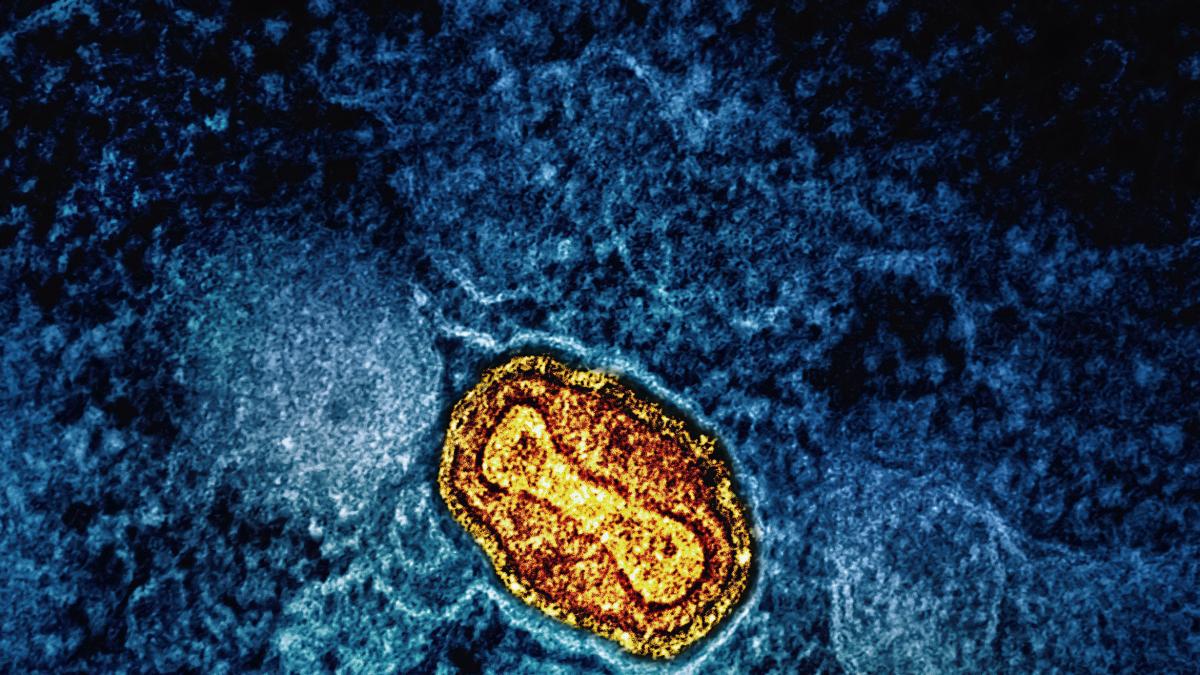
Few structures in the body are as complex and, at the
same time, as astonishing as the immune system. To mark the launch of the
CaixaResearch Institute, which is dedicated to the study of immunology, we
explore some of the stories, oddities and discoveries that reveal just how
extraordinary our defences truly are.
The first description of immunity
Long before the existence of microscopes, vaccines or
even a clear understanding of what infections were, some civilisations had
already observed that certain diseases were only experienced once, or that if
they returned, they did so in a much milder form. One of the earliest written
references to this phenomenon was made by the Athenian historian Thucydides. In
his account of the Plague of Athens in 430 BC, he noted that those who had
recovered from the disease were able to care for the sick because they did not
contract it again. That observation anticipated one of the fundamental
principles of immunology: the body’s ability to remember an infectious agent.
It would take almost two thousand years for that ancient intuition to become a
real medical tool, but the idea was already there, recorded in Antiquity.
 Scientists working at the National Cancer Institute in the 1930s.© National Cancer Institute, via Unsplash. Unsplash LicenseSmallpox: the
Scientists working at the National Cancer Institute in the 1930s.© National Cancer Institute, via Unsplash. Unsplash LicenseSmallpox: the
first time we learned how to protect ourselves
At the end of the 18th century, smallpox was one of
the deadliest diseases. In this context, the English physician Edward Jenner
took note of a common belief among milkmaids: those who had contracted cowpox, a
mild infection transmitted by cows, seemed to be protected against smallpox.
Intrigued by this observation, Jenner decided to put it to the test in 1798 by
carrying out an experiment that would change the course of medical history. He
inoculated a young boy with material taken from a cowpox lesion and later
confirmed that he was protected against smallpox. This experiment marked an
unprecedented breakthrough: for the first time, humanity was not merely
observing immunity, it was learning how to induce it deliberately.
