vitamin D levels linked to the greatest reduction in tau, but the researchers cautioned that these additional analyses were preliminary.
There was no meaningful difference in the vitamin D and tau relationship between men and women, nor did carrying a gene variant called APOE e4, which is known to increase Alzheimer’s risk, change the results.

(Infographic generated by StudyFinds)
Why Vitamin D Might Matter for the Brain
Vitamin D receptors are found throughout the nervous system, including in the hippocampus, a brain region critical for memory. Vitamin D helps control inflammation and defend against a type of cellular damage tied to aging, both of which have been linked to tau buildup. Animal studies have shown that vitamin D deficiency can ramp up tau-related damage in the brain, while supplementation can reduce it. In one mouse study, feeding animals a vitamin D-deficient diet for 13 weeks led to increased tau buildup, greater clumps of amyloid, and more nerve cell death.
Clinical trials in humans have shown some promising, if mixed, results. In one trial of 183 older adults with mild cognitive impairment, daily vitamin D supplementation over 12 months significantly improved thinking abilities compared to a placebo. In another small trial of 82 healthy adults, a higher dose of vitamin D led to better visual memory performance, especially among those who started with low levels. And in a trial of 210 Alzheimer’s patients, vitamin D supplementation reduced blood markers related to amyloid while improving several measures of cognitive function.
A large pooled analysis covering 24 randomized controlled trials and more than 7,500 participants found that vitamin D supplementation had a small but meaningful positive effect on overall thinking ability, with stronger effects in people who were deficient to begin with.
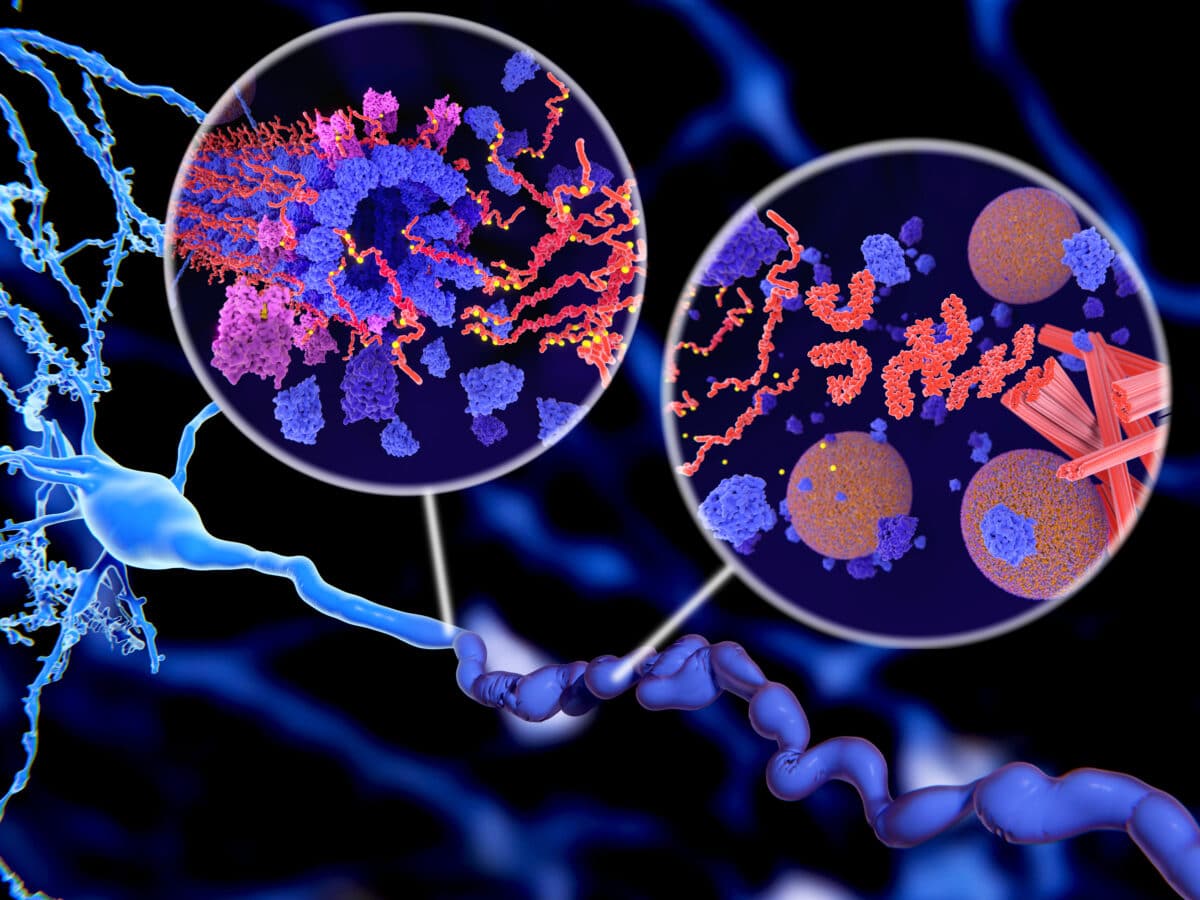
Alzheimer’s disease: Pathological Tau protein (red-orange) phosphorylation (yellow) leads to disintegration of microtubuli and aggregation to neurofibrillary tangles (orange) in a neuron axon. (Image by Juan Gaertner on Shutterstock)
What This Means for Vitamin D and Alzheimer’s Prevention
This study cannot prove that low vitamin D causes tau buildup. It is an observational study, meaning it can identify patterns but not definitively establish cause and effect. People with higher vitamin D might also exercise more, eat better, or spend more time outdoors, all factors that could independently benefit brain health. While the researchers adjusted for many of these variables, they acknowledged they lacked detailed information on lifetime physical activity, dietary habits, or time spent outdoors.
