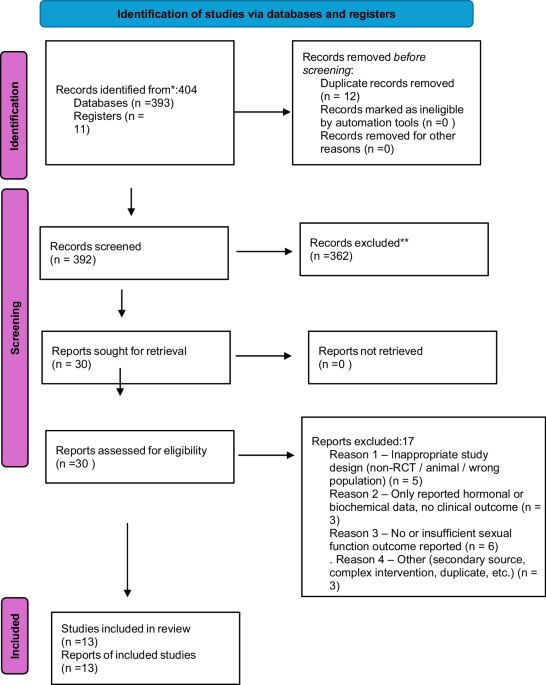
Hosseinabadi M, Khodadadi N, Tehrani H, Orooji A, Sany SBT. Sexual function and associated factors in postmenopausal women: a systematic review and meta-analysis. Health Sci Rep. 2025;8:e71270.
Daud WMW, Bajuri MY, Shuhaila A, Hatta S, Hassan MR, Norzilawati M. Sexual dysfunction among postmenopausal women. Clin Ter. 2014;165:83–9.
Monteleone P, Mascagni G, Giannini A, Genazzani AR, Simoncini T. Symptoms of menopause—global prevalence, physiology and implications. Nat Rev Endocrinol. 2018;14:199–215.
Simon J, Davis S, Althof S, Chedraui P, Clayton A, Kingsberg S, et al. Sexual well-being after menopause: an international menopause society white paper. Climacteric. 2018;21:415–27.
Paciuc J. Hormone therapy in menopause. Hormonal Pathology of the Uterus. Springer; 2020. p. 89–120.
Yoo TK, Han KD, Kim D, Ahn J, Park WC, Chae BJ. Hormone replacement therapy, breast cancer risk factors, and breast cancer risk: a nationwide population-based cohort. Cancer Epidemiol Biomarkers Prev. 2020;29:1341–7.
Davis JW, Weller SC, Porterfield L, Chen L, Wilkinson GS. Statin use and the risk of venous thromboembolism in women taking hormone therapy. JAMA Netw Open. 2023;6:e2348213.
Maas AH. Hormone therapy and cardiovascular disease: benefits and harms. Best Pract Res Clin Endocrinol Metab. 2021;35:101576.
Liu ZM, Ho SC, Woo J, Chen YM, Wong C. Randomized controlled trial of whole soy and isoflavone daidzein on menopausal symptoms in equol-producing Chinese postmenopausal women. Menopause. 2014;21:653–60.
Campos MG. Soy isoflavones. Handbook of Dietary Phytochemicals. Springer; 2021. p. 205–42.
Chalkidou A, Oikonomou E, Lambrinos D, Bothou A, Kyriakou D, Nikolettos K, et al. The comparative study of the administration of the combination preparation of Isoflavones and hyaluronic acid in menopausal women for the treatment of the symptoms of menopause, urogenital atrophy and osteoporosis in relation to existing hormone replacement therapies. Mater Sociomed. 2023;35:206.
Vitale DC, Piazza C, Melilli B, Drago F, Salomone S. Isoflavones: estrogenic activity, biological effect and bioavailability. Eur J Drug Metab Pharmacokinet. 2013;38:15–25.
Zhang J, Zhu Y, Pan L, Xia H, Ma J, Zhang A. Soy isoflavone improved female sexual dysfunction of mice via endothelial nitric oxide synthase pathway. Sex Med. 2019;7:345–51.
Lima SMRR, Bernardo BFA, Yamada SS, Reis BF, da Silva GMD, Galvão MAL. Effects of Glycine max (L.) Merr. soy isoflavone vaginal gel on epithelium morphology and estrogen receptor expression in postmenopausal women: a 12-week, randomized, double-blind, placebo-controlled trial. Maturitas. 2014;78:205–11.
Chaudhary D, Chaudhary S, Rajender G. A prospective study to investigate the 12-week efficacy of soy isoflavone vaginal gel (0.5%) in postmenopausal women with symptoms of vulvovaginal atrophy. J South Asian Fed Obstet Gynaecol. 2023;15:308–12.
Tranche S, Brotons C, Pascual de la Pisa B, Macías R, Hevia E, Marzo-Castillejo M. Impact of a soy drink on climacteric symptoms: an open-label, crossover, randomized clinical trial. Gynecol Endocrinol. 2016;32:477–82.
Jiménez I, Tirado R, Nava M, Angulo G, Medina J, Aguilar L, et al. Impact of phytoestrogen use on the quality of life of perimenopausal or postmenopausal women in Sinaloa, Mexico. Salud Cienc Tecnol. 2025;5:1095.
