If a second “novel coronavirus disease (COVID-19)” were to emerge, would we have to endure staying at home again while waiting for a vaccine?
A recent study published in the international journal ‘Science’ presents a completely different picture. Instead of precisely targeting a specific virus, it proposes creating a “universal vaccine” that strengthens the immune “resilience” of the lungs, enabling them to effectively fight even viruses encountered for the first time. We took a closer look with an expert to see if an era of preparing for various pathogens with a single nasal spray is possible.

In March 2020, people line up to buy government-supplied masks at a pharmacy in Incheon International Airport’s Terminal 1. Masks were the primary weapon for protecting public health before the COVID-19 vaccine was developed. Dong-A Ilbo
When the novel coronavirus disease (COVID-19) became a global pandemic in 2020, governments worldwide implemented city lockdowns or assembly bans to prevent the spread of infection. Pharmacies ran out of masks, and airplanes were grounded. The world had to wait for a COVID-19 vaccine to be developed.
However, a study on a “universal vaccine” published on February 19 in the international journal ‘Science’ by a team led by Professor Bali Pulendran of the Department of Microbiology and Immunology at Stanford University School of Medicine paints a future where, if humanity faces a second COVID-19, we would go to the pharmacy not for masks, but for a “universal spray” to use in our noses. (doi: 10.1126/science.aea1260)
● Boosting the Resilience of Trained Innate Immunity
On March 4, Professor Jo Nam-hyeok of the Department of Microbiology at Seoul National University College of Medicine, whom we met in his lab, began by calling Professor Pulendran’s team’s work an “interesting paper.” Professor Jo, an immunology researcher, explained, “Professor Pulendran’s team is a world-class research group in vaccine development,” and that this paper introduces the concept of a universal vaccine that prevents various diseases with a single shot.
First, let’s understand the concept of existing vaccines. Traditional vaccines create an acquired immune system that precisely recognizes and remembers specific antigens. This acquired immune system is called adaptive or acquired immunity.
When we are exposed to a specific antigen, such as the chickenpox virus, our body’s immune cells activate to eliminate the antigen and then most of them die. However, some cells called memory T cells and memory B cells survive for a long time, carrying the memory of the chickenpox virus. They are the protagonists of acquired immunity.
When they encounter the chickenpox virus again, they are immediately activated, proliferate rapidly in the early stages of infection, and mount a powerful immune response.
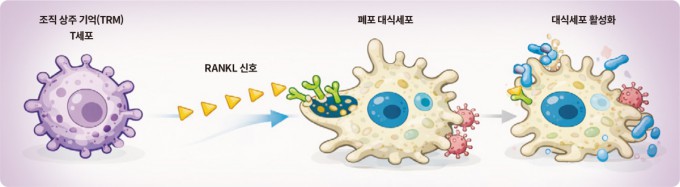
Bali Pulendran’s team at Stanford University School of Medicine revealed why innate immune cells like macrophages and neutrophils respond more strongly to a second stimulus after an initial one. Tissue-resident memory T cells secrete the RANKL protein, which keeps innate immune cells in an activated state. After elucidating this mechanism, the team developed a lipid nanoparticle vaccine that stimulates the innate immune system and confirmed in mouse experiments that trained innate immunity remained active for three months. Image generated by CHAT GPT
Existing vaccines help the body develop acquired immunity before actually contracting chickenpox by first introducing a weakened or dead chickenpox virus. This is similar to a police officer immediately recognizing and arresting a thief whose face is on a wanted poster. However, it cannot stop a thief who is not on the poster.
On the other hand, we also have immunity that we are born with: innate immunity (natural immunity). Innate immunity is a kind of first-line defense system that reacts in an antigen-nonspecific manner. It’s like arresting any unfamiliar face without considering their appearance. Macrophages and dendritic cells are active in innate immunity. Macrophages engulf pathogens, and dendritic cells present antigens to T cells.
“Previously, it was known that innate immunity does not have a memory response,” said Professor Jo. A memory response is an immune characteristic where the reaction to a second exposure to an antigen is faster and stronger. However, about 10 years ago, it began to be known that innate immunity also has a certain degree of ‘memory’.
For example, it was observed that individuals who had recovered from the flu virus showed increased immunity when later infected with a different pathogen, the COVID-19 virus.
This is called trained innate immunity. The universal vaccine targets this trained innate immunity. By elucidating the way innate immunity works, the research team has proposed a method to train a kind of ‘resilience’ enhancement capability.
Bali Pulendran, a professor in the Department of Microbiology and Immunology at Stanford University School of Medicine, is developing a vaccine that protects against various variants of SARS-CoV-2. Jack Kearse/Emory University
● The Key to a Universal Vaccine: Strengthen Innate Immunity
Professor Pulendran’s team first revealed the working principle of trained innate immunity, focusing on the lungs. There were three main elements.
The first is ‘Tissue-resident memory T cells’ (TRM) in the lungs. TRMs are memory T cells that settle in a specific organ and do not circulate. The respiratory, digestive, and reproductive tracts each have their own TRMs.
