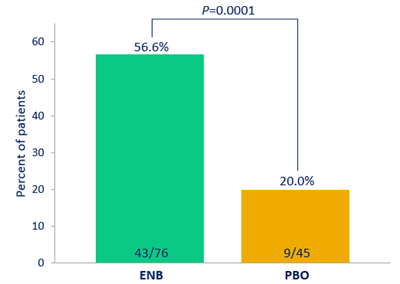
Urinary calcium excretion was normalised in 56.6% of patients who were hypercalciuric at baseline. Additional results through week 52 further support potential of eneboparatide to enable functional restoration of parathyroid hormone activity, including symptom and quality of life improvements, benefit to kidney function and preservation of bone health.
Positive results from the CALYPSO Phase III trial showed that eneboparatide (AZP-3601), an investigational parathyroid hormone (PTH) 1 receptor agonist, met its composite primary endpoint, demonstrating a statistically significant and clinically meaningful normalisation of albumin-adjusted serum calcium (sCa) levels and independence from active vitamin D and oral calcium supplements in adults with chronic hypoparathyroidism (HypoPT) at week 24. These late-breaking results were presented today at the European Congress of Endocrinology (ECE) in Prague, Czech Republic.1
In the trial, 31.1% of patients treated with eneboparatide met the composite primary endpoint, achieving sCa within normal range (8.3-10.6 mg/dL) and independence from oral supplements at week 24, compared with 5.9% of patients in the placebo group (eneboparatide: n=41/132; placebo: n=4/68; p=0.0001). Immunogenicity was observed in the majority of patients, resulting in reduced treatment effects in some patients. sCa was controlled with the aid of supplements and up-titration of eneboparatide.1
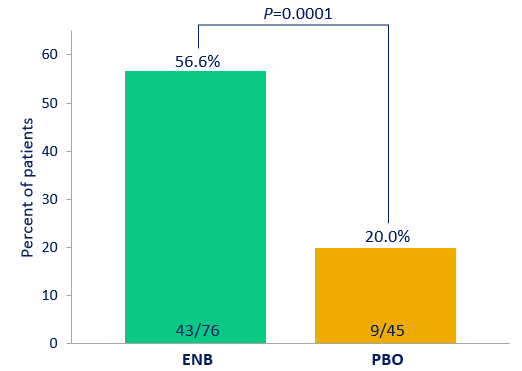
CALYPSO also met all key secondary endpoints at week 24, including normalisation of urinary calcium (uCa) excretion in patients with hypercalciuria at baseline. This was achieved in 56.6% of these patients in the eneboparatide group compared to 20% in the placebo group (eneboparatide: n=43/76; placebo: n=9/45; p=0.0001). Eneboparatide also demonstrated statistically significant improvements in patient-reported outcomes reflecting disease-specific core physical symptoms and physical functioning, as well as SF-36 Physical Function Subscore (SF-36-PFS).1
After week 24, patients continued eneboparatide (ENB/ENB group) or were switched to eneboparatide from placebo (PBO/ENB group) for an additional 28-week open-label extension (OLE) period. In the ENB/ENB group, clinical benefits were maintained through week 52 with some use of oral supplements, as assessed by OLE efficacy endpoints.1
Maria Luisa Brandi, MD, PhD, IRCCS European Institute of Oncology, Milan, Italy, and investigator in the trial, said: “As the underlying cause of HypoPT, inadequate PTH activity affects more than serum calcium levels, disrupting multiple body systems and significantly diminishing quality of life. The results from the CALYPSO Phase III trial demonstrate the potential for eneboparatide to stabilise serum calcium while preserving kidney and bone health, outcomes that are critical for improved patient functioning and successful long-term treatment.”
Gianluca Pirozzi, Senior Vice President, Head of Development, Regulatory and Safety, Alexion, AstraZeneca Rare Disease, said: “The breadth of data from CALYPSO, the largest global trial conducted in adults with HypoPT, demonstrates eneboparatide’s potential to deliver meaningful and sustained benefits in calcium regulation, symptom burden, physical function and bone health through functional restoration of PTH action. These effects were maintained through 52 weeks, supporting eneboparatide’s potential to address the broad burden of this complex rare disease and help close persistent gaps in care, given the limited treatment options available.”
