We’ve all heard the advice: eat your fruit and vegetables, get your vitamins, and stay healthy. For the most part, that guidance holds up. But some nutrients have a more complicated story, and vitamin B12 is a fascinating example.
Also known as cobalamin, B12 is essential for life. It helps the body produce red blood cells, keeps the nervous system functioning, and plays a central role in how cells copy and repair DNA.
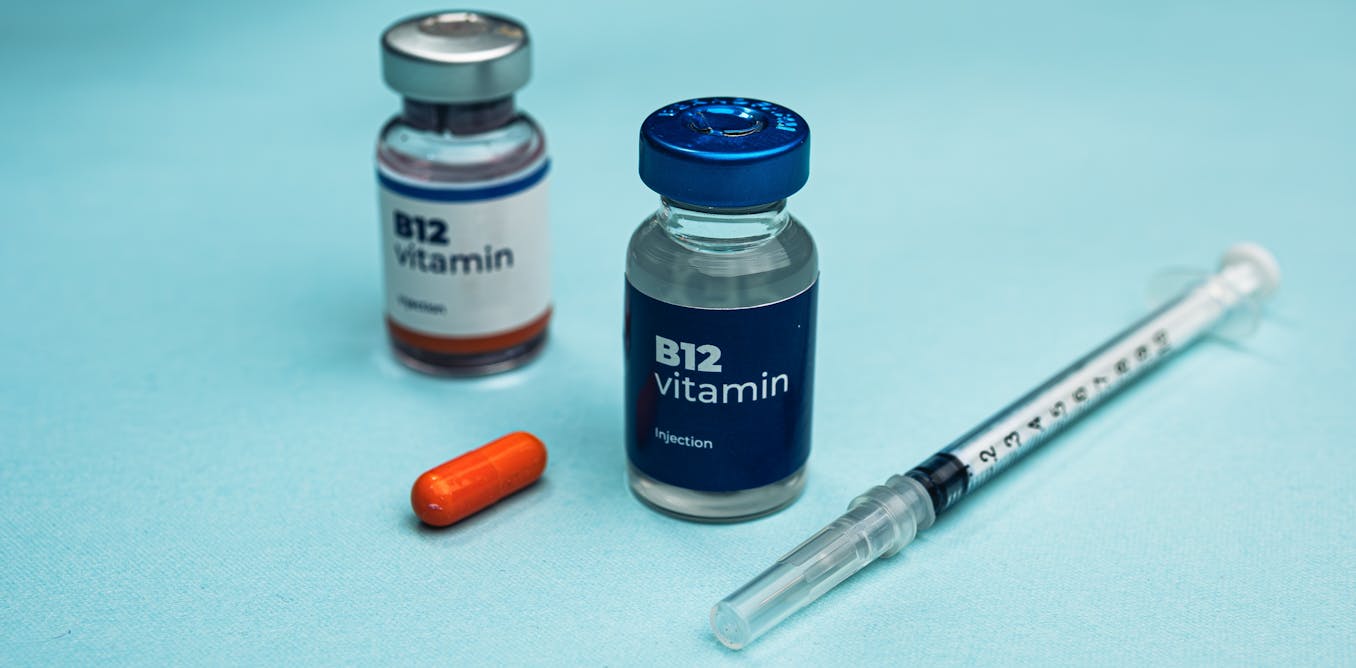
B12 is found naturally in animal products such as meat, fish, eggs, milk and cheese. Some cereals and breads are also fortified with it, helping people who do not eat meat get enough. Most people following a varied diet get the recommended amount, but vegans, people with certain gut conditions and older adults who absorb nutrients less efficiently may need supplements.

Most people can get sufficient vitamin B12 from their diet.
Tatjana Baibakova/Shutterstock
Without enough B12, things can go wrong, sometimes seriously, especially if deficiency is not recognised and treated. Yet in recent years, researchers have been asking whether high levels of B12 intake or high levels of B12 in the blood could be linked to cancer.
Staying balanced
The body is constantly making new cells. Every time a cell divides, it needs to copy its DNA accurately. Vitamin B12 is critical to that process. When levels are too low, DNA can be copied incorrectly, leading to mutations that, over many years, may increase the risk of certain cancers, particularly colon cancer. This is why B12 deficiency is taken seriously.
A 2025 case-control study from Vietnam found what researchers described as a U-shaped relationship between B12 intake and cancer risk, with both lower and higher intakes associated with increased risk. Because this kind of study can show an association but cannot prove cause and effect, the takeaway is not that B12 is dangerous. It is that balance matters.
It might seem logical that if B12 helps healthy cells thrive, taking extra doses should offer extra protection against cancer. But research does not fully support this. Vitamin B12 supports cell growth generally, not only the growth of healthy cells. One concern is that, if pre-cancerous cells are already present, very high availability of growth-supporting nutrients such as B12 could, in theory, support their growth too. But this remains difficult to prove in humans.
Overall, studies of high-dose B vitamin supplements taken over long periods have not shown clear protective effects against cancer incidence or cancer deaths. One analysis did report a reduced risk of melanoma, but this was a cancer-specific finding rather than evidence that high-dose B vitamins prevent cancer generally. Some observational research has also suggested a slight increase in lung cancer risk linked to long-term, high-dose B6 and B12 supplementation, particularly among men and smokers, although this kind of study cannot prove that the supplements caused the cancers.
Doctors have noticed that many cancer patients show unusually high levels of B12 in their blood. This raises an important question: does elevated B12 contribute to cancer, or can cancer itself cause B12 levels to rise?
Research in 2022 concluded that high B12 in cancer patients is often an “epiphenomenon”. In other words, the vitamin appears alongside the disease but does not necessarily trigger it. Further research from 2024 reached a similar conclusion.
This effect is thought to involve two main mechanisms. First, tumours can affect the liver, which stores large amounts of B12. When the liver is damaged or under strain, it may release more B12 into the bloodstream. Second, some tumours may increase proteins that bind to B12 in the blood. This can push blood test readings higher without necessarily meaning the body’s cells are receiving or using more B12.
Useful indication
Researchers are also recognising that elevated B12 may not be a cause of cancer, but it could be a useful marker of whether cancer is present or progressing. A large 2026 study found that colon cancer patients with very high B12 levels survived a median of around five years, compared with nearly eleven years for those with normal levels.
Similar patterns have been found in oral cancer and in patients receiving immunotherapy, where elevated B12 has been associated with poorer outcomes. This means that unexplained, persistent high B12, especially when it is not caused by supplements, should not be ignored. It may point to liver disease, blood disorders or an underlying cancer that has not yet been detected.
For most people, this is not something to worry about. B12 from a normal diet containing meat, fish, eggs, dairy or fortified foods is not usually the issue: it is very difficult to consume too much B12 from food alone. Deficiency remains a more common and better-established problem than excess.
The concern is prolonged high-dose supplementation without medical advice, or a blood test showing persistently high B12 when someone is not taking supplements.
The broader message is simple: more is not always better. Cancer cannot be prevented by loading up on any single vitamin. Long-term habits matter more: eating a balanced diet, exercising regularly, avoiding smoking, protecting your skin and attending routine health screenings.
So what about vitamin B12? Get enough through food or supplementation if you need it, especially if you are vegan, older or have a condition that affects absorption. But leave the megadoses on the shelf unless a doctor advises them. With B12, as with many nutrients, the goal is not as much as possible. It is the right amount.