 Edward Jenner performing his first vaccination on an 8-year-old boy named James Phipps on 14 May 1796.© Ernest Board, via Wikimedia Commons. Public domain
Edward Jenner performing his first vaccination on an 8-year-old boy named James Phipps on 14 May 1796.© Ernest Board, via Wikimedia Commons. Public domain Public health measures against a smallpox epidemic in New York. A Health Board inspector vaccinates homeless people at a police station.© The New York Public Library. New York City—Sanitary Precautions against a Smallpox Edpidemic— An Inspector of the Board of Health Vaccinating Tramps in a Station House. Public domain
Public health measures against a smallpox epidemic in New York. A Health Board inspector vaccinates homeless people at a police station.© The New York Public Library. New York City—Sanitary Precautions against a Smallpox Edpidemic— An Inspector of the Board of Health Vaccinating Tramps in a Station House. Public domain Edward Jenner, the British rural doctor who discovered the smallpox vaccine in 1796 and laid the foundations of modern vaccination.© Pierre Roch Vigneron, via Wikimedia Commons. Public domainHumanity has
Edward Jenner, the British rural doctor who discovered the smallpox vaccine in 1796 and laid the foundations of modern vaccination.© Pierre Roch Vigneron, via Wikimedia Commons. Public domainHumanity has
succeeded in eradicating a pathogen
The eradication of
smallpox remains, to date, a unique achievement. Following decades of mass
vaccination campaigns, epidemiological surveillance and international
cooperation, the last naturally occurring case of smallpox was recorded in
Somalia in 1977. Three years later, in 1980, the World Health Organisation officially declared the
disease eradicated. Never before had humanity succeeded in eliminating from
circulation a human pathogen of such impact. However, this success also has a
more troubling dimension: with the end of universal vaccination, the global
population has gradually lost its immunity to smallpox. For this reason,
although the virus no longer circulates naturally, it is still considered a
potential threat in scenarios involving accidents or bioterrorism.
The first vaccine
came from the cow
The word vaccine
has a much more literal origin than many people realise. It derives from the
Latin vacca, meaning “cow”, and refers directly to the pioneering work
of Edward Jenner, who used cowpox to immunise and protect people against
smallpox. Years later, Louis Pasteur built upon this legacy and expanded it. By
studying attenuated microorganisms – that is, those that have been deliberately
weakened – he observed that they could induce protection without causing severe
disease, and he chose to call this technique vaccination in honour of
Jenner. This work laid the foundations of modern immunology research and led to
the creation of leading scientific institutions such as the Pasteur Institute
in Paris, which remains one of the world’s most prestigious centres for the
study of infectious diseases and the development of vaccines.
Vaccinated individuals protect
those who cannot be vaccinated
So-called herd
immunity, also known as collective immunity, is one of the most
important concepts in public health. It occurs when a sufficiently large
proportion of the population becomes immune to an infection, either through
vaccination or prior exposure, making it more difficult for the pathogen to
find susceptible individuals to infect. As a result, transmission slows, and
those who cannot be immunised are indirectly protected. It is not a perfect
shield, nor does it work in the same way for all diseases, as it depends on
factors such as how contagious the pathogen is. Nevertheless, it represents a
highly effective collective barrier. Its importance lies in a fundamental idea:
protection is never purely individual, it is also communal.
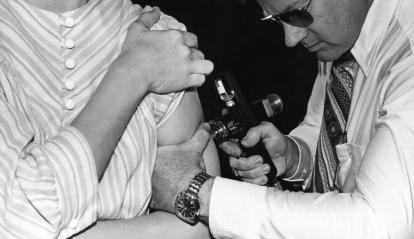 The instrument used by the doctor in the photograph was known as the “peace gun” because of its important role in global smallpox eradication campaigns. These devices used highly compressed air to deliver a jet of vaccine so fine that it penetrated the skin without the need for a needle.© Centers for Disease Control and Prevention (CDC), via Unsplash. Unsplash LicenseVaccine
The instrument used by the doctor in the photograph was known as the “peace gun” because of its important role in global smallpox eradication campaigns. These devices used highly compressed air to deliver a jet of vaccine so fine that it penetrated the skin without the need for a needle.© Centers for Disease Control and Prevention (CDC), via Unsplash. Unsplash LicenseVaccine
safety, backed by science
Despite the vast body of evidence accumulated, the
false link between vaccines and autism remains one of the most persistent
health myths. Its origin dates back to a study published in 1998 that suggested
a connection between the MMR (measles, mumps and rubella) vaccine and autism.