Primary efficacy endpoint (composite) at week 241
Eneboparatide (ENB)
Placebo (PBO)
Percent of patients who met composite primary efficacy endpoint:
• Independence from active vitamin D; and
• Oral calcium ≤600 mg/day; and
• Albumin-adjusted sCa within the normal range (8.3-10.6 mg/dL)
31.1%
(n=41/132)
5.9%
(n=4/68)
p = 0.0001
Stable control of ADsCa over time1
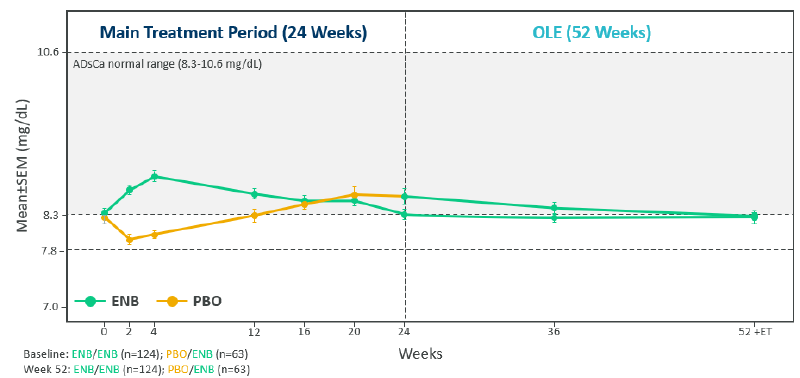
ADsCa, albumin-adjusted serum calcium; ENB, eneboparatide; ET, early termination; OLE, open-label extension; PBO, placebo; SEM, standard error of the mean
Key Secondary Endpoint: Normalisation of uCa in hypercalciuric patients at baseline at week 241
Bone health was preserved over 52 weeks, evidenced by increases in biomarkers procollagen type 1 N-terminal propeptide (P1NP) and C-terminal telopeptide (CTX) that remained within a normal range, consistent with balanced bone turnover, and no clinically significant reduction in bone mineral density (BMD), as measured by BMD T- and Z-scores.1
Eneboparatide was well tolerated over 52 weeks of treatment. The majority of treatment-emergent adverse events (TEAEs) were balanced between the eneboparatide group and the placebo group through week 24, and the overall safety profile remained consistent through week 52.1
Notes
Hypoparathyroidism
Hypoparathyroidism (HypoPT) is a rare endocrine disease caused by a deficiency of parathyroid hormone (PTH) and characterised by impaired regulation of calcium and phosphate, which can lead to a variety of neuromuscular, renal and skeletal manifestations.2,3 The primary cause in approximately 75% of people with HypoPT is injury to or removal of the parathyroid glands during neck surgery.3,4 There are more than 250,000 people in the US, EU5 and Japan living with HypoPT.5,6 Approximately 80% of people living with HypoPT are women, more than half of whom are peri- or postmenopausal and may be at increased risk of low bone mineral density or osteoporosis.6-9 Despite available treatments, people living with HypoPT continue to experience a significant unmet need.2,10
CALYPSO
CALYPSO is a global Phase III, randomised, double-blind, placebo-controlled, multicentre trial designed to evaluate the efficacy and safety of eneboparatide in adults with chronic hypoparathyroidism. The trial enrolled 202 patients treated with standard of care (active vitamin D and oral calcium supplementation) from 12 countries.11
Patients were randomised in a 2:1 ratio to receive once-daily subcutaneous injections of eneboparatide or placebo for 24 weeks. Patients received a starting daily dose of 20 µg of eneboparatide or placebo. Up-titration of eneboparatide could occur in 10-µg increments at least 7 days apart during the 20-week titration period, with a max dose of 100 µg. Oral supplements were progressively reduced, guided by serum calcium (sCa) until active vitamin D was eliminated, and oral calcium was ≤600 mg/day, when possible.11
The primary composite efficacy endpoint assessed the proportion of patients who achieved albumin-adjusted sCa within the normal range and independence from standard of care after 20 weeks of treatment and maintained it for four weeks on a fixed dose of eneboparatide. Key secondary efficacy endpoints included normalisation of 24-hour urinary calcium among patients with hypercalciuria at baseline, as well as patient-reported outcomes evaluating physical symptoms and quality of life.11
After the 24-week randomised main treatment period, patients on placebo were switched to eneboparatide and patients on eneboparatide remained on treatment for an additional 28 weeks (open-label extension). Patients who completed both treatment periods had the option to participate in a two-year long-term extension period and continue to receive eneboparatide. The long-term extension period is ongoing.11
Eneboparatide (AZP-3601)
Eneboparatide (AZP-3601) is an investigational parathyroid hormone (PTH) 1 receptor agonist being developed as a once-daily subcutaneous injection for the treatment of chronic hypoparathyroidism (HypoPT). It is designed to bind with high affinity to a specific conformation of the PTH receptor 1 with the aim of restoring PTH function to manage the symptoms of HypoPT while preserving kidney function and bone health. Eneboparatide has received fast track designation and orphan drug designation by the US Food and Drug Administration as well as orphan designation by the European Medicines Agency and the Ministry of Health, Labour and Welfare of Japan for the treatment of HypoPT.