The second is the macrophage. Macrophages are cells that initiate innate immunity by engulfing all bacteria and viruses that enter from the outside, not just specific antigens. In particular, alveolar macrophages, which reside in the ‘alveoli’—the small air sacs where gas exchange occurs in the lungs—are the first to engulf pathogens that enter through breathing.
The last one, RANKL, is a signaling protein. It is a signal secreted by T cells and received by macrophages. When TRMs secrete the RANKL signal, alveolar macrophages detect the signal through the RANKL receptor.
Bali Pulendran, a professor in the Department of Microbiology and Immunology at Stanford University School of Medicine, is developing a vaccine that protects against various variants of SARS-CoV-2.
“The key is that macrophages that receive the RANKL signal remain in a more activated state,” Professor Jo said. “Before this study was published, the mechanism by which the trained innate immune response occurs was unknown, but Professor Pulendran’s team revealed that macrophages activated by the RANKL signal are better at engulfing various antigens that later enter the body.”
Next, the research team developed a vaccine in a lipid nanoparticle formulation. They then conducted experiments to investigate the immune response by administering it to mice. “They put two components that stimulate the innate immune system and the OVA antigen into the vaccine.”
The two components are GLA, a synthetic immune-stimulating substance, and 3M-052-LS, an immune-activating compound. These two substances help the trained innate immunity to work. The OVA antigen is the most commonly used experimental antigen in immunology, and in this experiment, it served to induce an immune response in the mice.
“The research team probably registered a patent for the combination of the immune-stimulating substance and the activating compound. They found the best combination to activate the innate immune system,” Professor Jo explained.
The experimental results showed that the trained innate immunity lasted for about 3 months. The team administered the ‘universal vaccine’ to the mice a total of four times at weekly intervals, and the effect lasted for 3 months from the day of the fourth vaccination.
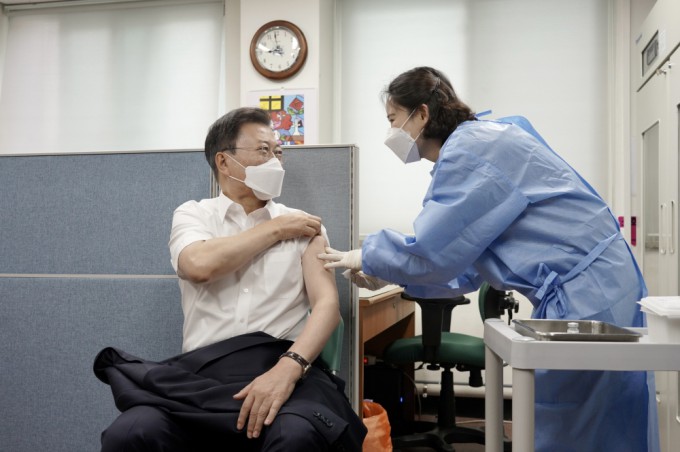
The emergence of a universal vaccine could change the course of future pandemics. On April 30, 2021, then-President Moon Jae-in receives his second dose of the COVID-19 vaccine at a public health center in Jongno-gu, Seoul. Dong-A Ilbo
● Will an Era of Lifelong Health from a Single Shot Arrive?
“So, will the era of a universal vaccine that can prevent not only the ever-changing flu each year but also a ‘second COVID-19’ with just one oral spray arrive?”
To this question, Professor Jo replied, “It’s possible, but the duration of the vaccine’s effect is not eternal.” Based on the results of Professor Pulendran’s team’s animal experiments, the effective period of the universal vaccine in the human body is expected to be about 1-2 years.
The short duration is an unavoidable limitation of the trained innate immune response. Even if the reactivity of innate immune cells is enhanced for a certain period, the state of the cells returns to its original state over time.
However, the period of 1-2 years could be extended. “The important thing is that this research is a starting point,” Professor Jo emphasized, pointing out that although there have been many studies to develop a ‘universal vaccine’ so far, statistically significant cases have been rare.
“While research has historically focused on specific diseases, the recent trend is to develop broad-spectrum therapies and universal vaccines. The funding priorities of the U.S. National Institutes of Health (NIH) are also changing.
Then, this time, they developed a universal vaccine with a statistically significant effect and identified the principle that this phenomenon is due to a trained innate immune response. Based on this, we can look forward to follow-up research to find ways to maintain trained innate immunity for longer.”
Furthermore, Professor Jo predicted that even if it’s not perfect, a universal vaccine will be necessary in a future where a second COVID-19 pandemic could occur. “It will definitely be useful when another new infectious disease emerges. Because we can strengthen the lungs’ resilience with a universal vaccine before a specific vaccine is developed.”
Before COVID-19 vaccinations began at the end of 2020, the cumulative global death toll had reached about 1.5 million. This was less than a year after the infectious disease had started to spread. The ‘superpower’ of a universal vaccine could change the game in pandemic response.
※ Related Article
Dong-A Science May issue, A second COVID-19, not scary? The emergence of a universal vaccine
Copyright ⓒ DongA Science. All rights reserved.