That study not only had a very small sample size and serious methodological
flaws, but was also ultimately retracted due to fraud, data manipulation and
conflicts of interest. Since then, numerous studies conducted in different countries,
involving hundreds of thousands of children and using far more robust designs,
have conclusively ruled out any link between vaccination and autism spectrum
disorders. The scientific consensus is unequivocal. What is concerning is that
this myth, despite being thoroughly discredited, continues to have real
consequences: it undermines confidence in vaccines, lowers vaccination rates
and contributes to the resurgence of preventable diseases that were once
thought to be under control.
Influenza
never stops changing
Unlike more stable pathogens, influenza viruses are
constantly changing. They do so through frequent mutations in their surface
proteins, particularly those recognised by the immune system. This means that
the defences developed against a previous strain may not be as effective
against variants circulating months later. For this reason, the influenza
vaccine is reviewed and updated each season based on the strains that,
according to international surveillance, are most likely to predominate that
year. Annual vaccination, therefore, is not due to a lack of effectiveness of
the vaccine, but rather to the ever-changing nature of the virus itself.
HIV, one of the most
complex virusesScanning electron micrograph (SEM) of an H9 T cell infected with HIV.© National Institute of Allergy and Infectious Diseases (NIAID)
HIV has an
extraordinary capacity to mutate, enabling it to change rapidly and evade
immune recognition. It also specifically targets key cells of the immune system
itself, weakening the body’s defences from within. In addition, it can
integrate itself into the genome of infected cells and remain hidden in
reservoirs for years, making it extremely difficult to eliminate. All of this
explains why, despite decades of intensive research, we still do not have a
fully effective preventive vaccine, although progress in this field continues
steadily.
Our mothers gave us immunity
Not all immunity is
acquired after contracting an illness or receiving a vaccination. There is also
passive immunity, which involves receiving antibodies already produced
by another organism. One of the most important examples occurs the relationship
between mothers and their children. During pregnancy, the mother transfers
antibodies to the foetus through the placenta, and after birth she can continue
to provide protection through breastfeeding. These antibodies provide the
newborn with a crucial temporary defence at a stage when their own protective
mechanisms are still immature.
The microbiota, a community that protects
us
An essential part of our health depends on living
alongside microbes. The human body hosts trillions of microorganisms (bacteria,
viruses, fungi and archaea) that form complex communities in the gut, skin,
mouth and other mucosal surfaces. This collective, known as the microbiota,
plays a role in digestion, produces useful compounds, contributes to metabolism
and plays a decisive role in the development and training of the immune system.
Exposure to these microorganisms helps our defences learn what should be
considered harmful and what should not, and when this balance is disrupted,
inflammatory, metabolic or allergic problems may increase. In other words, a part
of our defences is built through the constant dialogue with the microbes that
live within us.
Fever, pain and inflammation
are defence strategies of the body Before the development of antipyretic medicines, lukewarm water was used to reduce body temperature through evaporation.© British Museum, via Wikimedia Commons. CC BY-NC-SA 4.0
Before the development of antipyretic medicines, lukewarm water was used to reduce body temperature through evaporation.© British Museum, via Wikimedia Commons. CC BY-NC-SA 4.0
When someone has a
fever, muscle pain or inflammation, it is common to assume that all these
symptoms are caused directly by the invading pathogen. However, in many cases,
much of the discomfort actually comes from the body’s own immune response. When
an infection is detected, the body triggers a complex cascade of chemical
signals that coordinate the defence. Fever, for example, raises body
temperature to hinder the replication of many pathogens and enhance certain
immune functions. Similarly, inflammation helps recruit defensive cells and
direct them to the site of infection. In this way, what we experience as
illness is often the visible trace of a body actively fighting to protect
itself.
Our immunological arsenal can
fight against what does not yet exist
One of the most
remarkable characteristics of the immune system is its ability to anticipate
the unknown. This is possible because certain immune cells, such as B and T
lymphocytes, randomly generate millions of different receptors, each with a
slightly different shape, capable of recognising specific molecular structures.
Thanks to this vast diversity, the body has a repertoire ready to detect not
only known pathogens, but also entirely new ones. Rather than waiting to
encounter each threat and then designing a response from scratch, the body
maintains an immense library of possibilities already prepared for action.