Alexion
Alexion, AstraZeneca Rare Disease, is focused on serving patients and families affected by rare diseases and devastating conditions through the discovery, development and delivery of life-changing medicines. A pioneering leader in rare disease for more than three decades, Alexion was the first to translate the complex biology of the complement system into transformative medicines, and today it continues to build a diversified pipeline across disease areas with significant unmet need, using an array of innovative modalities. As part of AstraZeneca, Alexion is continually expanding its global geographic footprint to serve more rare disease patients around the world. It is headquartered in Boston, US.
AstraZeneca
AstraZeneca (LSE/STO/NYSE: AZN) is a global, science-led biopharmaceutical company that focuses on the discovery, development, and commercialisation of prescription medicines in Oncology, Rare Disease, and BioPharmaceuticals, including Cardiovascular, Renal & Metabolism, and Respiratory & Immunology. Based in Cambridge, UK, AstraZeneca’s innovative medicines are sold in more than 125 countries and used by millions of patients worldwide. Please visit astrazeneca.com and follow the Company on Social Media @AstraZeneca.
Contacts
For details on how to contact the Investor Relations Team, please click here. For Media contacts, click here.
References
Brandi ML, et al. The safety and efficacy of eneboparatide, a parathyroid hormone 1 receptor agonist, in adults with chronic hypoparathyroidism: a phase 3, randomized, placebo-controlled study (CALYPSO). Presented at the European Congress of Endocrinology; 2026 May 12; Prague, Czech Republic.
Bilezikian JP. Hypoparathyroidism. J Clin Endocrinol Metab. 2020;105(6):1722-1736.
Gafni RI, Collins MT. Hypoparathyroidism. N Engl J Med. 2019;380(18):1738-1747.
Shoback DM, et al. Presentation of hypoparathyroidism: etiologies and clinical features. J Clin Endocrinol Metab. 2016;101(6):2300-2312.
Hasegawa M, et al. Prevalence and characteristics of postoperative and nonoperative chronic hypoparathyroidism in Japan: a nationwide retrospective analysis. JBMR Plus. 2024;8(9):ziae100.
Vadiveloo T, et al. A population-based study of the epidemiology of chronic hypoparathyroidism. J Bone Miner Res. 2018;33(3):478-485.
Villarroya-Marquina I, et al. Influence of gender and women’s age on the prevalence of parathyroid failure after total thyroidectomy for multinodular goiter. Gland Surg. 2020;9(2):245-251
Deering KL, et al. Economic burden of patients with post-surgical chronic and transient hypoparathyroidism in the United States examined using insurance claims data. Orphanet J Rare Dis. 2024;19(1):164.
Khan A, et al. Skeletal health status among patients with chronic hypoparathyroidism: results from the Canadian National Hypoparathyroidism Registry (CNHR). Osteoporos Int. 2025;36:673-684.
Abate EG, et al. Review of hypoparathyroidism. Front Endocrinol (Lausanne). 2017;16(7):172.
ClinicalTrials.gov. Evaluation of the safety and efficacy of eneboparatide (AZP-3601) in patients with chronic hypoparathyroidism (CALYPSO). NCT Identifier: NCT05778071. Available here. Accessed May 2026.