Other limitations include the predominantly white participant pool, which means the findings might not apply equally to other racial or ethnic groups. The researchers also had only a single vitamin D measurement per person, taken at one point in time, rather than tracking how levels changed over the years. And the relatively small number of participants with very low vitamin D levels, only 37 people fell below 20 nanograms per milliliter, made it difficult to study the effects of more severe deficiency.
Still, the study offers something that has been largely missing from the vitamin D and brain health conversation: evidence that the connection might begin forming decades before anyone notices a problem. Most dementia research focuses on the finish line, the point when memory loss is already underway. This work puts the starting line much earlier, in a period of life when intervention is far more practical. Whether boosting vitamin D in middle age can actually prevent or slow Alzheimer’s-related brain changes remains an open question that will need to be answered by clinical trials. But for now, the message is hard to ignore: what’s circulating in the blood at age 39 may quietly be writing the brain’s story at age 55.
Disclaimer: This study observed a link between vitamin D levels and a biological marker of Alzheimer’s disease, but it cannot prove that low vitamin D causes brain changes or that taking supplements will prevent dementia. The findings are preliminary and require confirmation through clinical trials before any specific health recommendations can be made. Readers should consult a physician before making changes to their vitamin D intake or supplementation.
Paper Notes
Limitations
This was an observational study and cannot establish a causal relationship between vitamin D levels and tau accumulation. Vitamin D was measured at a single time point, which may not reflect changes over the years and could introduce measurement error, though the researchers noted this would likely have weakened rather than strengthened the observed associations. The 10-to-17-year gap between blood sampling and brain imaging raises the possibility that participants’ vitamin D status changed during that interval due to lifestyle, dietary, or metabolic shifts. The study sample was predominantly Caucasian, limiting how broadly the results can be applied to other racial and ethnic groups. Only 37 participants had vitamin D levels below 20 nanograms per milliliter, preventing meaningful analysis at that lower deficiency threshold. Detailed information on lifetime physical activity, dietary habits, and time spent outdoors was not available, which could contribute to misclassification. Only 22 participants were taking vitamin D supplements at baseline, limiting the ability to analyze exogenous vitamin D intake.
Funding and Disclosures
The Framingham Heart Study is supported by the National Heart, Lung, and Blood Institute (contracts N01-HC-25195, HHSN268201500001, and 75N92019D00031) and by NHLBI grants R01 HL60040 and R01 HL70100. Additional support came from the National Institute on Aging (R01 AG054076, R01 AG049607, U01 AG049505, R01 AG059421, and P30 AG066546) and the National Institute of Neurological Disorders and Stroke (NS017950 and UH2 NS100605). The Irish Research Council (GOIPG/2023/5216) and the Health Research Board of Ireland (CSF-2020-011) also supported the research. None of the funding entities were involved in study design, data collection, analysis, interpretation, or the decision to submit the manuscript for publication. The authors reported no relevant disclosures. The article processing charge was funded by University of Galway.
Publication Details
Title: Association of Circulating Vitamin D in Midlife With Increased Tau-PET Burden in Dementia-Free Adults
Authors: Martin David Mulligan, Matthew R. Scott, Qiong Yang, Ruiqi Wang, Saptaparni Ghosh, Keith A. Johnson, Alexa S. Beiser, Sudha Seshadri, and Emer R. McGrath
Affiliations: School of Medicine, University of Galway, Ireland; The Framingham Heart Study, MA; Department of Biostatistics, Boston University School of Public Health; Boston University Chobanian & Avedisian School of Medicine; Department of Radiology, Massachusetts General Hospital; Department of Neurology, Massachusetts General Hospital, Harvard Medical School; Center for Alzheimer Research and Treatment, Brigham and Women’s Hospital, Harvard Medical School; Glenn Biggs Institute for Alzheimer’s & Neurodegenerative Diseases, University of Texas Health Sciences Center, San Antonio; HRB Clinical Research Facility, University of Galway, Ireland
Journal: Neurology Open Access, Volume 2, Number 2, June 2026
DOI: 10.1212/WN9.0000000000000057
Received: July 31, 2025. Accepted: December 3, 2025. Submitted and externally peer reviewed. Handling editor: Roy E. Strowd, III, MD, MEd, MS.