Kotsopoulos D, Dalais FS, Liang YL, McGrath B, Teede H. The effects of soy protein containing phytoestrogens on menopausal symptoms in postmenopausal women. Climacteric. 2000;3:161–7.
Nahas EA, Nahas-Neto J, Orsatti FL, Carvalho EP, Oliveira MLC, Dias R. Efficacy and safety of a soy isoflavone extract in postmenopausal women: a randomized, double-blind, and placebo-controlled study. Maturitas. 2007;58:249–58.
Ullman KE, Diem S, Forte ML, Ensrud K, Sowerby C, Zerzan N, et al. Complementary and alternative therapies for genitourinary syndrome of menopause: an evidence map. Ann Intern Med. 2024;177:1389–99.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71.
Heinemann LA, Potthoff P, Schneider HP. International versions of the menopause rating scale (MRS). Health Qual Life Outcomes. 2003;1:28.
Kupperman HS, Wetchler BB, Blatt MH. Contemporary therapy of the menopausal syndrome. JAMA. 1959;171:1627–37.
Shea BJ, Reeves BC, Wells G, Thuku M, Hamel C, Moran J, et al. AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. BMJ. 2017;358:j4008.
Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alonso-Coello P, et al. GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ. 2008;336:924–6.
Ribeiro AE, Monteiro NES, de Moraes AVG, Costa-Paiva LH, Pedro AO. Can the use of probiotics in association with isoflavone improve the symptoms of genitourinary syndrome of menopause? Results from a randomized controlled trial. Menopause. 2019;26:643–52.
Manonai J, Songchitsomboon S, Chanda K, Hong JH, Komindr S. The effect of a soy-rich diet on urogenital atrophy: a randomized, cross-over trial. Maturitas. 2006;54:135–40.
Upmalis DH, Lobo R, Bradley L, Warren M, Cone FL, Lamia CA. Vasomotor symptom relief by soy isoflavone extract tablets in postmenopausal women: a multicenter, double-blind, randomized, placebo-controlled study. Menopause. 2000;7:236–42.
Lipovac M, Chedraui P, Gruenhut C, Gocan A, Kurz C, Neuber B, et al. The effect of red clover isoflavone supplementation over vasomotor and menopausal symptoms in postmenopausal women. Gynecol Endocrinol. 2012;28:203–7.
Simpson EE, Furlong ON, Parr HJ, Hodge SJ, Slevin MM, McSorley EM, et al. The effect of a randomized 12-week soy drink intervention on everyday mood in postmenopausal women. Menopause. 2019;26:867–73.
Tedeschi C, Benvenuti C. Comparison of vaginal gel isoflavones versus no topical treatment in vaginal dystrophy: results of a preliminary prospective study. Gynecol Endocrinol. 2012;28:652–4.
Carmignani LO, Pedro AO, Montemor EB, Arias VA, Costa-Paiva LH, Pinto-Neto AM. Effects of a soy-based dietary supplement compared with low-dose hormone therapy on the urogenital system: a randomized, double-blind, controlled clinical trial. Menopause. 2015;22:741–9.
Kanadys W, Barańska A, Błaszczuk A, Polz-Dacewicz M, Drop B, Malm M, et al. Effects of soy isoflavones on biochemical markers of bone metabolism in postmenopausal women: a systematic review and meta-analysis of randomized controlled trials. Int J Environ Res Public Health. 2021;18:5346.
Sayahi M, Keramat A, Mohammadzadeh H. Is there a difference between the effects of phytoestrogens and non-phytoestrogens medicinal plants on sexual health? A systematic review and meta-analysis. Int J Reprod Biomed. 2023;21:881.
Trento SRSS, Madeiro A, Rufino AC. Sexual function and associated factors in postmenopausal women. Rev Bras Ginecol Obstet. 2021;43:522–9.
Hirose A, Terauchi M, Akiyoshi M, Owa Y, Kato K, Kubota T. Low-dose isoflavone aglycone alleviates psychological symptoms of menopause in Japanese women: a randomized, double-blind, placebo-controlled study. Arch Gynecol Obstet. 2016;293:609–15.
Basaria S, Wisniewski A, Dupree K, Bruno T, Song M, Yao F, et al. Effect of high-dose isoflavones on cognition, quality of life, androgens, and lipoprotein in post-menopausal women. J Endocrinol Invest. 2009;32:150–5.
Fontvieille A, Dionne I, Riesco E. Long-term exercise training and soy isoflavones to improve quality of life and climacteric symptoms. Climacteric. 2017;20:233–9.
Mucci M, Carraro C, Mancino P, Monti M, Papadia L, Volpini G, et al. Soy isoflavones, lactobacilli, Magnolia bark extract, vitamin D3 and calcium. Controlled clinical study in menopause. Minerva Ginecol. 2006;58:323–34.
Chedraui P, San Miguel G, Hidalgo L, Morocho N, Ross S. Effect of Trifolium pratense-derived isoflavones on the lipid profile of postmenopausal women with increased body mass index. Gynecol Endocrinol. 2008;24:620–4.